S Nagula et al. Clin Gastroenterol Hepatol 2024; DOI:https://doi.org/10.1016/j.cgh.2023.10.034. Open Access! AGA Clinical Practice Update on High-Quality Upper Endoscopy: Expert Review
The summary with nine “best practice advice” statements is not very helpful. However, Figure 2 and Table 1 are very useful.
From Figure 2 -not shown below (but in article) are Prague classification for Barrett’s and EREFS for eosinophilic esophagitis. The remaining parts of this figure include the Los Angeles classification for erosive esophagitis, the Hill classification of the gastroesophageal flap, and the Forrest classification of peptic ulcers:
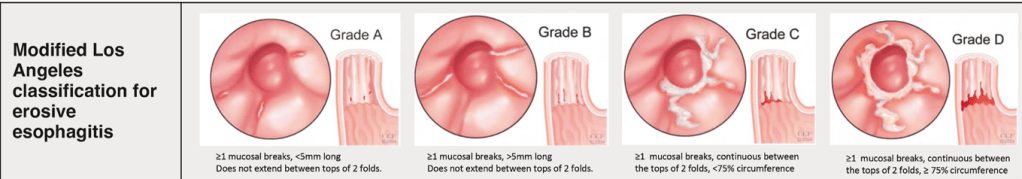
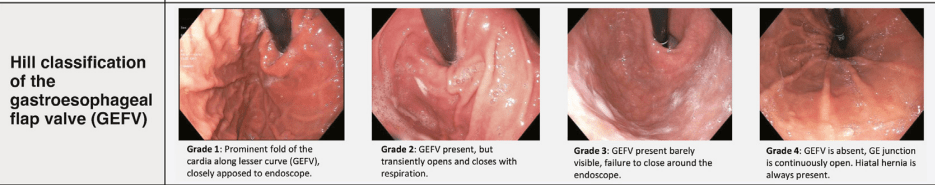
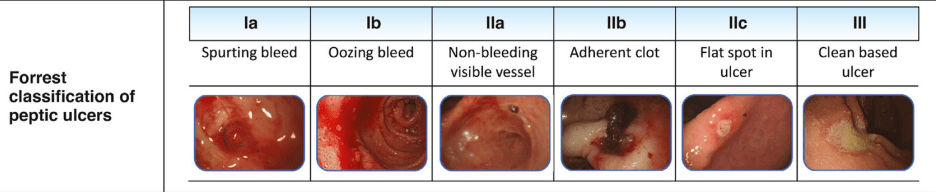
From Table 1:



Table 1 also gives guidance for biopsies with peptic ulcer disease, Barrett’s esophagus, gastric preneoplasia, and for gastric polyps.
My take: When suspicious of underlying disease, this article recommends taking more biopsies and in more jars.
Related blog posts:
- PEnQuIN and Improving the Quality of Pediatric Endoscopy
- 2023 ACG Celiac Guidelines for Adult and Children
- “When is Celiac Disease Celiac Disease?”
- Ultra-Short Celiac Disease
- How Useful Are 3-site Esophageal Biopsies for Eosinophilic Esophagitis
- 4-14-4 Rule: More Biopsies Needed For Eosinophilic Esophagitis
- Best Approach for Identifying Eosinophilic Esophagitis Prior studies have shown higher yield when taking 5 or 6 biopsies rather than fewer biopsies; thus, the location of biopsies may not be as important as the number of specimens. Also, prior studies have shown that having another pathologist review the slides can increase the yield by ~20%; this indicates that careful review of specimens by itself is helpful. Perhaps, more specimen containers will increase the time that a pathologist reviews the biopsies.
- Looking Twice for Eosinophilic Esophagitis
- GI Bleeding -Forrest Classification
