A recent study (MDE Potter et al. Am J Gastroenterol 2018; 113: 1036-44 -thanks to Ben Gold for this reference) examined the frequency of wheat intolerance and chronic gastrointestinal symptoms in a randomly selected population of 3542 in Autstralia via a mail survey.
Key findings:
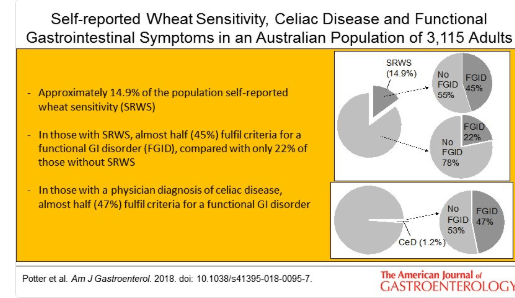
- Self-reported wheat sensitivity was 14.9%
- Prevalence of celiac disease (CD) was 1.2%
- A doctor-diagnosis of CD was associated with functional dyspepsia with an odds ratio (OR) of 3.35.
- Self-reported wheat sensitivity was independently associated with irritable bowel syndrome with an OR of 3.55 and almost half (45%) have an underlying functional GI disorder.
In a related editorial (pgs 945-8), Imran Aziz makes several useful points:
- Gluten-free industry has boomed in U.S. with retail sales going from $0.9 billion in 2006 to ~S24 billion in 2020.
- While previous studies have shown that gluten can induce symptoms in the absence of CD (Biesiekierski JR et al. Am J Gastroenterol 2011; 106: 508-14), more recent rigorous studies have indicated that “gluten-per-se accounts for 1-in-6 cases with the remaining majority either due to fructans (a type of FODMAP or a nocebo effect.”
- There are no accurate biomarkers of wheat intolerance
- Dr. Aziz also cautions against adopting a gluten-free diet without proper counseling. “The greatest concern is whether these diets are safe in the long-run, given the emerging data suggesting cardiovascular, nutritional, metabolic, and microbial changes.”
My take: This study shows that about 1 in 10 individuals have self-reported wheat intolerance; gluten, though, is the actual culprit in less than 20%.
Related Blog Posts:
- Wheat Intolerance Syndrome?
- What to make of FODMAPs | gutsandgrowth
- An Unexpected Twist for “Gluten Sensitivity” | gutsandgrowth
- Food choices, FODMAPs, and gluten haters | gutsandgrowth
- UVA Links | gutsandgrowth
- Mechanism for FODMAPs diet
- Low FODMAPs Diet in Pediatric Irritable Bowel | gutsandgrowth