FH Bloomfield et al. NEJM 2022; 387: 1661-1672. Early Amino Acids in Extremely Preterm Babies
My take: For preterm infants <1000 gram, this study showed that the usual dosing of amino acids 2.5 gram to 3.5 gram per day (the placebo group) appeared to have better secondary outcomes (though within confidence intervals) than those who received an additional 1 gram per day.
Slides from video summary:
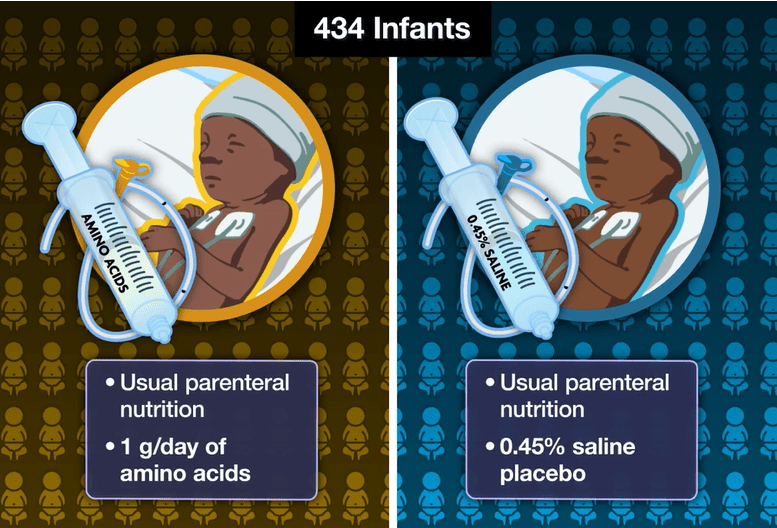
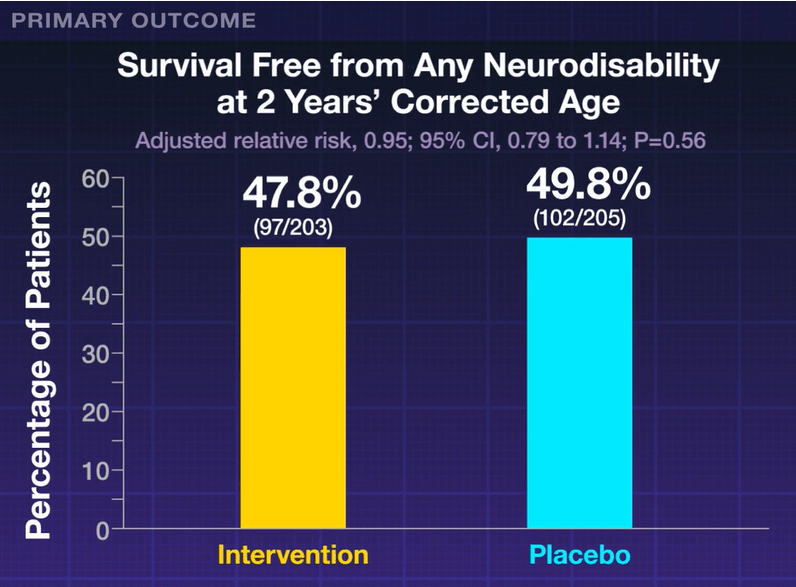
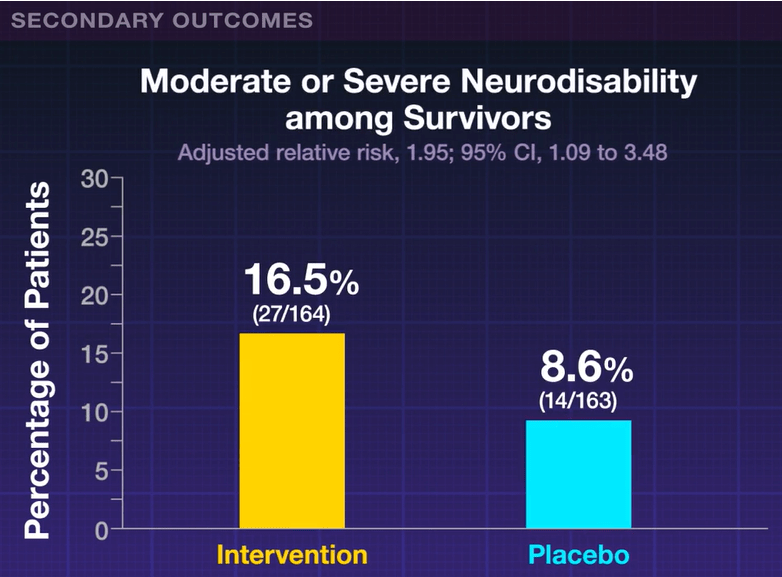
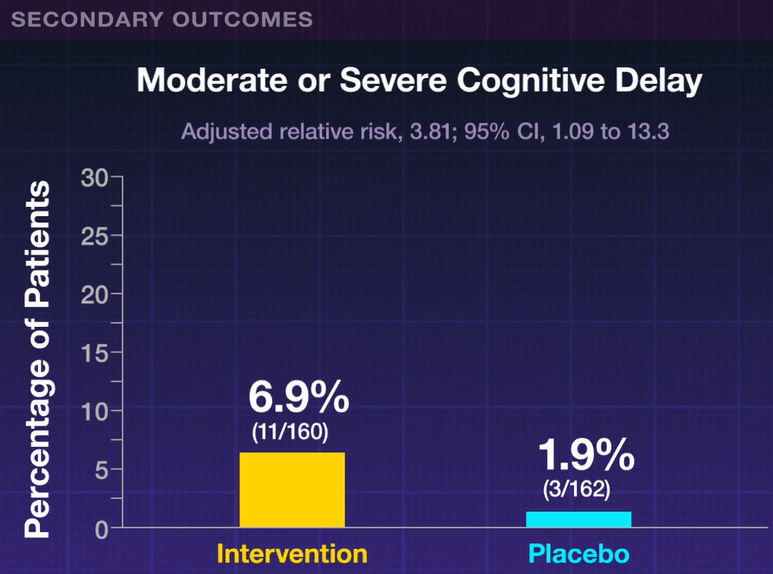


Related blog posts:
- Georgia AAP Nutrition Symposium 2019: Care of the NICU (Premature Infant) Graduate | gutsandgrowth
- Neonatal Nutrition Lecture -What We Know Right Now
- Improving Outlook in Neonatal Nutrition (Part 1) | gutsandgrowth
- Improving Outlook in Neonatal Nutrition (Part 2) | gutsandgrowth
- What’s Happening on the Edge of Viability | gutsandgrowth
- ESPGHAN Position Paper: Nutrition for Critically Ill Neonates | gutsandgrowth



