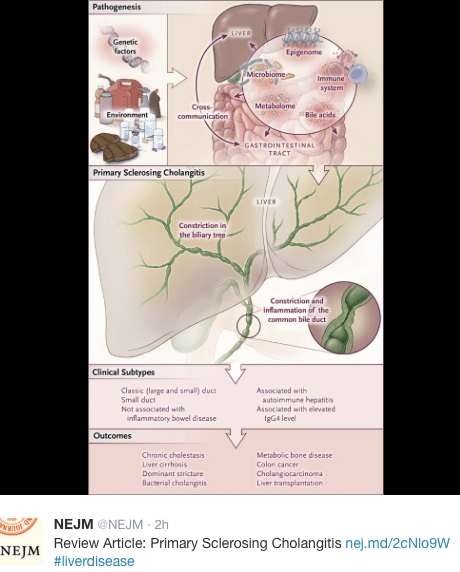
A recent study (AK Lunder et al. Gastroenterol 2016; 151: 660-69, editorial 590-3) provides more information about the prevalence of subclinical primary sclerosing cholangitis (PSC) in the setting of long-term inflammatory bowel disease. From a cohort of 756 Norwegian patients in the “IBSEN” cohort of patients with inflammatory bowel disease, the authors analyzed 327 patients with magnetic resonance cholangiography (MRC).
Key findings:
- 24 (7.5%) of 327 patients who had been followed for 20 years were found to have PSC lesions. Only 7 (2.2%) were known to have PSC based on biochemical or clinical features. Subsequently, a missed case of small-duct PSC was recognized increasing the rate to 8.1%.
- Subclinical PSC, interestingly, was detected more often in Crohn’s patients (9.0%) compared with ulcerative colitis (6.8%)
- Extensive colitis, high prevalence of colectomy, and refractory IBD symptoms were more common in patients with suspected PSC compared with those without PSC features (P= .029, P= .002, and P= .012 respectively)
The natural history of these subclinical cases of PSC is unclear. Studies have shown that patients with PSC with normal alkaline phosphatase values have an excellent outlook. Yet, there should be some concern. PSC has been associated with 400-fold higher chance of cholangiocarcinoma and 5-fold increased risk of developing colorectal cancer. This could indicate the need for more intensive surveillance in these patients –though the exact risks in those with subclinical disease is unknown.
My take: Until we know more, I doubt looking for subclinical PSC makes sense outside research protocols.
Related blog posts:
- Screening for subclinical PSC in IBD? | gutsandgrowth
- Vedolizumab for Primary Sclerosing Cholangitis (with … – gutsandgrowth
- Population-based outcomes for PSC gutsandgrowth
- Colonic disease and PSC | gutsandgrowth
- Challenges with primary sclerosing cholangitis | gutsandgrowth Numerous references with this blog post.
- PSC 2013 Review | gutsandgrowth