Tweets only this week.
Category Archives: Health Economics
Tweet Week -Health Coverage & Pre-existing Conditions + IBD Tweets
Tweet Week -Preexisting Conditions Before (? and After) Affordable Care Act
NEJM Presidential Candidate Health Proposals
Full text: My Vision for Universal, Quality, Affordable Health Care –NEJM
From NEJM: The editors invited the Democratic and Republican presidential nominees, Hillary Clinton and Donald Trump, to answer the following question for Journal readers: What specific changes in policy do you support to improve access to care, improve quality of care, and control health care costs for our nation? Secretary Clinton responded. Mr. Trump did not respond.
The main topics in Hillary Clinton’s commentary include expanding insurance coverage through the affordable care act (i.e. Obamacare), improve affordability in health care with proposals that affect both insurance companies and pharmaceutical companies, improve access to primary care/community care, and to continue to promote innovation/research.
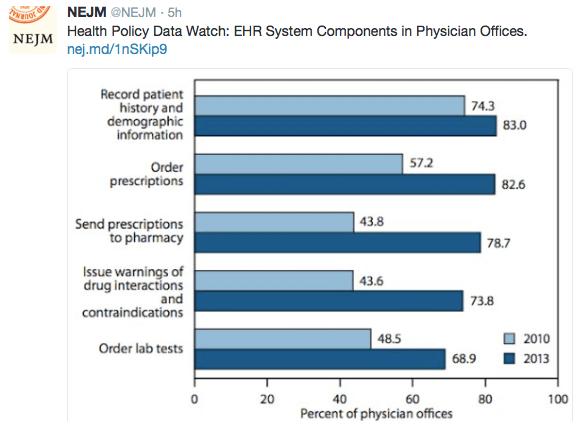
Image Only: EMR Uptake
Image
NEJM: Generic Drug Price Increases
Image
Is Obamacare Causing Skyrocketing Premiums?
Not yet according to a recent commentary: BD Sommers. NEJM 2016; 375: 201-3. The graph below provides some perspective. In addition, the author cautions those who have voiced early alarm bells regarding upcoming rates. He notes the same alarms have been raised in the previous 2 years. Though, he notes, “there are reasons to suspect that marketplace premium growth for 2017 will exceed this year’s levels. Two of the law’s provisions designed to reduce financial risk to insurers in the new markets expire after 2016 — the risk corridor and reinsurance provisions…the country’s continued emergence from the aftermath of the Great Recession may well spur increasing rates of health care inflation for the general population, as well as for the ACA exchanges”
“Premium growth — even when it does reach into the double-digit range that sparks such substantial media attention — is a policy challenge to be examined and addressed and is also part of the general historical pattern that precedes the ACA.” Those who argue “the law as a whole should be scrapped ignore the devastating effect that repeal would have on the estimated 20 million Americans who have thus far gained insurance under the law.”
My take (from commentary): “Regardless of what ends up happening this year, it seems likely that next spring will bring renewed claims that the sky is falling — when experience should make clear that it isn’t.”
Understanding the Risks of Propofol for Colonoscopy
A recent article & editorial (KJ Wernli et al. Gastroenterol 2016; 150: 888-94 & 801-2) shows that the use of propofol, delivered by an anesthetist, is associated with a small increase risk of adverse events. This finding goes against assumptions that there would be reduced complications with an anesthesia expert in the room who could manage resuscitation and airway problems.
The study analyzed claims data from more than 3 million colonoscopies in the U.S between 2008-2011 in 40-64 year-olds.
Key findings:
- Use of anesthesia was associated with a 13% increase in the risk of any complications within 30 days.
- The increased risk included perforation (OR 1.07), hemorrhage (OR 1.28), and abdominal pain (OR 1.07). Interestingly, the perforation risk was increased only in those undergoing polypectomy (OR 1.26) indicating that some confounders may have been difficult to eliminate.
- Complications secondary to anesthesia were present as well (OR 1.15) and stroke (OR 1.04).
This is not the first study to associate anesthesia with increased risk of aspiration and mechanical complications (Cooper G et al. JAMA Intern Med 2013; 173: 551-6). It is certainly possible that the increased risk is due in part to patient selection, despite attempts to control for this.
It is also important to note that better sedation has not resulted in improved colonoscopy outcomes like increased polyp detection.
Will these results change anything? No.
The small increased safety risk (detectable only in studies of millions of patients), if accurate, is not going to stop the use of anesthesia services for two reasons.
- Patient satisfaction
- Financial incentives
Patient satisfaction. Propofol results in excellent sedation, often with complete absence of pain combined with rapid recovery and an antiemetic effect.
Financial incentives. Many endoscopists are able to employ an anesthetist and generate additional revenue by billing for sedation (in addition to the costs of the endoscopist), whereas this is not allowed with the combination of intravenous opioids/benzodiazepines used for ‘deep sedation.’ Even in the many who do not receive revenue for these services, the rapid recovery expedites patient care and room turnover.
My take: While propofol administered by anesthetists is a little less safe and more expensive, it is here to stay, at least until incentives are created to reconsider this approach.
Understanding Single-Payer Health Care: “Medicare for All”
A recent commentary (J Oberlander. NEJM 2016; 374: 1401-3) explains the “virtues and vices of single-payer health care.”
“In a country where nearly 30 million persons remain uninsured, even insured patients face staggering bills, and more money is spent on administration than on heart disease and cancer, it’s no surprise to hear calls for sweeping change.”
Virtues of Single-Payer System:
- Based on Canadian experience, single-payer greatly reduces administrative costs and complexity.
- Concentration of purchasing power
- Guarantee that all residents receive care
- The problems of a single-payer system “pale in comparison” to the current U.S. system
Vices of Single-Payer System:
- Wait lists for some services
- Public dissatisfaction
- Would require increased taxes (though may improve overall finances for most)
It Does Not Matter if Single-Payer is Better:
It would face intense opposition from insurers, medical industry, and would not be adopted by Congress. “In short, single payer has no realistic path to enactment in the foreseeable future.”
My take (in agreement with author): “Preserving and strengthening the ACA [affordable care act] as well as Medicare, and addressing underinsurance and affordability of private coverage is a less utopian cause than single payer. I believe it’s also the best way forward now for U.S. medical care.”
Related blog posts:
- Why Georgia Cannot Provide More Healthcare | gutsandgrowth
- Zip Code or Genetic Code -which is more important for …
- 45,000 Unnecessary Deaths Per Year | gutsandgrowth
- A Leading Cause of Mortality in U.S…. | gutsandgrowth
Looking for Value in Medicine
- Finding Value in Unexpected Places — Fixing the Medicare Physician Fee Schedule. RA Berenson, JD Goodson. NEJM 2016; 374: 1306-10.
- When Is It Ethical to Withhold Prevention? TA Farley. NEJM 2016; 374: 1303-5.
As noted in yesterday’s blog post, after reading these two commentaries I thought a little more about value in pediatric gastroenterology. These articles though focus on other aspects. In the first reference, the authors explain the flaws with moving from volume to value-based care. They note that the medicare physician fee schedule (MPFS) has a powerful influence on physician activities and “their tendency to perform unneeded tests and procedures.” In fact, the fee schedule heavily contributes to growing shortages of primary care physicians. Key points:
- “Two key flaws in the RBVS [resource-based relative value scale] are its substantial misevaluations of physician work and the failure of current service codes to capture the range and intensity of nonprocedural physician activities, known as evaluation and management (E/M) services.”
- “The MPFS still assumes that it takes nearly 30 minutes to interpret a magnetic resonance image of the brain…typically takes about 10.” Echocardiogram per MPFS assumes 31 minutes, but takes 5-10 minutes. For colonoscopy with polyp removal, MPFS assumes 78 minutes, but this is overestimated as well.
- Valuations depend on AMA-sponsored expert panels…not surprisingly, updates that reduce RVUs are rarely proposed.
- While the commentary implies that procedural codes are overvalued, it notes that due to complexity of chronic conditions that E/M codes are undervalued.
- Their conclusion: “implementing new incentives and quality measures in new payment models while maintaining a broken fee schedule is a prescription for failure.”
The second reference bemoans the fact that the medical system will spend enormous amounts of money to prolong the life of an individual with terminal cancer for a few weeks but will not see the imperative of providing adequate prevention measures. Key points:
- “Many people reject any attempt to put a dollar value on human life…but…limits of funding make it impossible to pay for every conceivable intervention.”
- Cost-effectiveness is not considered by Medicare in determining treatment. “For example, treatment of metastatic lung cancer may cost $800,000 per QALY [quality-adjusted life-year], but it is typically provided. In sharp contrast, primary preventative services are often withheld even if they are highly cost-effective.”
- Diabetes prevention program focused on exercise and nutrition has QALY costs of $14,000. Smoking cessation with nicotine-replacement therapy has QALY <$5000.
- Author’s conclusion: “because withholding primary prevention leads to unnecessary suffering and death, we should be just as creative in finding ways to pay for it” as we do with treatment of all illnesses.
My take: At an individual physician level, we need to keep working to utilize our resources more carefully. However, at a policy making level, efforts at improving incentives for primary prevention and primary care are needed.
Related blog posts (see yesterday’s post Why are so many Low Value Endoscopies Performed? for related links as well):

Poster on Front of High Museum is reproduction of Vik Muniz piece created from Jelly and Peanut Butter