C Crist. GI & Hepatology News; 11/20/24: In IBD Patients, No Increased Risk for MACE Seen for JAK Inhibitors vs Anti-TNF
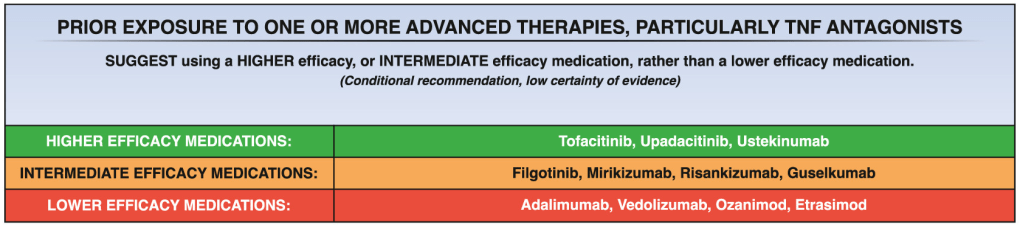
Background: There have been concerns that JAK inhibitors (JAKi), like tofacitinib (Xeljanz) and upadacitinib (Rinvoq) could increase the risk of major adverse cardiovascular events (MACE); as such, the FDA has placed warnings on these medications (see blog post: FDA Slaps Restrictions on JAK Inhibitors Over Serious Safety Risks).
An excerpt:
According to a study presented at the American College of Gastroenterology (ACG) 2024 Annual Scientific Meeting, .
Alsakarneh and colleagues conducted a retrospective cohort study using the TriNetX database to identify adult patients with IBD who were treated with JAKi or anti-TNF therapy after diagnosis. After matching patients in the JAKi cohort [n=3740] with patients in the anti-TNF cohort [n=3740], the research team looked for MACE and VTE within a year of medication initiation…
After excluding those with a history of a prior cardiovascular event, 57 patients (1.76%) in the JAKi cohort developed MACE, compared with 63 patients (1.94%) in the anti-TNF cohort. There weren’t significant differences between the groups in MACE (adjusted hazard ratio [aHR], 0.99) or VTE (aHR, 0.9).
Among patients aged ≥ 65, 25 patients (5.3%) in the JAKi cohort developed MACE, as compared with 30 patients (6.4%) in the anti-TNF cohort.
My take: Several studies now have not identified an increased risk of JAKi compared to other therapies for IBD. Perhaps, this will lead to a change in labeling by the FDA which has stated that JAKi should be used only in those with prior anti-TNF failure.
Related blog posts:
- Treatments for “Bad” Inflammatory Bowel Disease (Part 2) & Reassuring Data on Tofacitinib
- FDA Slaps Restrictions on JAK Inhibitors Over Serious Safety Risks
- Dr. Joel Rosh: Positioning Therapies for Pediatric Ulcerative Colitis
- Lipid Changes with IBD Medications
- Practice Tips for New IBD Therapies