This blog entry has abbreviated/summarized these presentations. Though not intentional, some important material is likely to have been omitted; in addition, transcription errors are possible as well.
Here is a link to postgraduate course syllabus: NASPGHAN PG Syllabus – 2017
Biliary Atresia: Update on diagnostic and prognostic biomarkers and therapeutic interventions
Cara Mack Children’s Hospital of Colorado
Key points:
- 84% of biliary atresia is isolated; 16% are syndromic with other defects
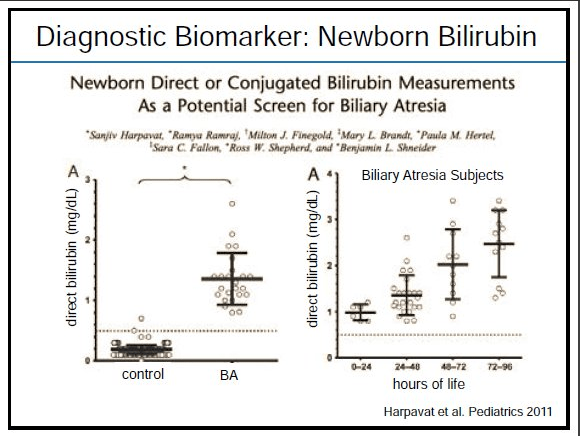
- Direct bilirubin is (mildly) elevated at birth in patients with biliary atresia
- Total bilirubin 3 months after Kasai predicts outcome. If <2 mg/dL, then unlikely to need a transplant in the first 2 years of life.
- Reviewed biomarkers including Th1, Autotaxin, IL-8
Therapeutic interventions:
- Nutritional support. Better nutrition improves outcomes after liver transplantation.
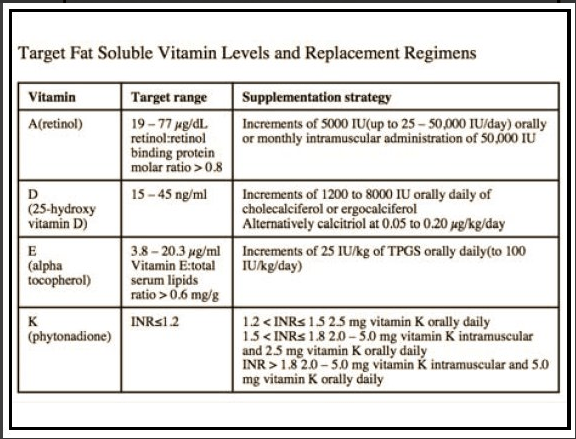
- Fat soluble vitamin supplementation
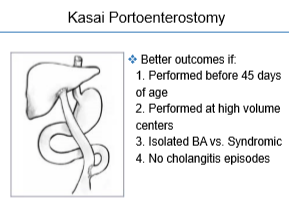
- Cholangitis prevention. Some studies have shown that prophylactic antibiotics may reduce incidence of cholangitis.
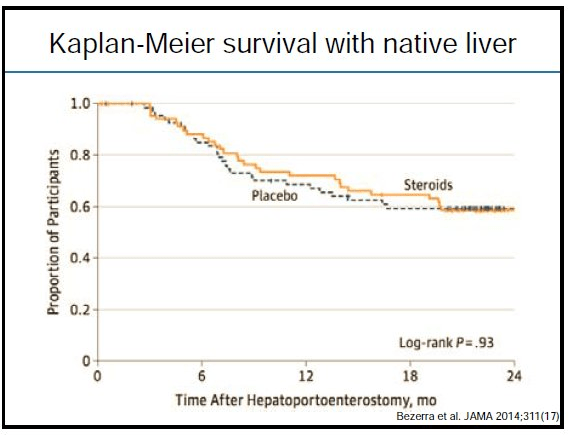
- No therapeutic interventions that delay progression of this disease
Diagnosis and Management of Pediatric NAFLD 2017
Stavra Xanthokos Cincinnati Children’s Hospital Medical Center
Key points:
- NAFLD is #2 cause of liver transplantation in adults and on its way to becoming #1
- ALT is still the best screening tool; NASPGHAN guidelines recommends screening overweight/obese children 9-11 years of age
- Ultrasound has poor sensitivity and specificity for NAFLD; it is helpful for detecting gallbladder disease
- Bariatric surgery has been effective for NAFLD
SMOFlipid and the Pediatric Patient
Peter Wales Hospital for Sick Children (Toronto)
Slides are not available in syllabus
Key points:
- Improving outcomes noted in the intestinal failure population
- Dr. Wales reviewed proposed improvements with Omega-3 lipids -less cholestasis, less hepatitis, and less fibrosis
- Compared improvements with lipid minimization (1 g/kg/day) compared to newer agents: omegaven and SMOFlipid. Additional studies are needed due to limitations of previous studies
- Discussed SMOFlipid vs. Intralipid trial at 5 centers in Canada. N=24.
- At SickKids: SMOFlipid for all preterms at admission & for term infants after 2 weeks of PN. Dosing 2-2.5 g/kg & now accounts for 85% of lipid usage at institution
- None of the lipid products were designed for preterm infants. Intralipid has a pediatric indication and other products are used off label
- Lipid restriction probably affects brain size/development; thus, a lipid agent that allows for higher doses likely will be beneficial for developmental outcomes. The retina can be used as a biomarker of the brain affects of lipids.
Painful Chronic Pancreatitis: Management/therapeutic interventions
Vikesh Singh Johns Hopkins University School of Medicine
Slides are not available in syllabus