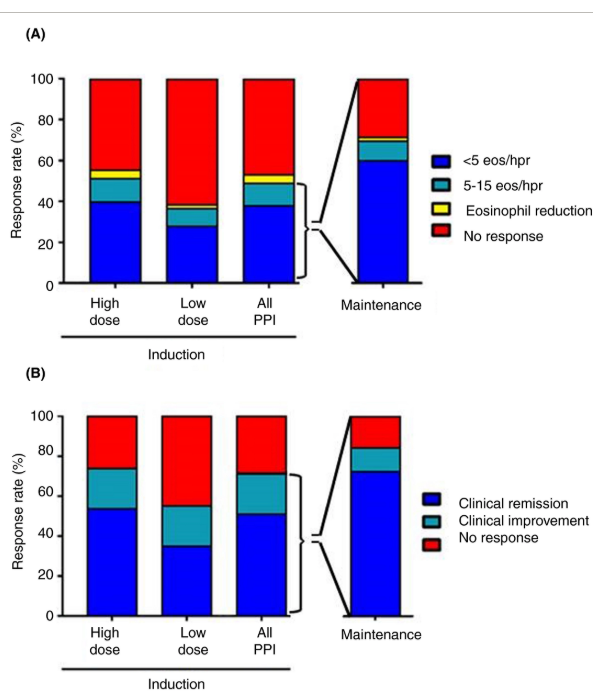
DA Hartnett et al. Clin Gastroenterol Hepatol 2026; 24: 375-384. Open Access! Distribution of Esophageal Eosinophilia as a Predictor of Proton Pump Inhibitor Response in Eosinophilic Esophagitis
Methods: This was a retrospective cohort study of newly diagnosed adult patients with EoE — All patients received ≥8-week PPI trial and underwent repeat biopsies to assess response. There were including 66 with isolated distal and 200 with proximal/diffuse disease. 86% of patients received twice daily PPI therapy (73% in those with isolated distal disease and 87% in the diffuse/isolated proximal disease.
Key findings:
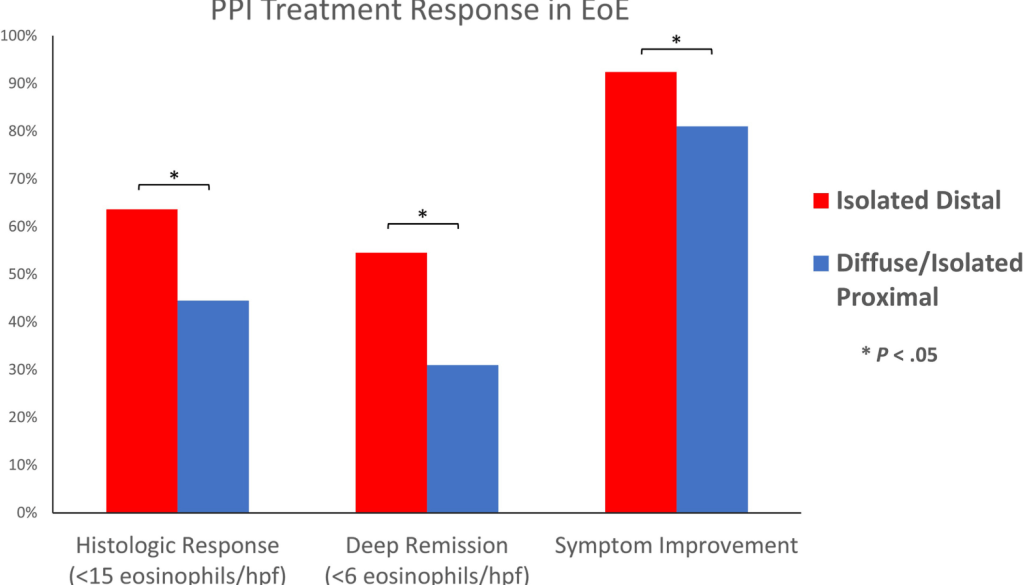
PPI response was higher among patients with isolated distal disease:
- histologic remission [<15 eosinophils/hpf post-PPI]: 63.6% vs 44.5%; P = .01
- deep remission [<6 eosinophils/hpf]: 54.5% vs 31.0%; P = .001
- symptom improvement: 92.4% vs 81.0%; P = .03).
The discussion noted that there has been limited studies of EoE distribution and response to treatment. “Godat et al observed that the distribution of esophageal eosinophilia had no impact on clinicohistologic remission rates (defined as ≤2 on a scale of 0–10 for dysphagia/odynophagia in the last 7 days and a peak eosinophil count <5 eos/hpf) in patients treated with budesonide orodispersible tablets.19“
“The generally higher PPI response with isolated/predominant distal disease suggests that acid suppression and improved mucosal barrier function likely play a key role in how PPI may lead to EoE remission…prior studies have demonstrated no correlation between findings on ambulatory pH monitoring and PPI response in EoE.25 Therefore, the differential response to PPI based on eosinophil distribution phenotypes may be due to more than comorbid GERD alone.”
My take: While the pathophysiology of how PPIs work for EoE is unclear, it appears that the response to PPIs is better with in those with isolated distal EoE. The difference in response may have been even more pronounced if both groups had a similar percentage of receiving twice daily PPI treatment.
Related blog posts:
- Updated Data on PPI Effectiveness For Eosinophilic Esophagitis
- How Effective Are PPIs for Eosinophilic Esophagitis?
- Practical Tips for Eosinophilic Esophagitis (2024 with Dr. Glen Furuta)
- ACG 2025 Guidelines for Eosinophilic Esophagitis
- How Genetics Influence Response to PPIs in Eosinophilic Esophagitis
- What is EoE?
- Dupilumab: FDA Approval for Eosinophilic Esophagitis
- Expecting Change in Eosinophilic Esophagitis Treatment | gutsandgrowth
- 4-14-4 Rule: More Biopsies Recommended for EoE
- ESPGHAN Eosinophilic Esophagitis Guidelines