A Bautista-Casasnovas et al. JPGN Reports 4(4):p e353, November 2023. Open access! Multicentre Study Into the Use of Polyethylene Glycol With Electrolytes Over at Least 6 Months to Treat Constipation in Paediatric Populations
Background: PEG 3350 with electrolytes (PEG+E) is the most widely used osmotic laxative in Europe, and it is normally prescribed for short or limited periods in children, such that there is little information regarding its long-term use (≥6 months).
Methods: This was a retrospective, observational, descriptive, longitudinal, and multicentre study was carried out on 74 children diagnosed with functional constipation.
Patient characteristics: The mean (±SD) duration of the symptoms of constipation before starting PEG+E treatment was >1 year (15.6 ± 8.4 months). Fecal disimpaction was necessary in 49 children (66.2%) .
Key findings:
- The mean PEG+E dose used was 1.0 (±0.8) g/kg.
- The mean duration of PEG+E use was 18.6 (±13.4) months (range 8–73 months), and 59.45% (n = 44) of the patients took the treatment for more than 1 year.
- 81% (n = 60) of the patients achieved 4 or more weekly bowel movements after having taken PEG+E for at least 3 weeks.
- All clinical symptoms (abdominal pain, gassiness/bloating) were reduced considerably, with the resolution of the anal fissures, bleeding, and soiling in all patients.

Polyethylene glycol (the active ingredient in Miralax) is considered a first-line treatment for pediatric constipation and for fecal impaction. “However, caregivers may be hesitant to administer medication over long periods due to a fear of a rebound effect or addiction (23). Indeed, early withdrawal of laxatives is the commonest cause of recurrence (4,5), highlighting the need for longer follow-up studies (8).”
My take: It is helpful to have long term studies of PEG 3350 showing its effectiveness and safety, especially as the medication labels state to not use these medications for more than 7 days.
Related blog posts:
- Expert 2017 Opinion: Miralax is (Still) First Choice Laxative for Children
- Updated Pediatric Expert Constipation Guidelines
- Here we go again …Miralax Safety Questioned
- Which is Safer and More Effective –Miralax (PEG 3350) or Lactulose?
- Miralax Safety
- Safety of Senna-Based Laxatives
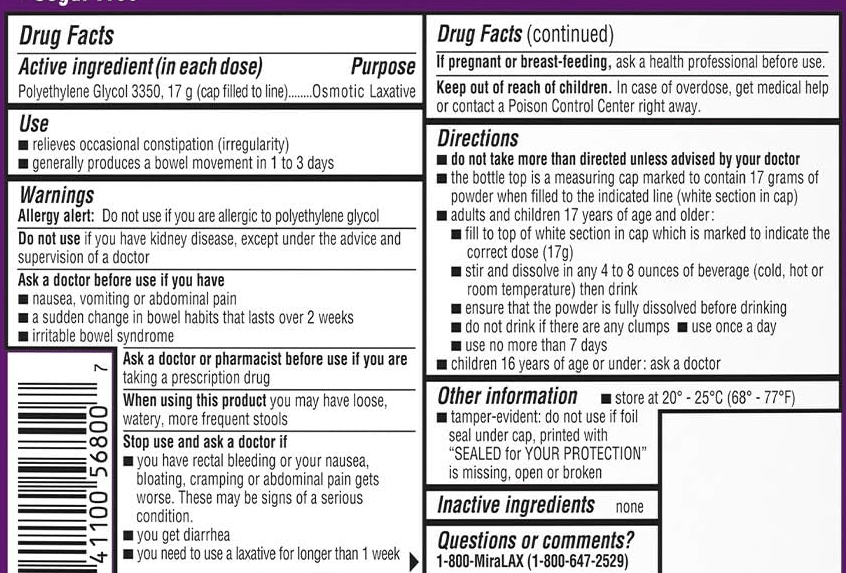
Clarification: However, Ben Enav pointed out that the label also states the following in bold: “do not take more than directed unless advised by your doctor.” The actual label is shown below.