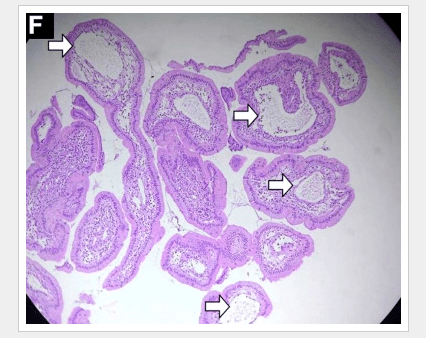
A small prospective study (M Manco et al. J Pediatr 2017; 180: 31-7) provides evidence that bariatric surgery/sleeve gastrectomy is effective at reversing nonalcoholic steatohepatitis (NASH) and hepatic fibrosis in adolescents (n=20).
All patients in this study had BMI >35 and weere 13-17 yrs of age.
Key findings at one year following intervention:
- Among the 20 patients who underwent sleeve gastrectomy, there was a 21.5% loss in baseline weight, which compared with weight loss of 3.4% among 20 patients who received intragastric balloon device and weight increase of 1.7% among 53 patients who received lifestyle intervention counseling.
- Sleeve gastrectomy group had resolution of NASH in all 20 and disappearance of hepatic fibrosis in 18 (90%). In the intragastric balloon group, NASH reverted in 24% and fibrosis in 37% whereas there was no improvement in the lifestyle intervention group.
Full text link: Sleeve Gastrectomy for NASH
Limitations are discussed in the editorial by Inge and Xanthakos (pgs 6-7) and included small sample size, absence of patients with type 2 diabetes, and short followup period. Nevertheless, this is “the largest and most informative series…in select adolescents with severe obesity.”
My take: Given the lack of effective pharmaceutical therapy and the typically impotent effects of lifestyle intervention, this data supports bariatric surgery to facilitate weight loss/NASH reversal in select adolescents.
Related article: JCF Leung et al. Hepatology 2017; 65: 54-64. This study showed that the histologic severity and clinical outcomes are modestly better in nonobese patients (n=72) with NAFLD compared with obese patients (n=307). High triglycerides and higher creatinine were associated with more advanced liver disease in nonobese patients.
Briefly noted: D Houghton et al. Clin Gastroenterol Hepatol 2017; 15: 96-102. This study with 24 subjects with nonalcoholic steatohepatitis showed that exercise reduced hepatic triglyceride content, visceral fat, and plasma triglycerides. However, circulating markers of inflammation and fibrosis was not reduced. The implication is that exercise should be part of NASH treatment but that weight management/diet are needed as well.
. Related blog posts:
- Adolescent Bariatric Outcomes
- Is a Three Year-Old Too Young for Bariatric Surgery …
- Reaching Consensus on Bariatric Intervention… | gutsandgrowth
- Trends in Adolescent Bariatric Surgery | gutsandgrowth
- Six year outcomes with bariatric surgery | gutsandgrowth
- Staggering cost of obesity | gutsandgrowth
- Two new drugs for obesity | gutsandgrowth
- Treating diabetes with surgery | gutsandgrowth
- Six years later-Mediterranean diet comes out on top | gutsandgrowth
- Childhood Obesity and Consensus Recommendations | gutsandgrowt
- Have you seen the Duodenal-Jejunal Bypass Liner? | gutsandgrowth