J McCreary. MedPage Today; 2/26/26. Open Access! Same Stool Sample, Different Results in Gut Microbiome Tests
An excerpt:
“Direct-to-consumer gut microbiome tests produced markedly different results — even when analyzing the same stool sample, researchers found.
Identical fecal samples sent via 21 home-testing kits to seven anonymized direct-to-consumer testing companies yielded a wide variation in reported bacterial abundance and in the health assessments generated from those data, reported Stephanie L. Servetas, PhD, of the National Institute of Standards and Technology (NIST) in Gaithersburg, Maryland, and colleagues in Communications Biology.
In some cases, there was not even agreement among kits produced by the same company…
When researchers compared 18 commonly reported microbial genera across companies, no single provider aligned with the consensus profile for all 18. Across the full dataset, 1,208 unique taxa were reported, but only three genera appeared in every company’s results…
The authors said the discrepancies likely stem from differences in sample processing, sequencing methods, bioinformatics pipelines, reference databases, reporting thresholds, and quality control standards…
“These tests have become popular, partly because people, I think, are increasingly interested in health and wellness, and partly because the gut microbiome has been linked — at least in the public imagination — to the idea that you can improve a whole range of conditions through diet and lifestyle changes,” said co-author Diane Hoffmann, MS, JD, of the University of Maryland in Baltimore.
“There’s been a lot of hype around that, but the hype doesn’t really match the evidence. These tests often have limited evidence behind them, especially when it comes to informing clinical decisions or even basic dietary recommendations,” she added. “So the marketing can be questionable, and consumers can end up misinterpreting or over-trusting results that aren’t very reliable.”
Related article from Houston Methodist Hospital (2024): Should You Do a Gut Microbiome Test? Key point: “While these tests seem to be effective in mapping the gut microbiome, there is currently no benchmark for what a ‘normal’ gut microbiome looks like. So the question becomes what to do with the results…microbiomes are highly variable — even normal, healthy ones. This makes it incredibly challenging to define the patterns or signatures that suggest a microbiome has become imbalanced. Plus, the at-home steps for correcting microbiome imbalance aren’t established either.”
My take: It is uncomfortable informing families that these gut microbiome tests have little clinical value because there is not a proper way to interpret the results. In addition, this study shows that the tests from one place to another produce wildly different results.
While one’s microbiome is important, we still don’t understand what exactly is a normal microbiome.
Related blog posts:
- Can We Predict Which Patients With Irritable Bowel Will Respond to Dietary Manipulation Based on Their Microbiome?
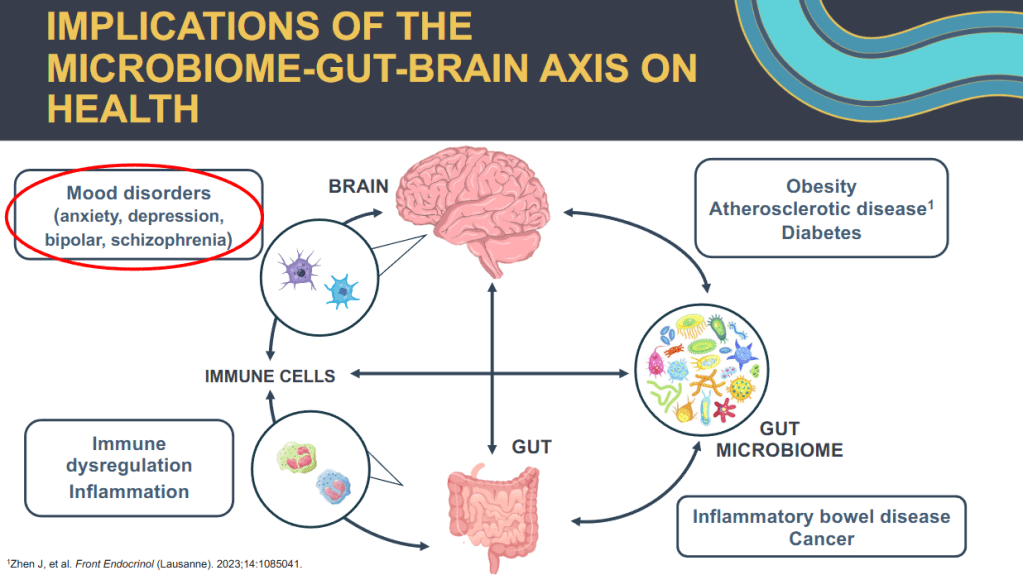
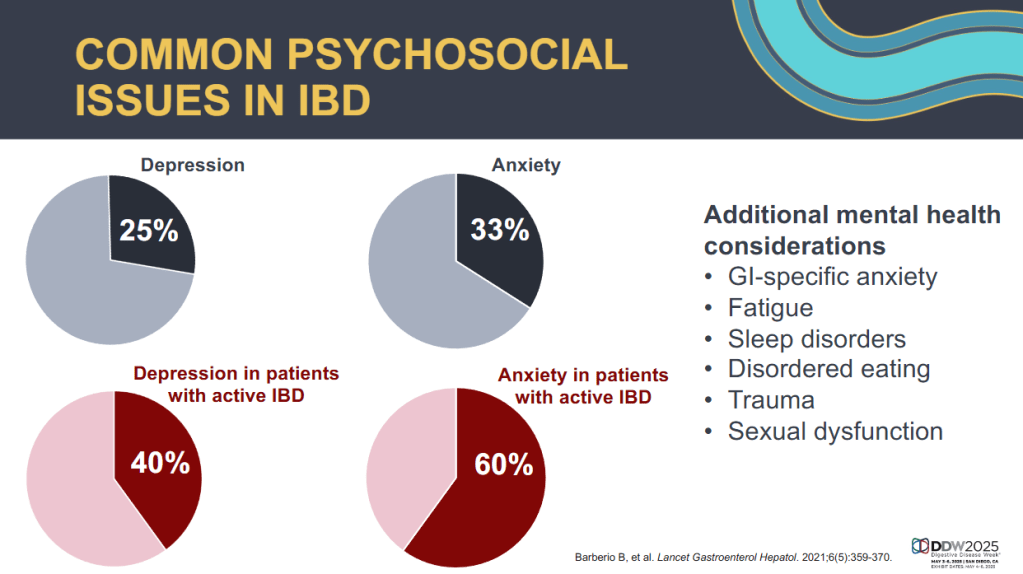
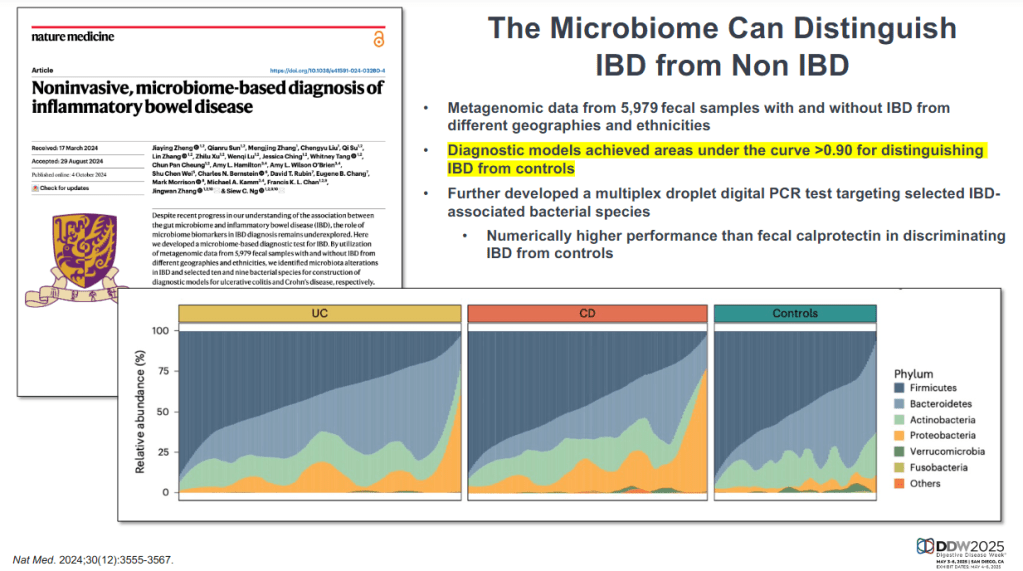
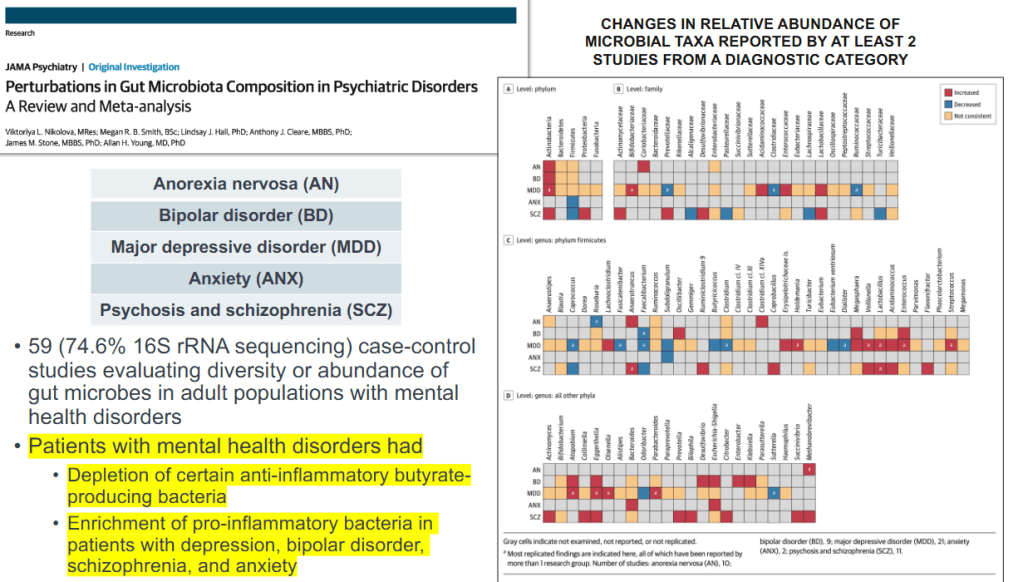
- David Rubin: Linking Inflammatory Bowel Disease and Mental Health Through the Gut Microbiome
- Rapid Gut Microbiome Recovery: Diet Outperforms Microbial Transplant
- Microbiome Therapy (SER-109) for Recurrent Clostrioides Difficile
- How Important is Your Microbiome for Weight Loss?
- Healthy Microbiome: A Work in Progress, Plus Microbiome-Drug Metabolism (2020)
- “There is No ‘Healthy’ Microbiome” (2014)