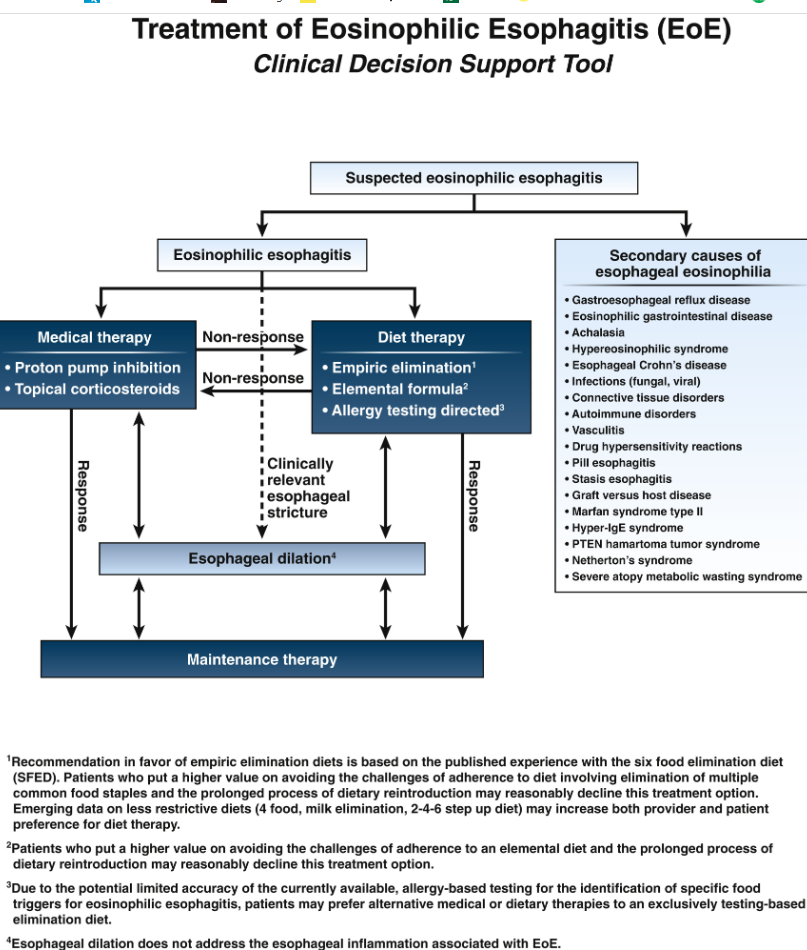
CC Reed et al. Clinical Gastroenterology and Hepatology 2025; Worsening Disease Severity as Measured by I-SEE Associates With Decreased Treatment Response to Topical Steroids in Eosinophilic Esophagitis Patients
This was a retrospective study with children and adults with eosinophilic esophagitis (EoE). Among 1312 patients, there were 657 (50%), 461 (35%), and 194 (15%) with mild, moderate, and severe disease by I-SEE, respectively. Disease activity was categorized as mild (I-SEE 1–6), moderate (I-SEE 7–14), or severe (I-SEE ≥15).
Key findings:
- Patients with severe disease were less likely to have histologic response (49% (severe) vs 55% (moderate) vs 64% (mild); P = .03 for <15 eosinophils per high-power field)
- Patients with severe EoE also had lower global symptom response rates (53% vs 79% vs 83%, respectively) and higher post-treatment EoE Endoscopic Reference Scores (EREFS; 3.6 ± 2.3 vs 2.4 ± 1.8 vs 1.6 ± 1.6, respectively)
My take: More severe disease is harder to treat with EoE (and most everything else too).
Related blog posts:
- I-SEE for Eosinophilic Esophagitis (has pictures and table to calculate I-SEE score)
- I-SEE (Index of Severity for Eosinophilic Esophagitis) Works in Kids TooPractical Tips for Eosinophilic Esophagitis
- AGA: High Quality Upper Endoscopy
- “Esophageal Hypervigilance” and Outcomes in Eosinophilic Esophagitis
- “Real-World” Dupilumab for Eosinophilic Esophagitis
Link: I-SEE Tool Scoring Table