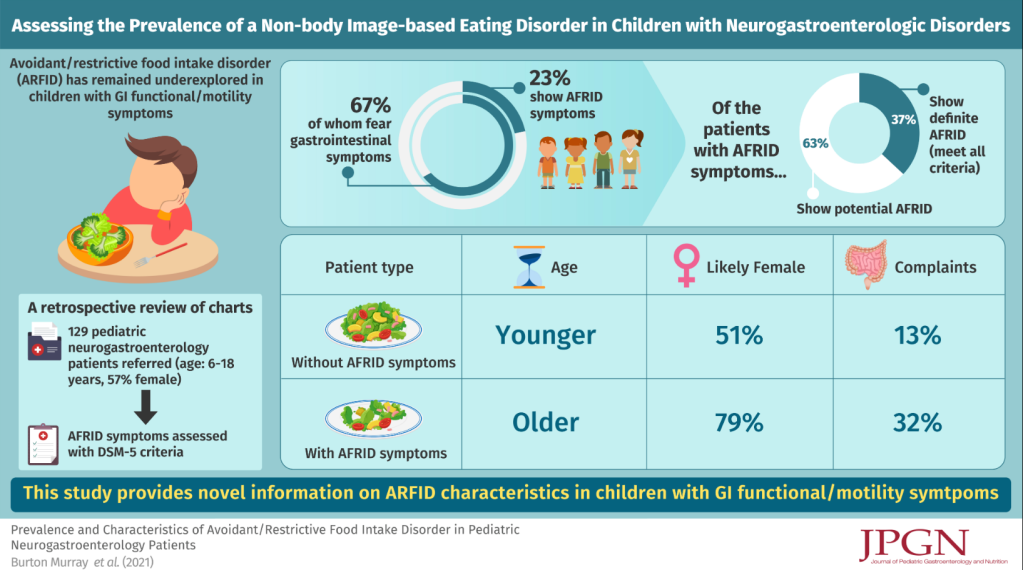
HB Murray et al. JPGN 2022; 74: 588-592. Prevalence and Characteristics of Avoidant/Restrictive Food Intake Disorder in Pediatric Neurogastroenterology Patients
Associated commentary by SB Oliveira, A Kaul: Invited Commentary Re: Prevalence and Characteristics of Avoidant/ Restrictive Food Intake Disorder in Pediatric Neurogastroenterology Patients
This was a retrospective study with 129 consecutive neurogastroenterology patients. Key findings:
- Eleven cases (8%) met the full criteria for ARFID (DSM, 5th ed) and 19 cases (15%) had clinically significant avoidant/ restrictive eating behaviors with insufficient information for a definitive ARFID diagnosis
- In a separate retrospective study, the same center published data on ARFID in a general pediatric population, showing 1.5% meeting the full criteria and 2.4% with some features (KT Eddy et al. Int J Eat Disord . 2015 Jul;48(5):464-70. Prevalence of DSM-5 avoidant/restrictive food intake disorder in a pediatric gastroenterology healthcare network)
The discussion notes that while elimination diets (eg. low FODMAPs diets) are frequently used for disorders of brain-gut interaction, they may increase the risk of ARFID. “Some children may develop fear of what will happen when they try foods again.”
The insightful commentary makes several useful points:
- A retrospective study is not the best way to determine prevalence of ARFID particularly as many practitioners have limited familiarity and documentation may be inadequate
- Nutritional rehabilitation can improve GI function. It has been shown that patients with anorexia nervosa have delayed gastric emptying which improved with refeeding. More broadly, it is often challenging to definitively determine the cause and effect in patients with malnutrition and gut dysmotility. (This is why I rarely obtain gastric emptying studies in patients with poor nutritional status)
My take: ARFID can be difficult to manage and is important to consider in our patient population, and probably even more so in patients seen in neurogastroenterology programs. The exact prevalence of ARFID in these programs is uncertain and prospective studies are needed.
Related blog post: