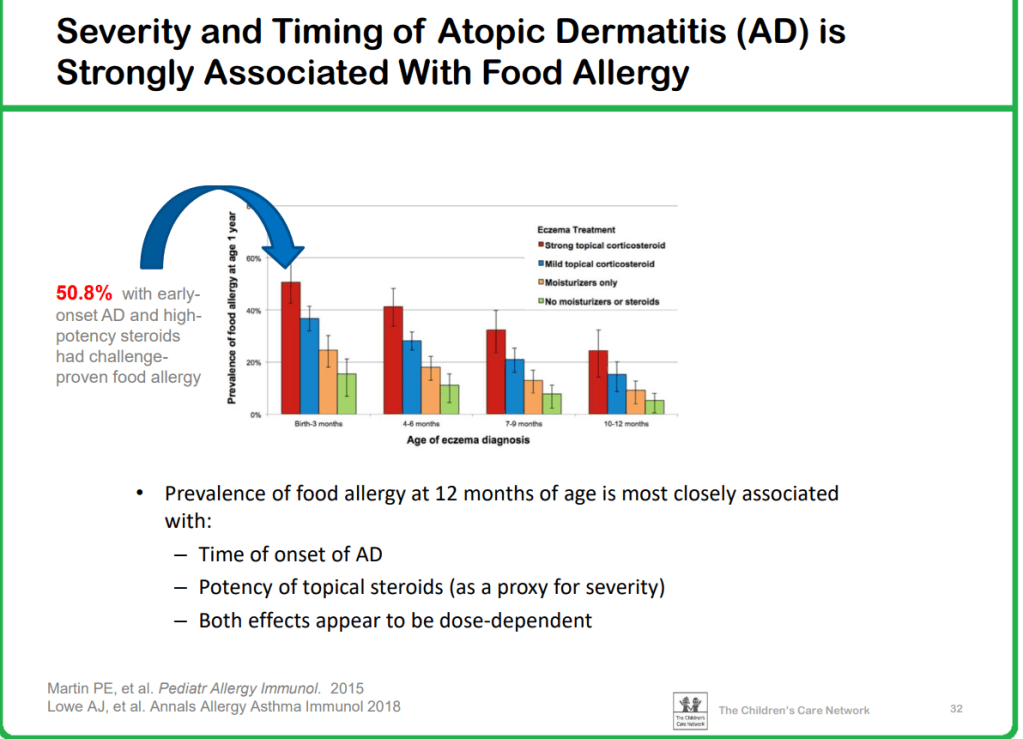
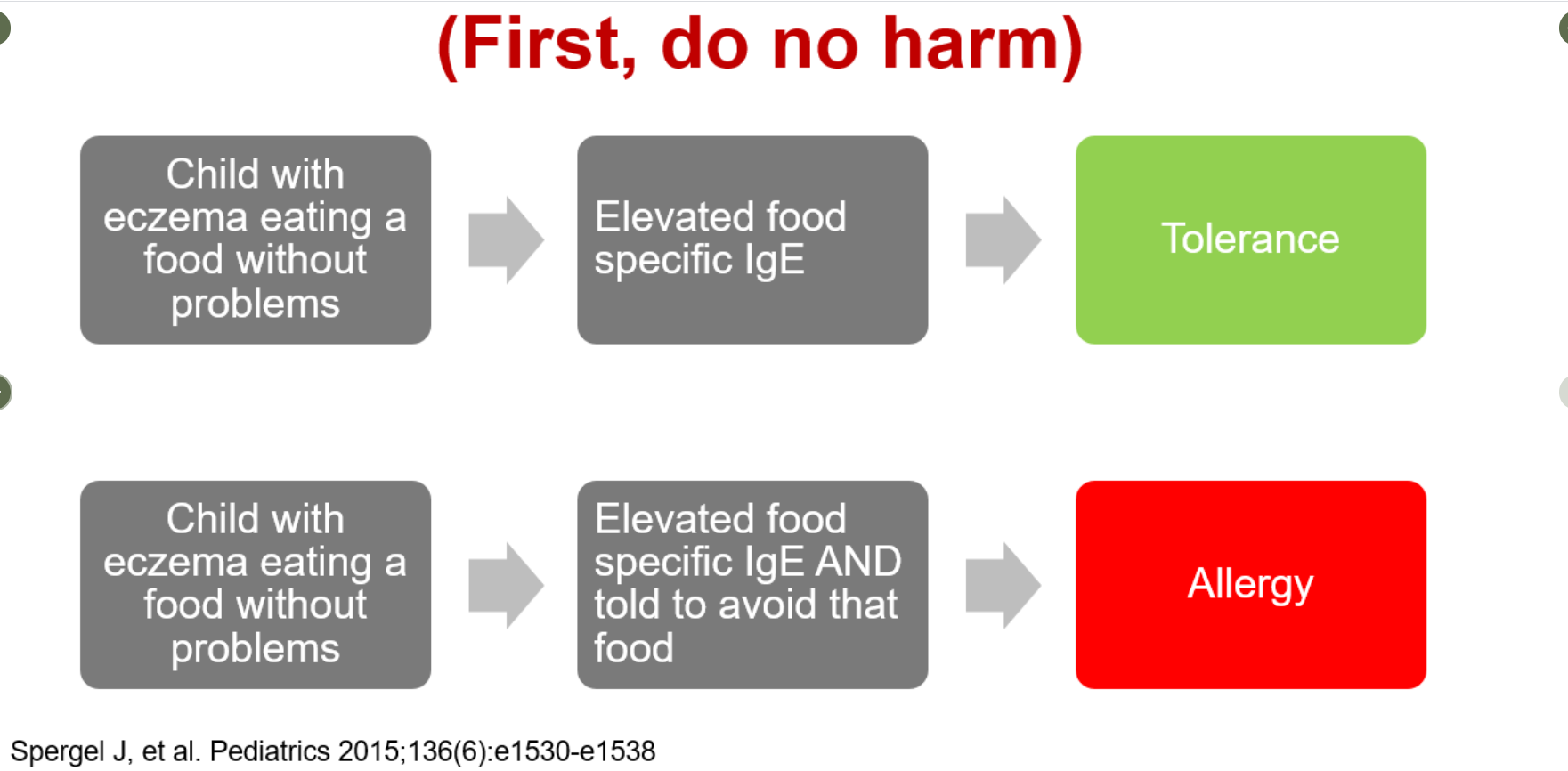
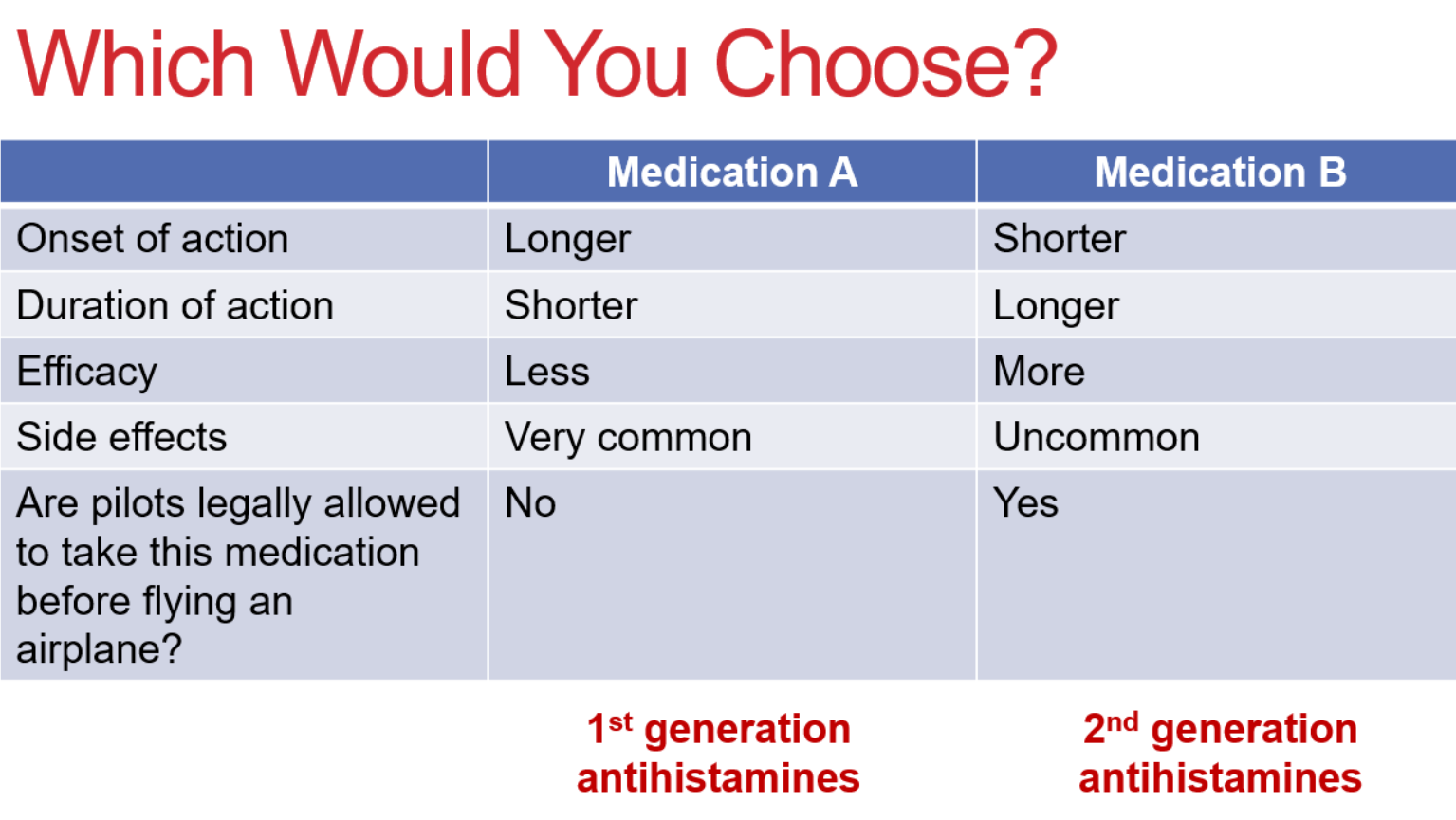
E Fradkov et al. Inflamm Bowel Dis 2022; 28: 895-904. Efficacy of Ustekinumab in Crohn’s Disease With and Without Concurrent Autoimmune Skin Disease
This retrospective study reviewed 395 CD patients received ustekinumab therapy (79 CD-ASD (autoimmune skin disease), 316 CD-none). ASD included atopic dermatitis, eczema, psoriasis/psoriaform dermatitis and alopecia. The skin disease group also included those with cutaneous manifestations of Crohn’s disease: erythema nodosum, pyoderma gangrenosum, pyostomatitis vegetans, Sweet’s syndrome, granulomatous vasculitis, and leukocytoclastic vasculitis. 55 of the 79 with CD-ASD had psoriatic disease, 20 had eczema, 11 had erythema nodosum, 8 had pyoderma gangrenosum.
Key findings:
- Ustekinumab had greater efficacy in CD-ASD when evaluated by fecal calprotectin (P = .0337) and CRP (P = .078). For calprotectin, the values decreased by 61% after at least 5 months of therapy (394 to 164) in the CD-ASD group compared to 11% in the group without skin disease (365 to 265)
- The CD-ASD group also showed better outcomes in Likert scores of endoscopy (P = .016), histopathology (P = .074), and imaging (P = .094).
My take: Ustekinumab appears to be particularly effective in patients with concurrent skin disease.
Related posts:
- Characteristics of Skin Lesions Associated with Anti-Tumor Necrosis Factor Therapy | gutsandgrowth
- IBD Updates: Fatigue Trajectory, Risk of IBD with Derm Findings
- Pattern of Skin Reactions to Anti-TNF Agents | gutsandgrowth
- TNF Antagonists and Psoriasis | gutsandgrowth
- IBD Shorts -Skin, Adalimumab Kinetics
- IBD and Chronic Recurrent Multifocal Osteomyelitis: Paradoxical Association with anti-TNF Therapy in Some Cases