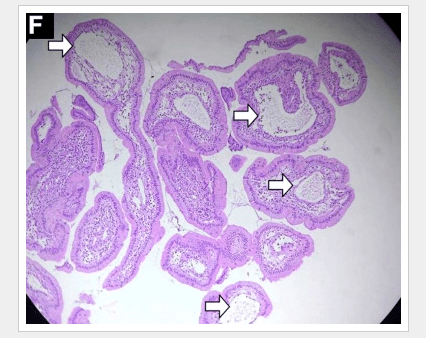
Did you know that Remicade and Humira are orphan drugs? For those concerned about pharmaceutical costs, a recent NPR article is a must.
From NPR: Drugs For Rare Diseases Have Become Uncommonly Rich Monopolies
Here’s an excerpt:
Lucrative financial incentives created by the Orphan Drug Act signed into law by President Reagan in 1983 succeeded far beyond anyone’s expectations. More than 200 companies have brought almost 450 so-called orphan drugs to market since the law took effect.
Yet a Kaiser Health News investigation shows that the system intended to help desperate patients is being manipulated by drugmakers to maximize profits and to protect niche markets for medicines already being taken by millions. The companies aren’t breaking the law but they are using the Orphan Drug Act to their advantage in ways that its architects say they didn’t foresee or intend. Today, many orphan medicines, originally developed to treat diseases affecting fewer than 200,000 people, come with astronomical price tags…
More than 70 were drugs first approved by the Food and Drug Administration for mass market use. These medicines, some with familiar brand names, were later approved as orphans. In each case, their manufacturers received millions of dollars in government incentives plus seven years of exclusive rights to treat that rare disease, or a monopoly…
When a drugmaker wins approval of a medicine for an orphan disease, the company gets seven years of exclusive rights to the marketplace, which means the FDA won’t approve another version to treat that rare disease for seven years, even if the brand name company’s patent has run out. The exclusivity is compensation for developing a drug designed for a small number of patients whose total sales weren’t expected to be that profitable…
Industry-wide, orphan drug tax credits cost the federal government $1.76 billion in fiscal 2016
My take: Any objective observer would recognize that the goals of the Orphan Drug Act are being subverted by current practice and changes are needed to achieve the goals of targeting rare diseases and reasonable medication costs.

Related blog posts: