A Khan et al. Clin Gastroenterol Hepatol 2020; 18: 1913-1922. Nonceliac Gluten and Wheat Sensitivity
This useful review notes that ” there is a great deal of skepticism within the scientific community questioning the existence of NCGS as a distinct clinical disorder.”
Key points:
- The pathogenesis of NCGS is unclear and there is no known biomarker or diagnostic histologic lesion for this condition.
- In these suspected patients, it is important to first exclude celiac disease and wheat allergy (especially if a rash with eating). If celiac disease is identified, this allows for appropriate longitudinal followup, strict dietary instructions, and potential screening of at-risk family members.
- Recent studies have shown that GI symptoms in those labelled with NCGS are frequently due to dietary FODMAPs.
- In a large meta-analysis study with 1312 adults, only 16% of participants experience gluten-specific symptoms using a double-blind placebo-controlled rechallenge. In addition, 40% of participants experienced a nocebo response (ie. a greater negative effect than usual due to negative expectation from a dietary treatment)
- In clinical practice, a single blind placebo-controlled rechallenge trial has been recommended for diagnosis
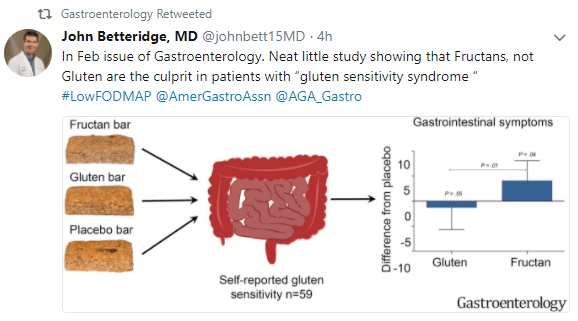
My take: GFD is often unnecessary and ineffective, even in those who have previously identified gluten as a potential food trigger. Fructans are more likely to induce gastrointestinal symptoms.
Related blog posts:
- Fructans, not Gluten, Induces GI Symptoms in Patients with NCGS
- FODMAP diet -Real World Experience
- FODMAPs Advice From Harvard
- An Unexpected Twist for “Gluten Sensitivity” | gutsandgrowth
- Low-FODMAPs with or without Gluten-Free Diet in IBS …
- Mechanism for FODMAPs diet | gutsandgrowth
- Another Study: Low FODMAPs for IBS