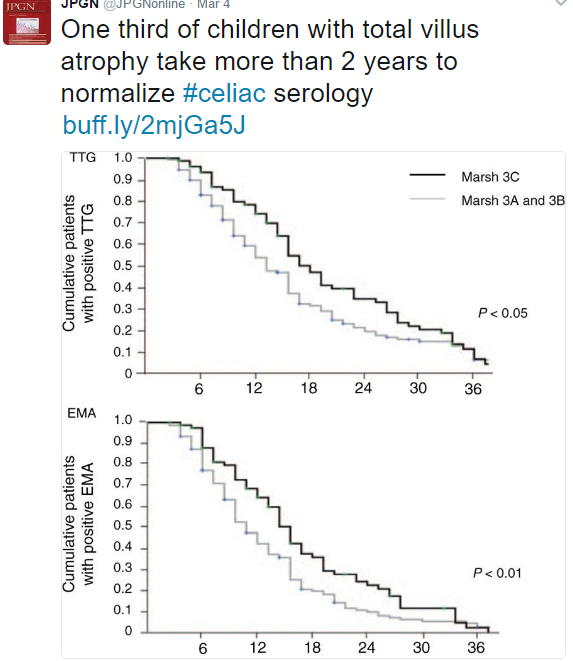
A retrospective study from Boston has gained attention for suggesting that repeat biopsies may be needed for celiac disease (published online, MM Leonard et al JPGN, doi: 10.1097/MPG.0000000000001460). In my view, this may be a little early for that recommendation for asymptomatic patients with normal serology.
Full Abstract:
Value of IgA tTG in Predicting Mucosal Recovery in Children with Celiac Disease on a Gluten Free Diet.
Objective: Our objective was to determine the rate of mucosal recovery in pediatric patients with celiac disease on a gluten free diet. We also sought to determine whether IgA tissue transglutaminase (tTG) correlates with mucosal damage at the time of a repeat endoscopy with duodenal biopsy in these patients.
Methods: We performed a retrospective chart review of one-hundred and three pediatric patients, under 21 years of age, with a diagnosis of celiac disease defined as Marsh 3 histology, and who underwent a repeat endoscopy with duodenal biopsy at least twelve months after initiating a gluten free diet.
Results: We found that 19% of pediatric patients treated with a gluten free diet had persistent enteropathy. At the time of the repeat biopsy, tTG was elevated in 43% of cases with persistent enteropathy and 32% of cases in which there was mucosal recovery. Overall the positive predictive value of the autoantibody tissue transglutaminase was 25% and the negative predictive value was 83% in patients on a gluten free diet for a median of 2.4 years.
Conclusions: Nearly one in five children with celiac disease in our population had persistent enteropathy despite maintaining a gluten free diet and IgA tTG was not an accurate marker of mucosal recovery. Neither the presence of symptoms nor positive serology were predictive of a patient’s histology at the time of repeat biopsy. These findings suggest a revisitation of monitoring and management criteria of celiac disease in childhood.
Link to full text: A few other key points:
- The most common indications for repeat endoscopy were due to persistent symptoms (43%) and new gastrointestinal symptoms (27%). Twenty-four subjects (34%) had persistently elevated serology at the time of the repeat biopsy.
- 19% exhibited persistent enteropathy consistent with a Marsh 3 lesion at the time of the repeat endoscopy.
- Only 71 patients had serology within 4 months of repeat endoscopy, limiting the interpretation of the concordance of tTG value to histology
My take: I think it is premature to recommend routine followup biopsies in asymptomatic patients with normal serology. I think a prospective study will be helpful; the majority of patients in this study who underwent repeat biopsy were symptomatic and 9% were not adherent to their diet. Thus, this may not reflect a typical patient with celiac disease at followup. In addition, it would be helpful with regard to whether persistent histological findings have clinical significance.
Despite these limitations –this is how this article is being reported (from news-medical.net), here’s an excerpt from a recent summary:
Alessio Fasano, MD, director of the MGHfC center and co-senior author of the study, was also surprised by the results, which were based on a retrospective examination of the biopsy and medical records of 103 children with celiac disease treated at MGHfC or BCH. The children had been on the gluten-free diet for at least one year and were determined by dietitians and other hospital health care practitioners to have complied well with the diet. But repeat biopsies found persistent intestinal damage in 19 percent of them. “The number of children who don’t heal on the gluten-free diet was much higher than what I expected,” Fasano says.
Another finding that surprised Fasano was that blood levels of the autoantibody IgA tTG – the primary lab test used to monitor celiac disease – did not accurately measure mucosal recovery.
Related blog posts:
Disclaimer: These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition.