In the movie There’s Something About Mary, there is a scene (YouTube: 7-minute abs) where the main character picks up a hitchhiker. The hitchhiker reveals his brilliant idea for the 7-minute ab workout to replace the 8-minute ab workout. Of course, he becomes upset when the lead character suggests that someone else could invent the 6-minute ab workout.
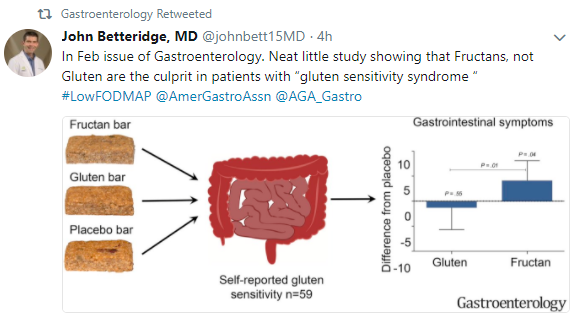
This is what I was thinking of when I read a recent article describing a simplified, less restrictive low FODMAP diet.
P Singh et al. Clin Gastroenterol Hepatol 2025; 23: 362-364. Is a Simplified, Less Restrictive Low FODMAP Diet Possible? Results From a Double-Blind, Pilot Randomized Controlled Trial
This pilot study with 35 subjects with IBS-D were randomized to a standard low FODMAP diet (LFD) or to a simplified FODMAP diet which eliminated solely fructans and galactooligosaccharides. The primary endpoint was the proportion of subjects meeting the FDA responder definition for abdominal pain intensity (ie. a >/= 30% reduction in weekly average of daily abdominal pain scores for 2 of the 4-week treatment period).
Key findings:
- There was a similar reduction in key symptoms (see below)
- Fewer individuals in the simplified diet dropped out due to side effects or difficulty with adherence (12.5% vs 26.3%)
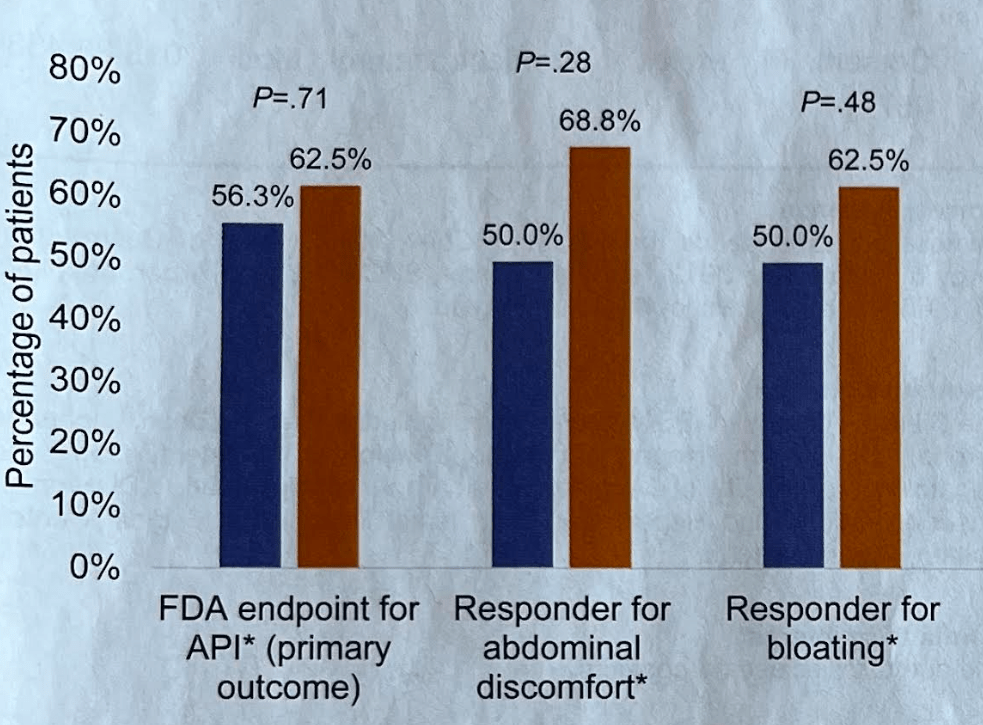
and orange represents response to simplified low FODMAP diet (n=16)
My take: Larger trials are needed. This study suggests that a simplified version of a low FODMAP diet would improve symptoms in most patients with IBS-D.
Related blog posts:
- Low-FODMAPs with or without Gluten-Free Diet in IBS
- Which FODMAPs are Most Difficult to Reintroduce in Patients with Irritable Bowel Syndrome
- “How to Approach a Patient with Difficult-to-Treat IBS”
- Differential Microbiome Effects of Prebiotics and low FODMAPs
- Fructans and FODMAPs in Children with Irritable Bowel Syndrome