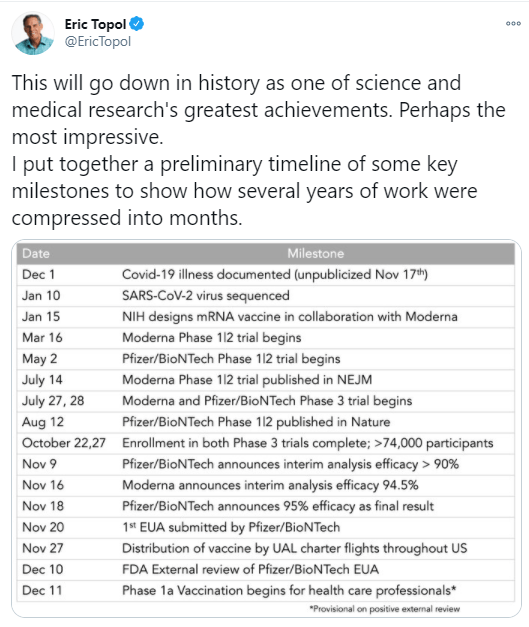
NE Ebel et al. J Pediatr 2020; 226: 195-201. Decreased Incidence of Hepatic Artery Thrombosis in Pediatric Liver Transplantation Using Technical Variant Grafts: Report of the Society of Pediatric Liver Transplantation Experience
This study used multicenter data from the Society of Pediatric Liver Transplantation on first-time pediatric (aged <18 years) liver transplant recipients (n = 3801) in the US and Canada (1995-2016).
Key findings:
- 7.4% developed HAT within the first 90 days of transplantation.
- Of those who were retransplanted, 20.7% developed recurrent HAT.
- Those less than 1 year had the highest risk OR 1.20).
- Lower Risk for HAT:
- Recipients with split, reduced, or living donor grafts had decreased odds of HAT (OR, 0.59; P < .001 compared with whole grafts)
- Adolescents aged 11-17 years (OR, 0.53; P = .03).
- HAT increased risk of graft failure and mortality:
- Fifty percent of children who developed HAT developed graft failure within the first 90 days of transplantation (adjusted hazard ratio, 11.87; 95% CI, 9.02-15.62)
- Mortality risk (w/in 90 days after transplantation): adjusted hazard ratio, 6.18 (95% CI, 4.01-9.53).
The finding that split grafts had lower rates of HAT may be related to the fact that these grafts more typically come from larger donors with larger vessels. Historically, split grafts had been described as a risk factor for HAT. The authors note that high-performing centers with the lowest incidence of HAT “also tend to have high rates of living and split transplants, suggesting that surgical expertise may play a role in the decreased risk of HAT in select recipients with technical variant grafts.”
Increased rates of HAT among those who were retransplanted, in some, could be related to thrombophilic conditions; thus, consideration of anticoagulation protocol could be needed
My take: Continued efforts are needed to reduce HAT due to its impact on liver transplantation outcomes. One of the biggest risk factors is age. While this would seem to be a nonmodifiable factor, improving recognition and treatment of biliary atresia could help.
Related blog posts:
- Outcomes of Liver Transplantation in Small Infants
- “Big Improvements for Smallest Recipients” with Bad Liver Disease
- Pediatric Liver Transplantation: Past Time to Split
- Picking winners and losers with liver transplantation allocation
- Landmark Study on Universal Screening for Biliary Atresia –It Works!
- High Survival Rates for Biliary Atresia Patients Undergoing Liver Transplantation