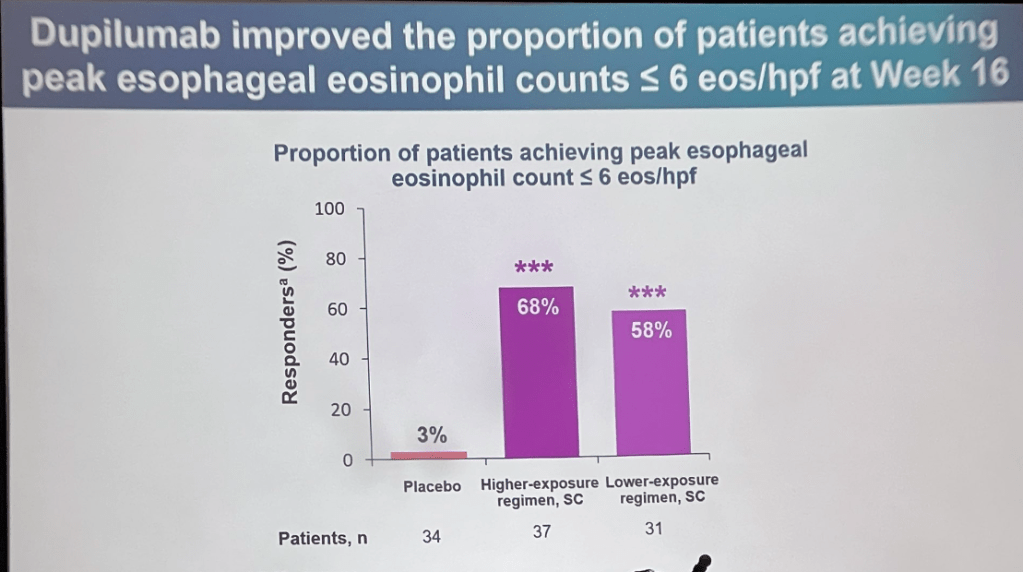
Dupixent Data in 1-11 year olds:

Rumination -clinical diagnosis:

Full text: M Halland et al Clinical Gastroenterol Hepatol 2018; 16: 1549-1555 provide an excellent review and practical recommendations for rumination syndrome.
The article describes the high prevalence which is ~0.8-0.9% of adults and ~5% of children. Some populations like patients with eating disorders and fibromyalgia have even higher rates.
Other key points:
My take: This is a useful review article. Rumination needs to be considered particularly in patients with regurgitation, often labelled vomiting by families, that happens quickly after meals.
Related posts:
In the news…from Washington Post:
A recent randomized, placebo-controlled cross-over study by A Pauweis et al (Am J Gastroenterol 2018; 113: 97-104) indicated that baclofen improved rumination syndrome in adults (mean age 42 years). Thanks to Ben Gold for this reference.
Baclofen (dosed at 10 mg TID) had the following effects:
My take: In this study, baclofen improved symptoms of rumination and regurgitation, but not supragastric belching.
Related posts:
Briefly noted: While in most cases, rumination syndrome does not require manometry for diagnosis, in cases of uncertainty, it can be helpful. A recent retrospective study (FR Grunder, A Aspirot, C Faure. JPGN 2017; 65: 627-32) highlights the utility of high-resolution esophageal manometry (HREM) in the diagnosis of rumination syndrome using 15 patients with rumination and 15 control patients.
Background: The sensitivity of HREM can be lower in a clinical setting as many “subjects with rumination are often able to tolerate the test meal during the manometry study with minimal or no symptoms.”
HREM also helps determine whether rumination is primary, secondary or if there is supragastric belch-associated rumination.
Key finding from this study:
My take: Manometry is usually not needed for the diagnosis of rumination syndrome but does help explain the pathophysiology.
More information from this year’s annual NASPGHAN meeting.
This blog entry has abbreviated/summarized this presentation. Though not intentional, some important material is likely to have been omitted; in addition, transcription errors are possible as well.
The following slides highlight a terrific lecture by Carlo DiLorenzo (Nationwide Children’s Hospital). Subsequently, I’ve included slides from Miranda van Tilburg (UNC); I was unable to attend her lecture and found some of the slides via twitter.
Key points:
From Miranda Tilburg:
J Monagas et al JPGN 2017; 64: 930-2 showed that among 30 patients with rumination (age 4 to 21 years) the rate of dental erosions was 77% (23 of 30) compared wtih 4 (13%) of the control subjects. My take: Patients with rumination should see their dentist.
Related post: Costs of Rumination
Reading a recent study (A Alioto et al. J Pediatr 2017; 185: 155-9) reminded me of “My Cousin Vinny.” In a crucial scene, Mona Lisa Vito (Marisa Tomei) proves that the accused killers were not the killers by identifying tire tread marks that were inconsistent with the defendants’ car simply by looking a photograph.
Similarly, the authors of this retrospective report highlight the extensive cost of that children undergo for evaluation of rumination when simple observation might suffice.
Key findings:
Limitations:
Other comments:
My take: Not every doctor is as good at doctoring as Vinny Gambini is at lawyering. That being said, the authors note “for patients who present with repeated effortless regurgitation and vomiting of food that begins soon after they eat or drink, is not preceded by retching, and does not occur during sleep, there are very few other diagnoses to be considered.”
Related blog posts:
Disclaimer: These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition.
Treatment options for rumination and for belching are limited. Baclofen improves symptoms and decreases events in both of these disorders (Clin Gastroenterol Hepatol 2012; 10: 379-84).
Rumination is characterized by effortless regurgitation of recently ingested food into the mouth (or beyond). It is easily mistaken for vomiting disorders and motility disturbances. With rumination, patients have retrograde flow of gastric contents into the esophagus through voluntary, though unintentional, abdominal muscle contractions with increased intragastric pressure increases.
Supragastric belching occurs when air is sucked into the esophagus by decreasing the intrathoracic pressure or by contracting pharyngeal muscles.
Baclofen is an agonist of the γ-aminobutyric acid B (GABA) receptor which results in increased lower esophageal sphincter (LES) pressures and reduced swallowing rates. Baclofen has been shown to improve reflux, mainly by reducing transient LES relaxations (TLESRs) but also by increasing basal LES pressures.
In the majority of patients, the mainstay of treatment has been behavioral which use diaphragmatic breathing to compete/extinguish these behaviors. There are a shortage of therapists familiar with this approach. As such, alternative treatments are needed. In this study, high-resolution manometry-impendance recordings were taken from 16 patients (10 women; mean age 43 years; range 18-89 years); eight of the patients had rumination. Only 12 patients were included in the final analysis; four patients refused repeat manometry. Manometry was performed before and after treatment along with recording symptoms. Both symptoms and manometry recordings improved with Baclofen therapy. This was a one-week open-label study. Baclofen was dosed at 10 mg TID. At baseline the total number of “flow events” was 473; after treatment, this was reduced to 282 events. In total, rumination events decreased by 68% during treatment. This improvement correlated with increased LES pressures.
Four of the 12 patients reported mild side effects mainly sleepiness and difficulty concentrating.
Additional references:
Additional Baclofen references: