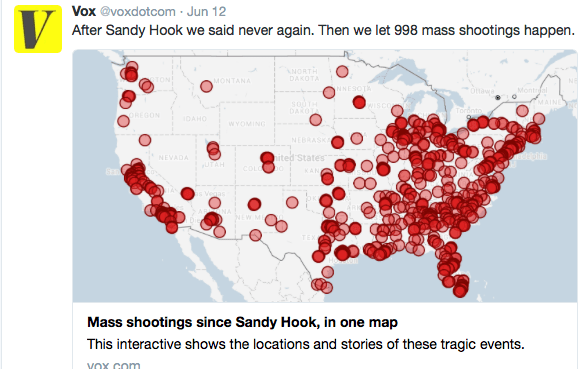
A recent study (EK Wright et al. Inflamm Bowel Dis 2016; 22: 1086-94) collected data from 135 participants in a prospective, randomized, controlled trial aimed at preventing postoperative Crohn’s disease (CD) recurrence. As part of this study, serial stool collections enabled comparison of fecal markers: calprotectin (FC), lactoferrin (FL) and S100A12 (FS).
FC was the optimal marker and was superior to CRP and CDAI. Table 4 provides a list of sensitivity, specificity, PPV, and NPV for each of the fecal markers at various cutoffs.
For FC, using the optimal cutoff of 135 mcg/g, the sensitivity was 0.87, specificity was 0.66, PPV was 56%, and NPV 91%. A lower cutoff (50 mcg/g) improved sensitivity to 0.96 and NPV to 94%; whereas a higher cutoff (200 mcg/g) lowered the sensitivity to 71% but improved the specificity to 0.74 along with raising the PPV% to 59%.
My take: While the yield of a test changes based on the population examined, this report indicates that it is likely that calprotectin would outperform the other fecal inflammatory markers in most settings.
Related blog posts:
Briefly noted: G Gale et al. Inflamm Bowel Dis 2016; 22: 1071-77. This report describes more extensive disease when there is concomitant orofacial granulomatosis with Crohn’s disease.