SH Ibrahim et al. Hepatology 2022; 75: 1627-1646. Cholestatic liver diseases of genetic etiology: Advances and controversies
Table 1 lists more than 40 monogenic disorders of cholestasis. Examples:
- Disorders of membrane transporter or polarity: PFIC1, PFIC2, PFIC3, Dubin-Johnson
- Basolateral disorders: NTCP deficiency, Rotor syndrome, Organic solute transporter deficiency
- Disorders of nuclear receptors: PFIC5
- Disorders of intracellular trafficking: Arthrogryposis-renal dysfunction-cholestasis, PFIC6 microvillous inclusion (MYO5B gene), Osteo-oto-hepato-enteric, Fanconi renotubullar syndrome
- Disorders of cytoskeletal and tight junction protein: PFIC4, Neonatal ichthyosis sclerosing cholangitis
- Cholangiopathies-Ciliopathy: Neonatal sclerosing cholangitis, Nephronophthisis, Meckel-Joubert syndrome, renal cysts and diabetes syndrome, BASM
- Cholangiopathies-Bile duct paucity: Alagille
- Cholangiopathies-cholangiocyte channelopathy: Cystic Fibrosis
- Hepatocellular disease: A1AT deficiency, mitochondrial depletion, mitochondrial translation defect, transaldolase deficiency
- Inborn errors of metabolism -bile acids: BASD, bile acid conjugation defects, peroxisomal defects
- Inborn errors of metabolism -carbohydrates: galactosemia, hereditary fructose intolerance
- Inborn errors of metabolism -amino acids: tyrosinemia type 1
Key Points:
- Low GGT genetic disorders (>25 genetic mutations) include canalicular transporter defects, basolateral transporter defects, intracellular trafficking defects, defects of cytoskeletal and tight junction protein, transaldolase deficiency, bile duct paucity, and inborn errors of metabolism.
- The authors note that the timing and utility of a liver biopsy is changing due to the advent of rapid molecular testing.
- Potential treatments are reviewed include ursodeoxycholic acid, IBAT inhibitors, cholic acid, biliary diversion, and liver transplantation.
- Multidisciplinary evaluation is often needed in patients with Alagille. 87% have cardiac anomalies, up to 36% have/develop cerebral vasculopathy, 21% develop post-transplant renal dysfunction, and 22% develop spontaneous or procedure-associate systemic bleeding (need for hematology consultation). In addition, pathologic fractures are common; one report found the rate of femur fractures was 50 times that in the general population which is likely related to intrinsic bone defects (as well as cholestasis).
My take: With the widespread availability of genetic testing which is needed due to the numerous etiologies, the diagnosis of ‘idiopathic’ chronic cholestasis has decreased and targeted therapies have emerged.
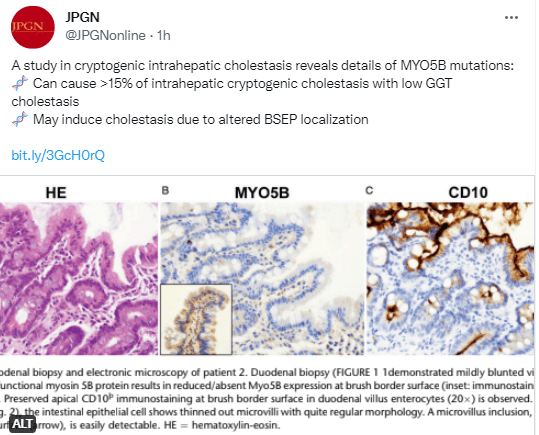
Related article: L Matarazzo et al. JPGN 2022; 74; p e115-e121. MYO5B Gene Mutations: A Not Negligible Cause of Intrahepatic Cholestasis of Infancy With Normal Gamma-Glutamyl Transferase Phenotype
Key finding:
In this multicenter retrospective and prospective study was conducted in 32 children with cryptogenic intrahepatic cholestasis, whole exome sequencing identified 6 with MYO5B mutations. The most common signs were pruritus, poor growth, hepatomegaly, jaundice, and hypocholic stools.
Related blog post:
