WJ Sandborn et al. NEJM 2021; 385: 1280-1291. Ozanimod as Induction and Maintenance Therapy for Ulcerative Colitis
This study led to FDA approval of ozanimod (Zeposia) in May 2021 for ulcerative colitis.
Mechanism of Action: Ozanimod is a selective sphingosine-1-phosphate receptor modulator which leads to internalization of S1P1 receptors in lymphocytes and the prevention of lymphocyte mobilization to inflammatory sites.
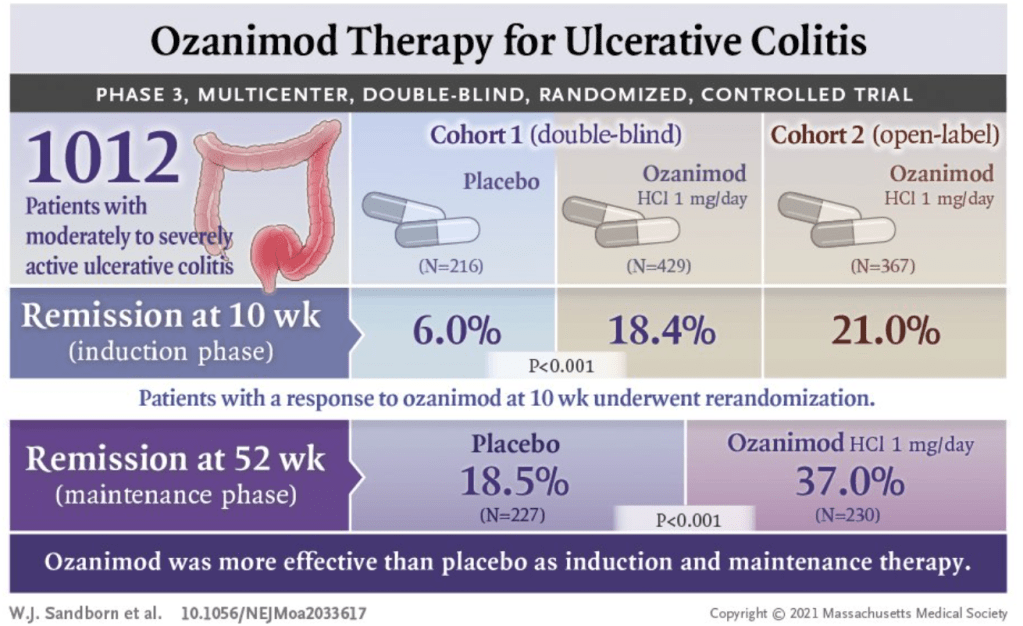
Design: There were two initial cohorts of adults with moderately to severely active ulcerative colitis. The first cohort (n=645) of this 52-week multicenter, randomized, double-blind, placebo-controlled trial (285 sites, 30 countries) of ozanimod as induction and maintenance therapy received either 1 mg of ozanimod hydrochloride once a day or placebo. A second cohort (n=457) received open-label ozanimod and was designed to assure that there would be adequate numbers of patients for the maintenance phase. The design allowed up to 30% of the first cohort to have received prior anti-TNF therapy and up to 50% of the second cohort to have received prior anti-TNF therapy. Ozanimod-treated patients with a clinical response during the 10-week induction were randomized again to a treatment group (n=230) or a placebo group for maintenance (n=227). Placebo-treated patients with a clinical response continued to receive placebo.
Approximately 97% of both cohorts had received prior aminosalicylate treatment and ~20% had received prior vedolizumab therapy.
As a safety measure (due to concerns of bradycardia), there was a 7-day period at the start of treatment with dose escalation, starting at 0.25 mg on days 1-4, 0.5 mg on days 5-7, then to 1 mg thereafter.
Key findings:
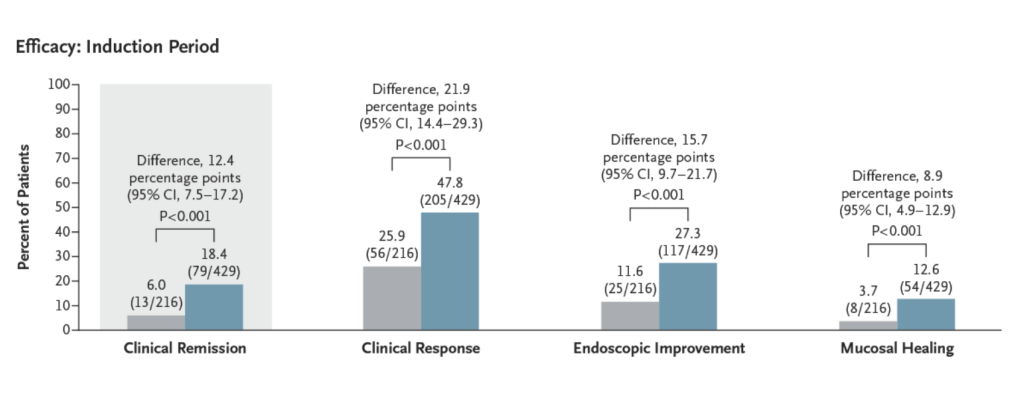
- The incidence of clinical remission was significantly higher among patients who received ozanimod than among those who received placebo during both induction (18.4% vs. 6.0%, P<0.001) and maintenance (37.0% vs. 18.5% [among patients with a response at week 10], P<0.001).
- The incidence of clinical response was also significantly higher with ozanimod than with placebo during induction (47.8% vs. 25.9%, P<0.001) and maintenance (60.0% vs. 41.0%, P<0.001).
- Histologic remission during induction, ozanimod vs placebo: 15.% vs 5.8%.
- A post hoc analysis showed decreases in the rectal-bleeding and stool-frequency subscores by week 2 (1 week after the completion of dose adjustment).
Safety Concerns:
- Serious adverse events attributed to ozanimod or placebo occurred in 4 (0.5%) and 2 (0.9%) during induction respectively and none and 1 (0.4%) respectively during maintenance.
- Overall all adverse events during induction occurred in 40% of ozanimod-treated patients and 38% of placebo recipients; during maintenance, adverse events were 49% and 37% respectively.
- Absolute lymphocyte count (ALC) decreased by a mean of ~54% from baseline to week 10 in ozanimod-treated patients; ALC was <200 in 1.1% (both cohorts) in induction and 17 patients during maintenance. None of the patients with ALC <200 experienced a serious or opportunistic infection.
- Serious infections associated wtih ozanimod or placebo occurred in 10 (1.3%) and 1 (0.5%) during induction respectively and 2 (0.9%) and 4 (1.8%%) respectively during maintenance.
- Common infections like nasopharyngitis and upper respiratory tract infections in 3-4% of ozanimod-treated patients compared to ~2% of placebo-treated patients
- Cancer: during induction there was one ozanimod-treated patient who had a basal cell carcinoma and during maintenance there was one ozanimod-treated patient who had a basal cell carcinoma. In the placebo group, during maintenance there was one patient who developed adenocarcinoma of the colon and one who developed breast cancer.
- Among ozanimod-treated patients, bradycardia was evident in 5 (~0.6%) during induction and none during maintenance. (Patients with significant cardiovascular history were excluded from trial)
- Among ozanimod-treated patients, hypertension occurred in 13 (~1.6%) during induction and 4 (1.7%); in the placebo group, none in the induction period and three (1.3%) in the maintenance had hypertension.
- Prior to entry, the trial required documented varicella zoster IgG antibody or completion of vaccination. Still, HSV occurred in 3 during induction (~0.5%) and 5 (2.2%) during maintenance (only 1 placebo patient (0.4%) had an HSV infection during maintenance.
- Elevated liver tests associated wtih ozanimod or placebo occurred in 42 (5.3%) and 2 (0.9%) during induction respectively and 32 (13.9%) and 1 (5.3%%) respectively during maintenance.
- Macular edema was noted in 2 ozanimod-treated patients during induction and 1 during maintenance.
My take: This study shows that ozanimod was more effective than placebo in adults with moderately to severely active ulcerative colitis. It will probably be years before we have adequate pediatric data.

Pingback: Favorite Posts of 2021 | gutsandgrowth