We are getting a lot of calls from families trying to figure out what they should be doing for their children with inflammatory bowel disease in regards to school attendance. Here is what our ICN team has developed:
School guidance during Covid pandemic:
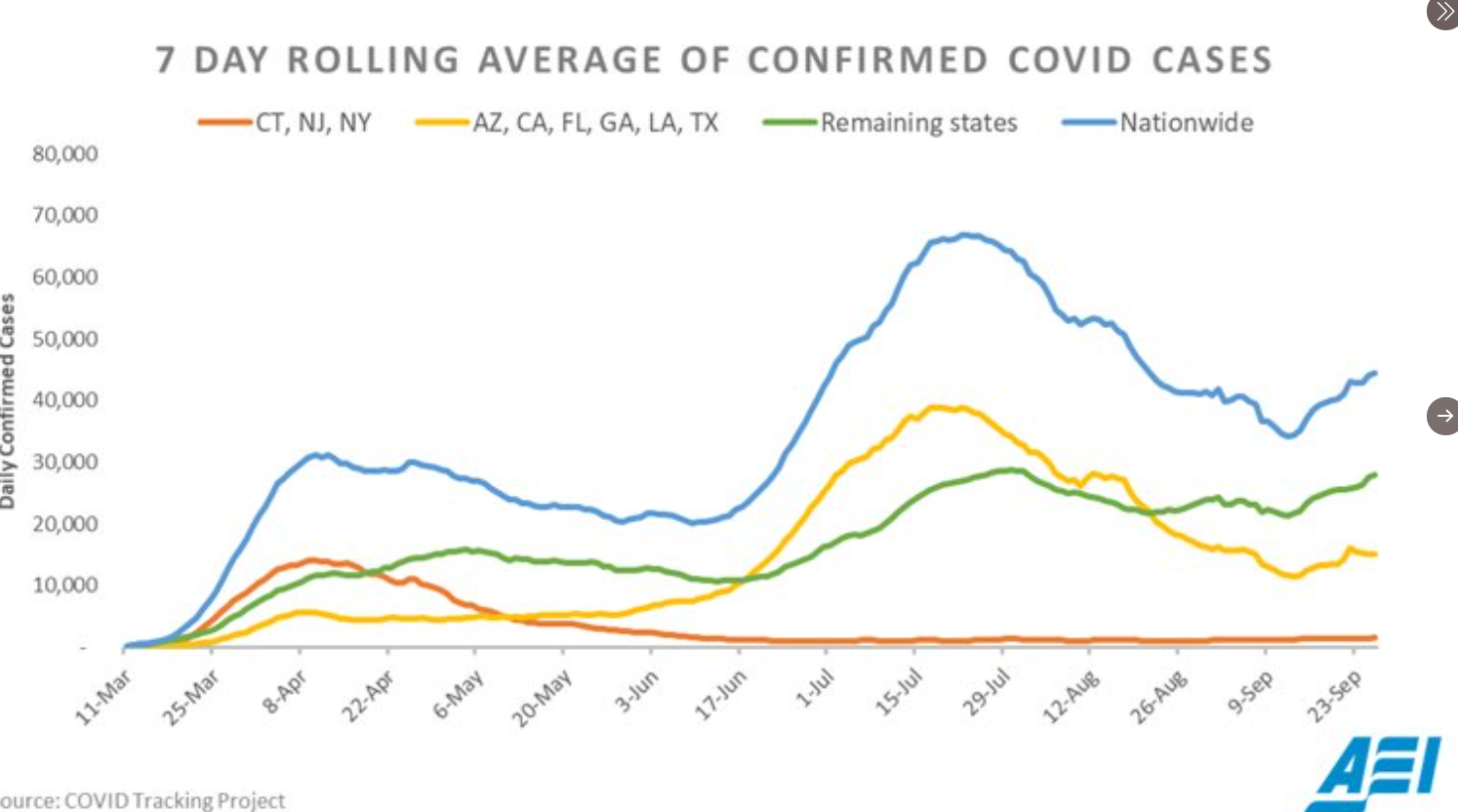
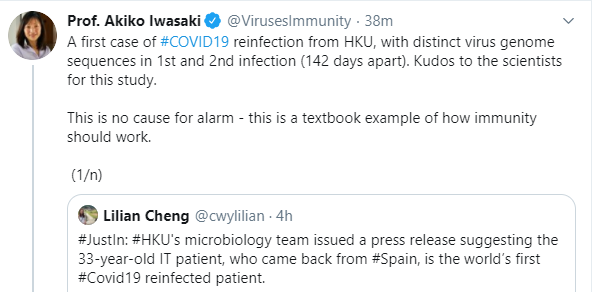
With the flood of information in the lay and scientific media, GI Care for Kids wanted to assure that our patients and families who had children with inflammatory bowel disease (IBD), Crohn’s or ulcerative colitis, had some guidance in making important decisions about beginning the 2020-2021 school year. Currently, research shows that just having IBD, DOES NOT put a person more at risk for acquiring (i.e. catching) coronavirus (COVID-19) infection. In addition, research suggests that biologics (e.g. Remicade, Humira) DO NOT seem to increase the risk for more severe Covid related illnesses.
However, steroids, thiopurines (e.g. 6-MP; azathioprine, immuran) and prograf DO appear to have a larger effect on increasing risk for more severe coronavirus infection and COVID-19 disease. Additional research is being carried out with oldest patients (e.g. > 65 years of age) who appear to be at increased risk for infection and COVID-related disease, and, other co-morbid conditions (e.g. obesity, diabetes, cardiovascular disease) being at highest risk for COVID-19 disease as well.
All patients should practice good hand hygiene, wear masks at all times outside of the house, and observe social distancing. If your family does not feel that return to a traditional school building is in your child’s best interest, please let us know, and we will help make sure we support you from a medical standpoint.
For further information on the status of coronavirus in people with IBD world-wide, young or old, please go to: www.covidibd.org.
Additional information about the status of COVID-19 can be found at the following websites:
Also, this:
Facebook link (1:22 min): This is what happens when a Special Effects guy stays at home with his son during lockdown
Disclaimer: This blog, gutsandgrowth, assumes no responsibility for any use or operation of any method, product, instruction, concept or idea contained in the material herein or for any injury or damage to persons or property (whether products liability, negligence or otherwise) resulting from such use or operation. These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. Because of rapid advances in the medical sciences, the gutsandgrowth blog cautions that independent verification should be made of diagnosis and drug dosages. The reader is solely responsible for the conduct of any suggested test or procedure. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition