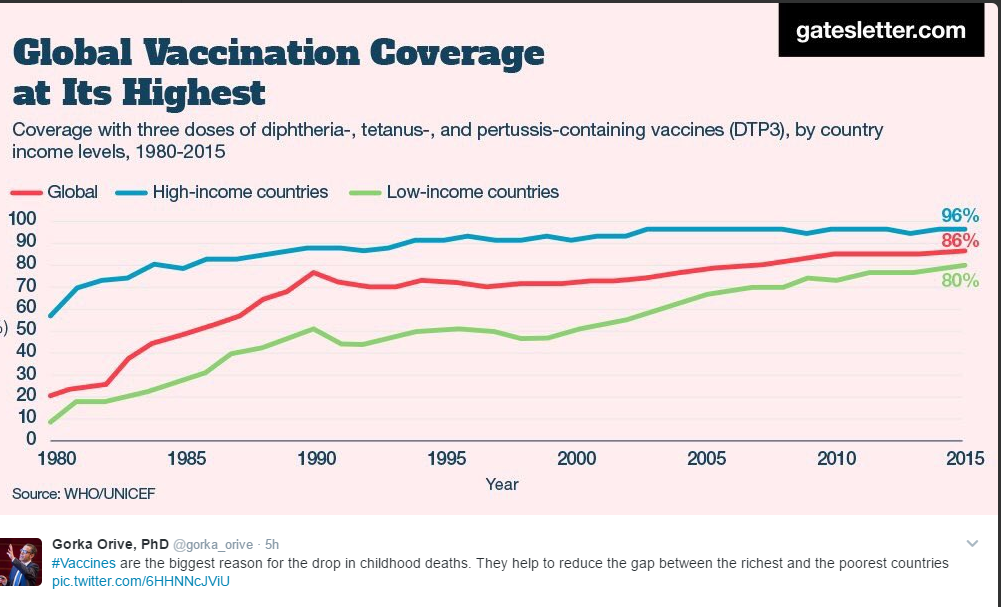
C Schulthei et al. Hepatology 2021; 73: 1436-1448. Full text: Next-Generation Immunosequencing Reveals Pathological T-Cell Architecture in Autoimmune Hepatitis
This is highly technical study of 60 patients with AIH. “Our key finding was a clearly biased signature of TRBV-J gene usage in peripheral and liver-infiltrating T-cells of patients with AIH, independent of AIH predisposing HLA-DRB1 alleles. This signature was unaffected by immunosuppressive treatment and not related to complete biochemical disease remission. This suggests that treatment acted on T-cell functionality rather than on the underlying pathological T-cell architecture in this disease that has a high relapse rate.”
My take (borrowed from authors): “Patients with AIH show profound and persisting T-cell architectural changes that may explain high relapse rates after tapering immunosuppression.”
Related blog posts:
- Predicting Outcomes in Childhood Autoimmune Hepatitis
- Autoimmune Hepatitis -Early Response Associated with Remission
- Online Aspen Webinar -Autoimmune Hepatitis
- Using Less Steroids for AIH
- Steroid-Free Approach in Autoimmune Hepatitis
- Azathioprine metabolite measurement for Autoimmune Hepatitis | gutsandgrowth
- Adult versus Pediatric Data: Autoimmune Hepatitis | gutsandgrowth
- Genetics of Autoimmune Hepatitis | gutsandgrowth
- Diagnosing autoimmune hepatitis
LF Chun et al. J Pediatr 2021; 233: 105-111. Hepatic Steatosis is Negatively Associated with Bone Mineral Density in Children
Key findings:
- Using a community-based sample of 235 children, the authors found that there was a significant negative relationship between liver MRI-PDFF and BMD z score R = −0.421, P < .001).
- There was no significant association between vitamin D status and BMD z score (P = .94).
- Children with clinically low BMD z scores were found to have higher alanine aminotransferase (P < .05) and gamma-glutamyl transferase (P < .05) levels compared with children with normal BMD z scores.
My take: This study shows another organ that is affected in children with fatty liver disease; other associated problems include increased risk for cardiovascular disorders, pancreatic dysfunction/diabetes, cancer, polycystic ovary syndrome, and neurologic disorders
Related blog posts:
- Best Practice for Fatty Liver Disease
- ASPEN Webinar on NAFLD and NASH
- The Paramount Health Challenge for Humans in the 21st Century
- How Often Do Children with Obesity Have a Fatty Liver?
- Pediatric NAFLD: You Don’t Have to be Obese/Overweight to have Fatty Liver Disease (but it helps)
- Should Teenagers with Severe NAFLD Undergo Bariatric Surgery?
- Concise Review: Fatty Liver in Pediatrics
Image below near the Seven Mile Road on the Florida Keys: