Earlier this week, I was tasked with helping a teenager with an upper GI bleed. I was surprised to learn that our hospital did not have IV erythromycin available due to a shortage. A potential alternative is azithromycin.
The following is a 2017 ACG abstract (D Issa et al): A Comparison of Azithromycin to Erythromycin Infusions in Improving Visualization of Endoscopy for Upper Gastrointestinal Bleeding
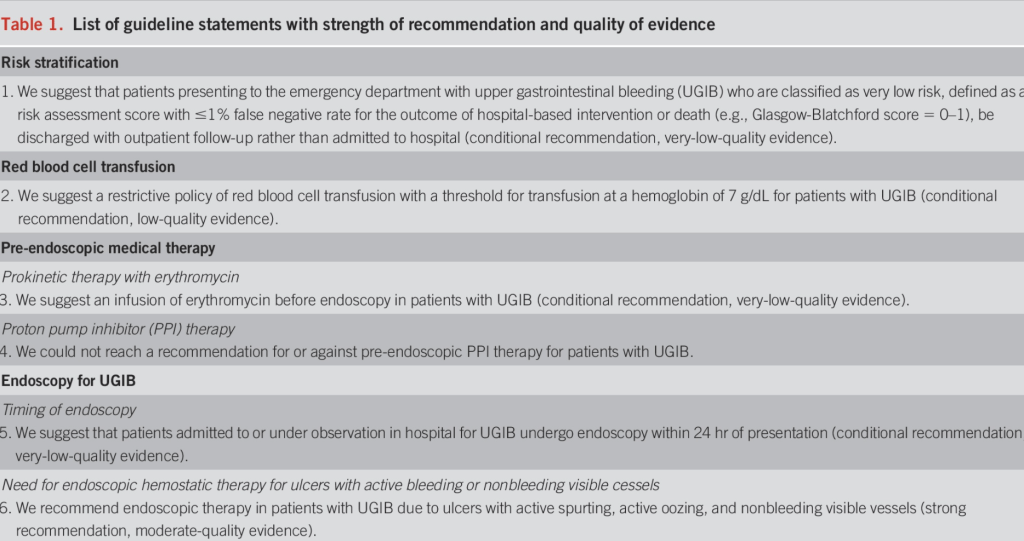
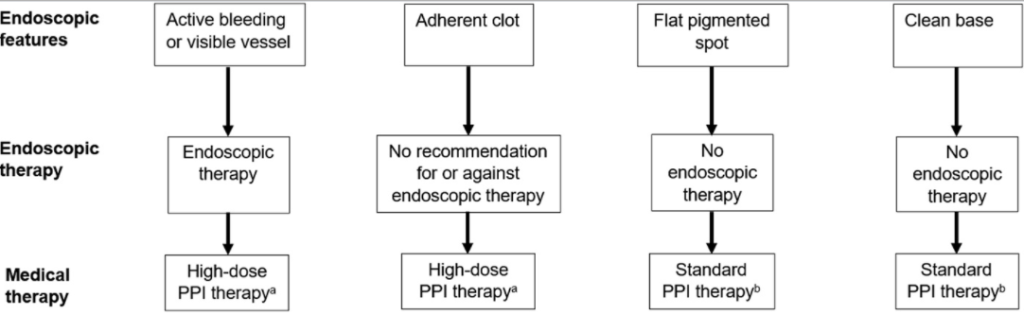
Introduction: Several studies show the use of intravenous erythromycin prior to upper endoscopy for upper gastrointestinal bleeding (GIB) improves visualization and decreases the need for second look endoscopy. Erythromycin requires reconstitution delaying administration in emergency procedures. Azithromycin is more readily available as it is part of pneumonia treatment protocols and does not require reconstitution. Physiologic studies show azithromycin produces motility effects similar to that of erythromycin.
Aim: To assess the effect of azithromycin in improving the quality of endoscopic visualization in upper GIB compared to erythromycin.
Methods: We performed a retrospective analysis of patients admitted with acute upper GIB who underwent emergent endoscopy and were ordered either erythromycin or azithromycin before procedure. Primary outcome of the quality of visualization was assessed by two gastroenterologists, blinded to the choice of infusion, using a scoring system ranging from 0 to 8 with a maximum of 2 points assigned to each of the fundus, body, antrum and bulb. Secondary outcomes included time elapsed between administering the infusion and starting the procedure, length of hospital stay, blood transfusions, and procedure-related complications.
Results: The study included 31 patients in the erythromycin group and 18 patients in the azithromycin group. Mean age was 57 years and 68% were male. The overall median visualization score was significantly higher in the azithromycin group compared to that of the erythromycin group {7.0 (1.5) vs. 6.0 (3.0), respectively; P=0.02}. Time between administration of azithromycin and starting the procedure was longer than that of erythromycin but did not meet statistical significance (67 vs 48.5 minutes, respectively; P = 0.92). Length of hospital stay was comparable between the two groups after adjusting for the admission primary diagnosis (6.0 days for azithromycin vs. 7.0 days for erythromycin; P=0.48). Four patients were ordered erythromycin but this was not administered on time whereas all patient who were ordered azithromycin started the infusion prior to the procedure. Procedure immediate complications, need for second look endoscopy and number of transfused blood units did not differ between the groups.
Discussion: Azithromycin infusion before endoscopy for upper GIB was associated with better visualization than that of erythromycin, the current standard of care. Randomized trials are needed to validate these findings.
Here is a link to a summary from Gastro and Endoscopy News: Azithromycin Appears Worthy Stand-In For Erythromycin in Upper GI Bleeding
There have been prior publications showing that azithromycin, like erythromycin, has prokinetic properties: Broad J, Sanger GJ. The antibiotic azithromycin is a motilin receptor agonist in human stomach: comparison with erythromycin. Br J Pharmacol. 2013 Apr;168(8):1859-67.
Related blog posts:

Disclaimer: These blog posts are for educational purposes only. Specific dosing of medications/diets (along with potential adverse effects) should be confirmed by prescribing physician/nutritionist. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition.