For medication administration, there are five “rights” that are needed for optimal results:
- Right drug
- Right dose
- Right route (e.g., oral, intravenous, topical)
- Right patient
- Right time
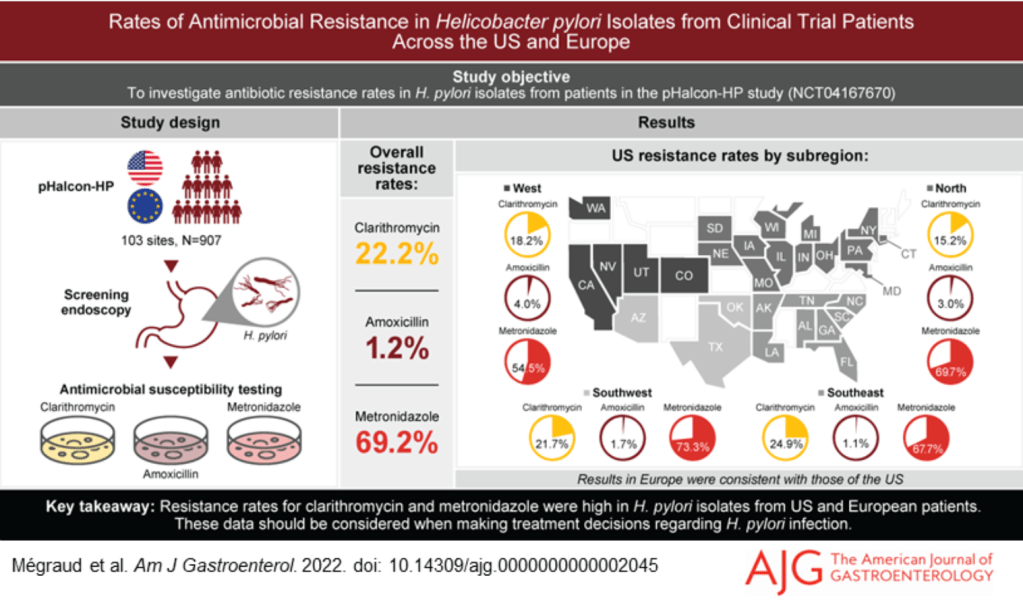
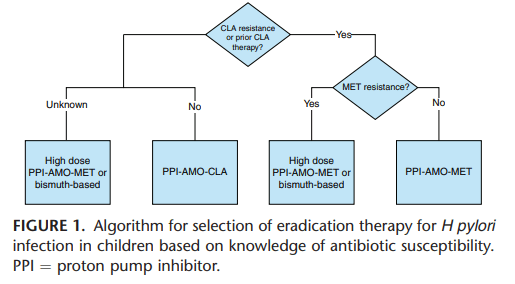
The recent article below highlights the fact that the “right drug” for H pylori can be dependent on resistance patterns. Previous articles (see below) have shown that the right dose is equally-important to improve cure rates.
C Chan et al. J Pediatr Gastroenterol Nutr. 2025;81:1133–1141. Antimicrobial susceptibility-guided treatment is superior to empiric therapy for Helicobacter pylori infection in children
Methods: Retrospective study with 218 children who had histologically-proven H pylori infection. Susceptibility-guided treatment (SGT) was given to 123 and empiric therapy (ET) to 95. Testing for susceptibility was via a send-out assay to an outside specialty laboratory (Mayo Clinic Laboratories).
Key findings:
- Eradication success was significantly higher in the SGT group (89.4%,110/121) compared to the ET group (70.2%, 66/94) (p < 0.001).
- Amoxicillin resistance was strongly associated with failure (27.3% vs. 0.9%, p = 0.002), as was dual clarithromycin-metronidazole resistance (36.4% vs. 8.2%, p = 0.018).
My take: This study shows the huge improvement when therapy is adjusted based on known susceptibility.
Related blog posts:
- Give the Right Dose (for H pylori) -It Works Better!
- Dr. Benjamin Gold: 2024 Pediatric H pylori Guidelines (Part One)
- Dr. Benjamin Gold: 2024 Pediatric H pylori Guidelines (Part 2)
- Excellent Review of H Pylori in Children Plus One on Healthy Aging
- Brief Updates: H pylori Resistance Rates, VEDOKIDS, Increasing Bariatric Surgery in Kids

Also, more on changes to CDC website:
Benjamin Mazer, The Atlantic; 11/21/25: Open Access! Do Childhood Vaccines Cause Tornadoes? It hasn’t been ruled out (Related blog post: CDC Website Changed to Include False Claims About Autism and Vaccines)