The Children’s Care Network (in Atlanta) has recently shared its Spring 2022 Clinical Quality Forum. Following is the link to the video recording. The poll during the live presentation is not active for the recording.
- Meeting video via YouTube
- More resources at www.tccn-choa.org
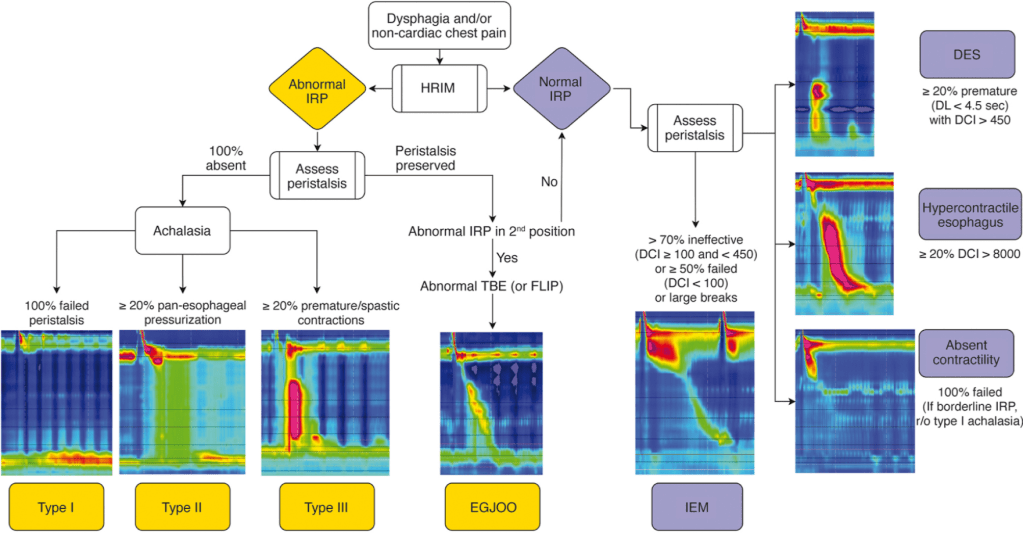
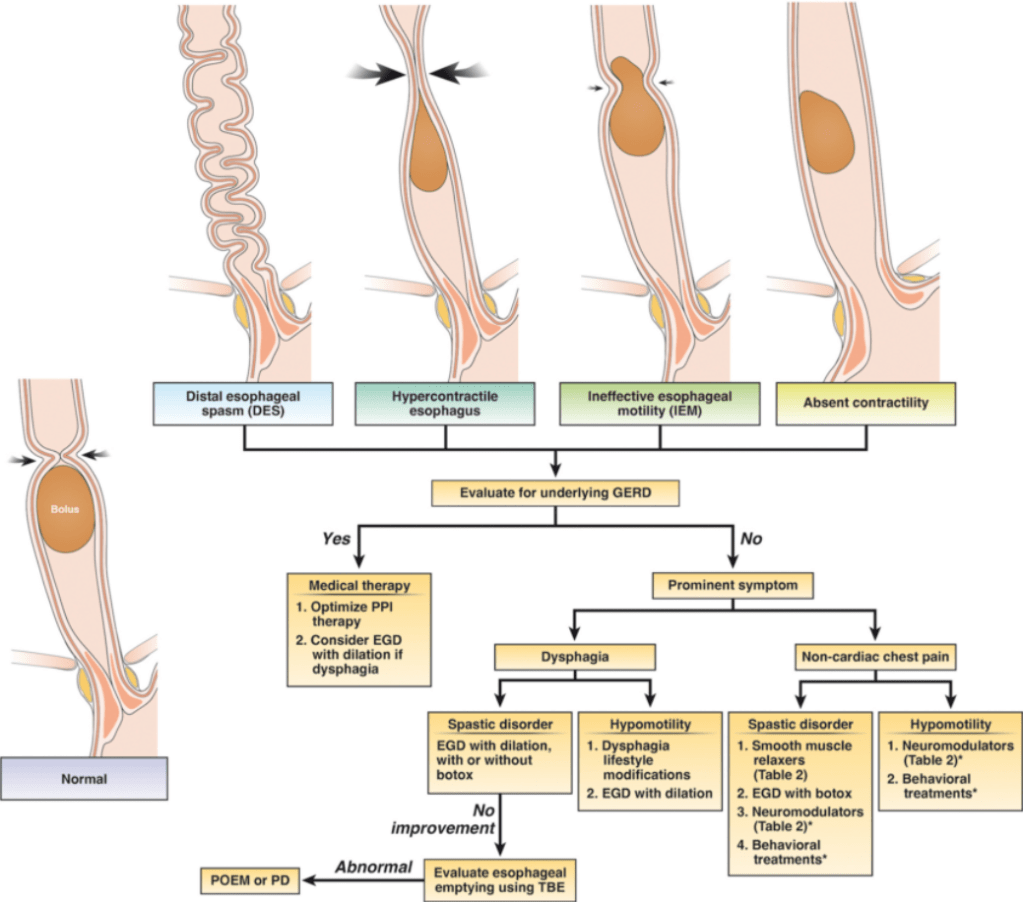
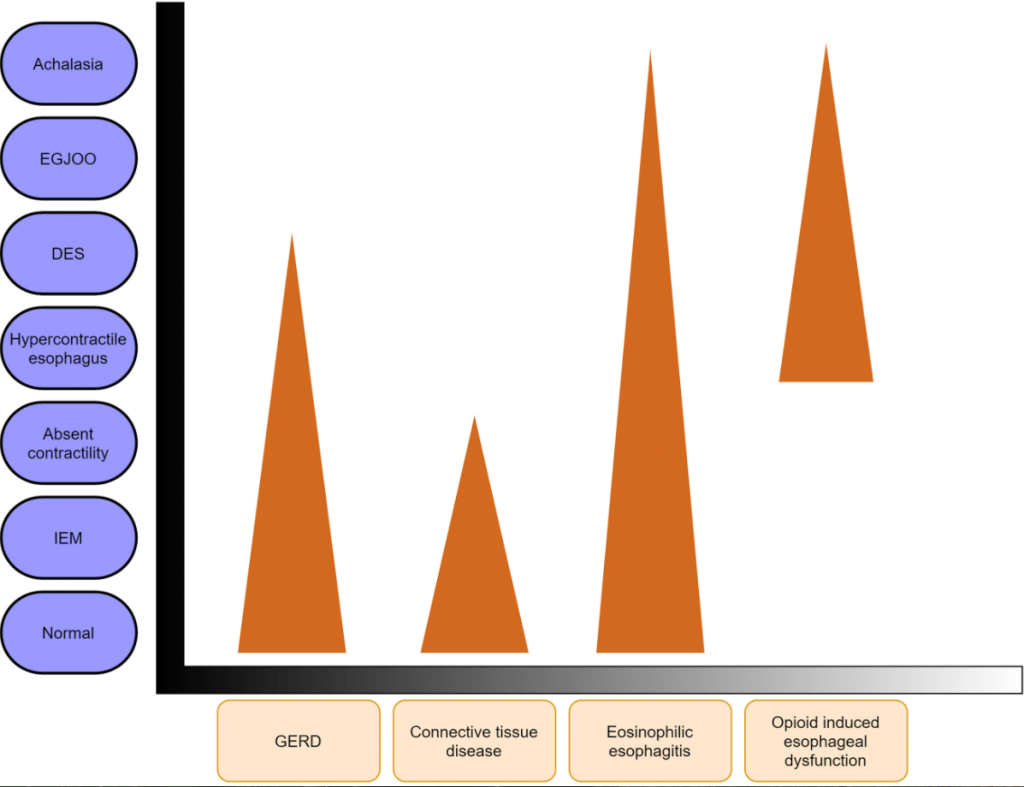
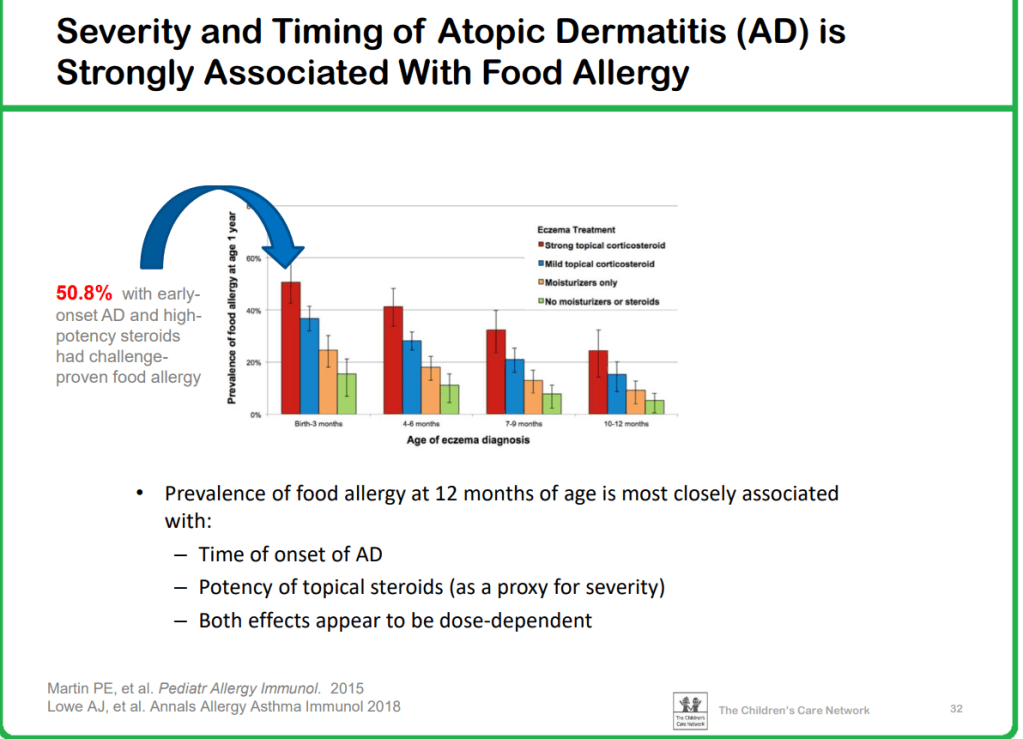
Some of the slides that I think are most helpful are shown below (used with permission). This 2nd part of content is from Dr. Brian Vickery which describes the relationship of atopic dermatitis to food allergy and best practices for prevention of food allergy:



ASCIA Handouts:


Related blog posts:
- Eczema Rarely Linked to Food Allergy
- “The Truth About Allergies and Food Sensitivity Tests”
- The Peanut Story -From NEJM Blog
- Peanut Allergy Prevention Guidelines | gutsandgrowth
- The “EAT” Study | gutsandgrowth
- Poorly-Conceived Allergy Testing Can Lead to Unnecessary Diet Restrictions and Complications
- What’s Wrong with “I Want My Kid Tested For Food Allergies” | gutsandgrowth
- How Allergy Testing Can Lead to More Allergies
Disclaimer: This blog, gutsandgrowth, assumes no responsibility for any use or operation of any method, product, instruction, concept or idea contained in the material herein or for any injury or damage to persons or property (whether products liability, negligence or otherwise) resulting from such use or operation. These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. Because of rapid advances in the medical sciences, the gutsandgrowth blog cautions that independent verification should be made of diagnosis and drug dosages. The reader is solely responsible for the conduct of any suggested test or procedure. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition