8/2/23 NPR Lisa Doggett: Doctors have their own diagnosis: ‘Moral distress’ from an inhumane health system
This article describes the terms “moral injury” and “moral distress” which contribute to job dissatisfaction for physicians.
Here are excerpts:
The terms “moral distress” and “moral injury” were first used in a military context to characterize the torment felt by soldiers as they tried to process and justify their actions amid the cruelty of war. In more recent years, these terms have been used to describe the feelings of guilt, sadness and defeat felt by health care professionals when we know what our patients need but can’t provide it...
At Austin’s CD Doyle clinic for people who are homeless, where I volunteer, nearly every patient has unmet needs impacting their health…Even in well-resourced private clinics, doctors often feel frustrated that they can’t spend time with patients who need it and have little control over their schedules…
Doctors struggle to meet productivity demands, rushing in and out of exam rooms, working late into the evening to finish documenting in cumbersome electronic medical record systems. Despite some efforts to move away from a “fee-for-service” payment model, in most cases, our system still rewards volume of patients seen over value of care provided…
In Texas and other states, recent legislation, such as abortion bans and prohibitions against gender-affirming care for trans-youth, have introduced new moral dilemmas for doctors. We want to do right by our patients but face added barriers – even the potential for jail time – if we overreach or misinterpret the laws…
A commitment from health care leaders, health insurance plans, and all levels of government to address the nonmedical conditions in which we live, work, learn and play — the social determinants of health that drive 80% to 90% of health outcomes on a population level – would improve the health of individuals and communities. It would also decrease the pressure on doctors to treat medical conditions stemming from unhealthy environments that we can’t change.
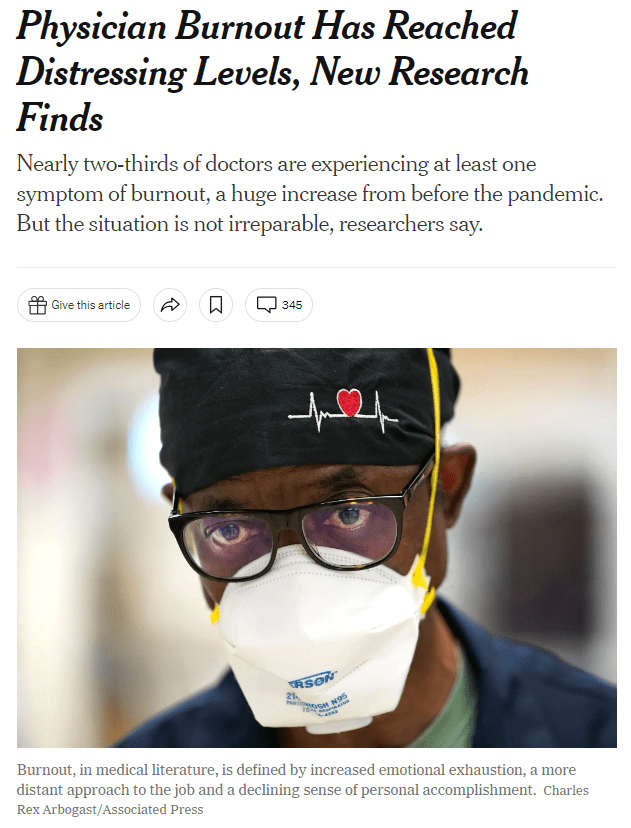
A survey published last fall in Mayo Clinic Proceedings showed an alarming increase in physician burnout, with 62.8% of respondents reporting at least one symptom in 2021 compared to just 38.2% in 2020.
Physicians, too, face rates of depression and suicide that are higher than the among the general population. While moral distress doesn’t fully account for the difference, it is a contributing factor for some.
My take: My role as a physician is often constrained by troubling factors out of my control including lack of resources and poor social situations.
Related blog posts:
- What is the Difference Between Burnout and Depression?
- Primary Care Physician Looming Shortage
- Why Physician Burnout Is Happening & How to Fix It
- Briefly Noted: Avoid Food Sensitivity Testing, Physician Burnout Worsening and Apple Medication Tracker