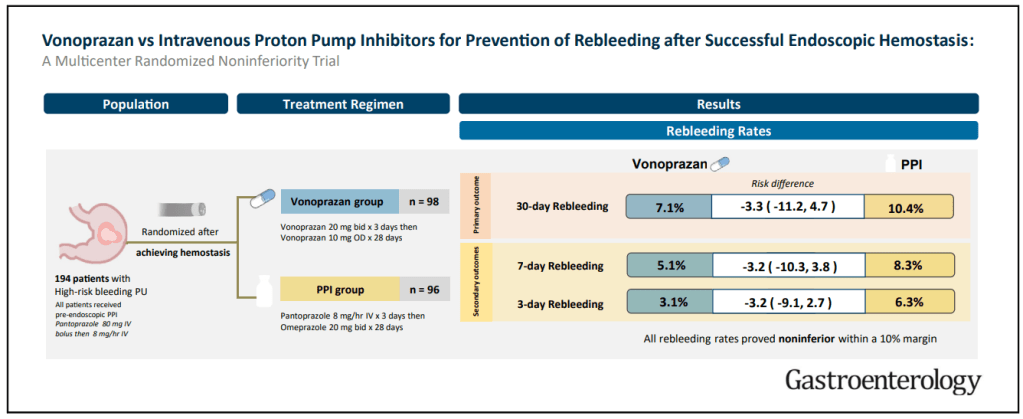
T Geeratragool et al. Gastroenterol 2024; 167: 778-787. Open Access PDF! Comparison of Vonoprazan Versus Intravenous Proton Pump Inhibitor for Prevention of High-Risk Peptic Ulcers Rebleeding After Successful Endoscopic Hemostasis: A Multicenter Randomized Noninferiority Trial
All patients received IV PPI treatment prior to endoscopy. Key finding from this multicenter randomized open-label adult trial:
- The 30-day rebleeding rates in vonoprazan and PPI groups were 7.1% (7 of 98) and 10.4% (10 of 96), respectively
- There were similar outcomes with regard to safety and secondary outcomes
My take: This study shows that oral vonoprazan is not inferior to IV PPI treatment for high-risk peptic bleeding ulcers. Perhaps, a study with more participants would show superiority of vonoprazan given the absolute lower rebleeding rates in this study.
Related blog posts:
- Improved Efficacy with Vonoprazan for Severe Esophagitis
- Why Vonoprazan Is More Effective For Erosive Esophagitis Than a Proton Pump Inhibitor
- Understanding FDA Approval of Vonoprazan-Based Therapies for Helicobacter Pylori
- Safety and Efficacy of Potassium Competitive Acid Blockers (3 Studies)
- All Bleeding Stops (part 2)
- All bleeding stops



