The advent of highly-effective therapy for hepatitis C has led to the use of hepatitis C-infected livers for organ transplantation.
H Bohorquez et al. Liver Transplantation 2021; 27: 548-557. Liver Transplantation Using Hepatitis C Virus–Viremic Donors Into Hepatitis C Virus–Aviremic Recipients as Standard of Care
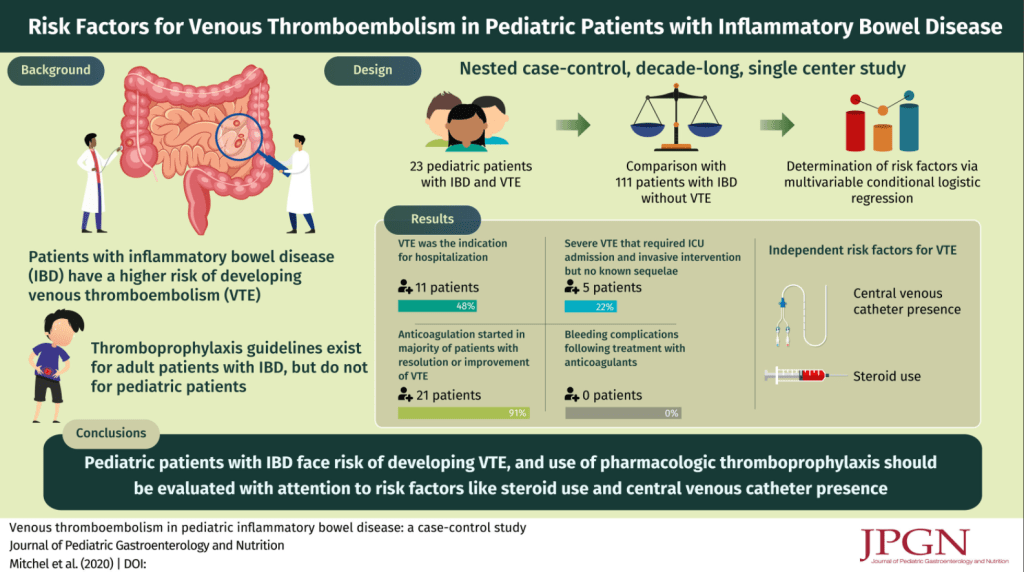
Methods: The authors would utilize livers from donors with hepatitis C if they had a “normal gross appearance or, in cases in which a liver biopsy was indicated, acceptable histology less than grade 2 inflammation and less than stage 2 fibrosis (Batts-Ludwig classification)”
Key findings:
- 292 patients, 61 rHCV− received DNAT+ livers (study group), and 231 rHCV− received DNAT− (aviremic donors [nuclear acid test‐negative donors]) (2018-2019)
- 1‐year post‐LT patient and graft survival were similar between groups
- In the study group, 4 patients died, and 1 patient required retransplantation within the first year post‐LT (all unrelated to HCV)
- 51 patients completed DAA treatment, all achieving sustained virologic response for 12 or more weeks (SVR‐12) (one required re-treatment)
Given the limited organ availability, using livers from donors with hepatitis C has the potential to reduce waitlist times and waitlist mortality.
My take: Liver transplantation with hepatitis C has become bidirectional; livers are being received by those with liver failure due to hepatitis C and failed livers are being replaced by donors infected with hepatitis C.
Related blog posts:
- Liver Shorts August 2020 -large study of HCV+ organ donation (kidney, liver, heart)
- Expanding Organ Transplantation with Hepatitis C-Positive Donors
- Increased Organ Availability Related to Opioid Epidemic
- Opioid Epidemic –Devastating Impact on Children
- Hepatitis C Infections Increasing -Tied to Opioid Crisis