KO Hensel et al. J Pediatr 2021; 238: 50-56. Sclerosing Cholangitis in Pediatric Inflammatory Bowel Disease: Early Diagnosis and Management Affect Clinical Outcome
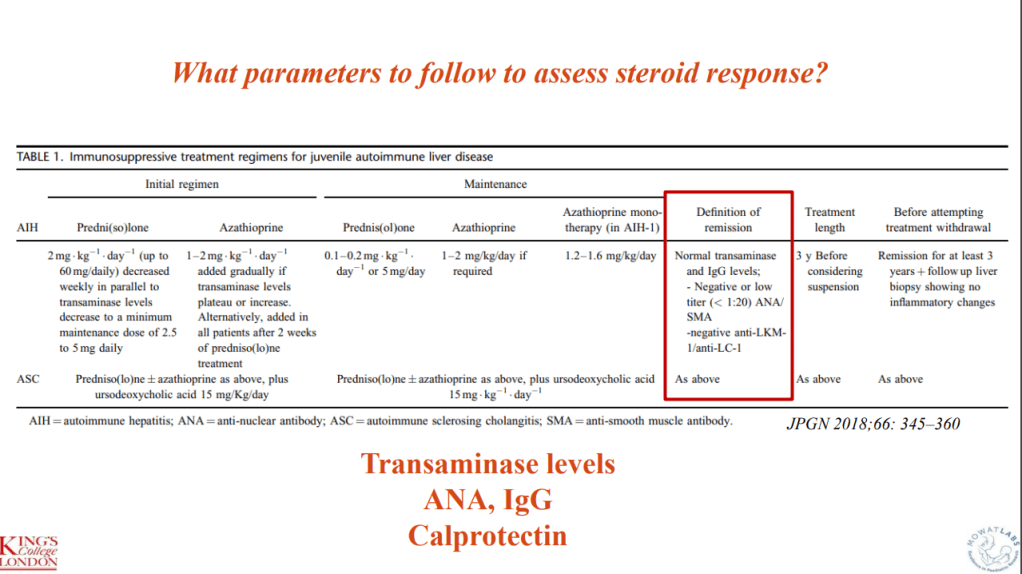
This was a retrospective study of 82 pediatric patients (31% female) with IBD-SC and a mean age at diagnosis of 11.9 ± 2.8 years who were followed up for a mean of 6.8 ± 3.3 years. Tests for SC included immunoglobulins and serology (ANA, ASMA, LKM-1, and SLA). Patients with ASC were maintained on low dose prednisolone (5 mg/day) and azathioprine (up to 2 mg/kg/day).
Key findings:
- Autoimmune SC (ASC) was diagnosed in 72%, and small duct SC was diagnosed in 28%
- Complication-free and native liver survival were 96% and 100%, respectively, at 5 years after diagnosis and 75% and 88%, respectively, at 10 years after diagnosis
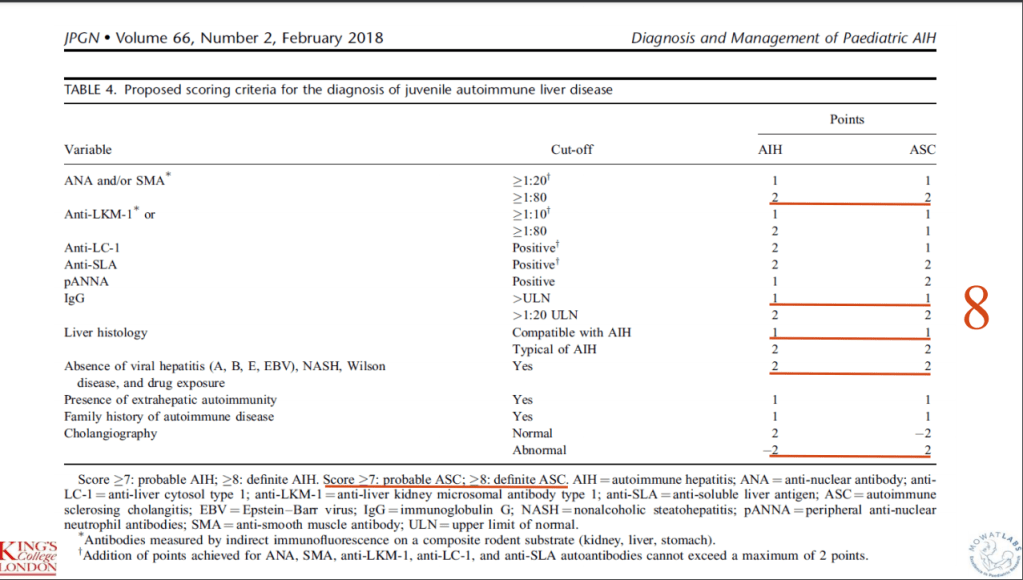
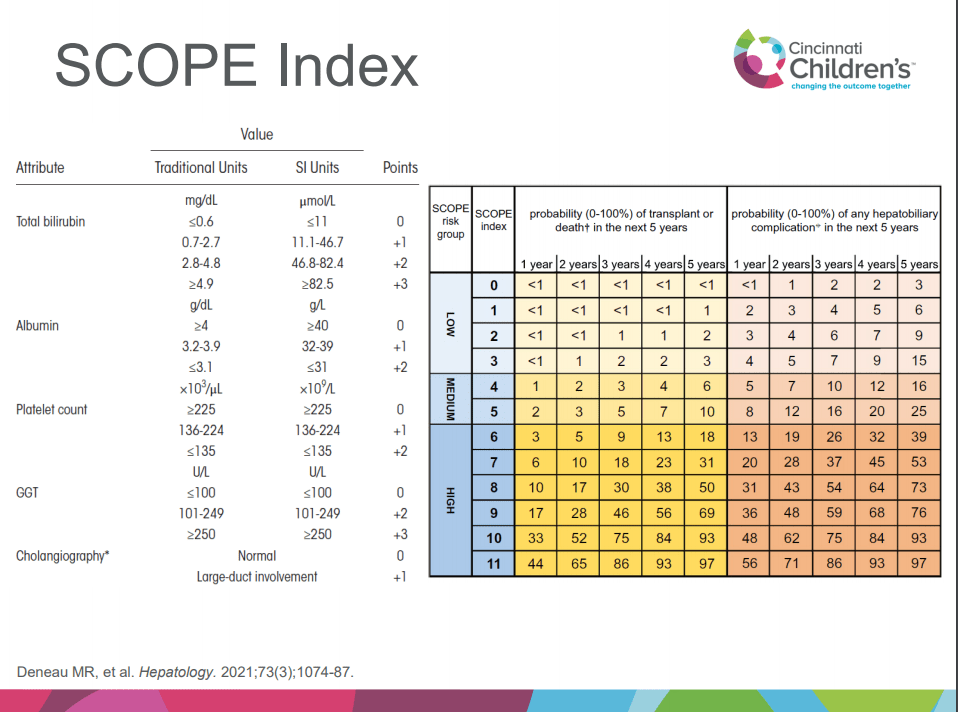
The discussion notes generally better outcomes in this cohort than in previous studies. The authors note that this may be due to earlier diagnosis (though lead-time bias could be a factor as well). To increase earlier diagnosis, the gastroenterology diagnostic pathway at one institution (CUH) includes mandatory assessment of liver function and a low threshold for performing a liver biopsy (with initial panendoscopy). Diagnosis of ASC was based on the ESPGHAN diagnostic score for AILD (JPGN 2018; 66: 345-360, related post has image with scoring: Aspen Webinar 2021 Part 5 -Autoimmune Liver Disease & PSC). Also, they note that SCOPE score “seemed to overestimate the risk for developing complications.”
My take: In those with IBD and abnormal liver enzymes/GGT, looking for SC/ASC may improve outcomes.
Related blog posts:
- Aspen Webinar 2021 Part 5 -Autoimmune Liver Disease & PSC
- Active Colitis More Likely in Children in Clinical Remission Who Have PSC and IBD
- How Primary Sclerosing Cholangitis Alters Outcomes in Inflammatory Bowel Disease
- Big Study of PSC in Children
- PSC -Natural History Study (pediatric)
- Primary Sclerosing Cholangitis (PSC) –Natural History Study