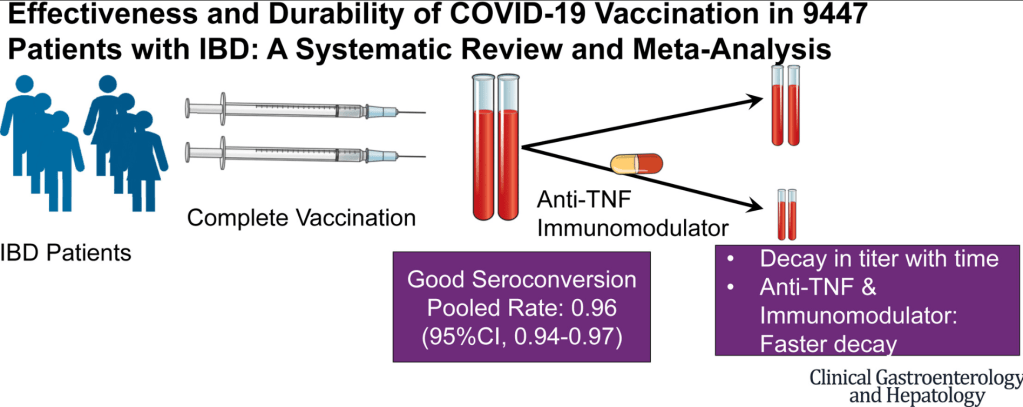
A Jena et al. Clin Gastroenterol Hepatol 2022; 20: 1456-1479. Open access: Effectiveness and Durability of COVID-19 Vaccination in 9447 Patients With IBD: A Systematic Review and Meta-Analysis
This was a systematic review and meta-analysis that included 46 studies.
- Key findings:
In 9,447 subjects who were completely vaccinated, the pooled seroconversion relative risk was 0.96 (95%CI, 0.94-0.97), and was higher for mRNA vaccines (0.97, 95%CI 0.96-0.98) than for adeno-associated vaccines (0.87, 95%CI: 0.78-0.93) - The pooled seroconversion rates were similar regardless of IBD therapy, and ranged from 0.93 to 0.99.
- The pooled relative risk of breakthrough COVID-19 infections in vaccinated patients with IBD was not significantly different from that of vaccinated controls. However, a decay in antibody titers after 4 weeks from vaccination appeared to be accelerated in those on anti-TNF agents, immunomodulators or their combination.
My take: IBD patients benefit from complete COVID-19 vaccination similar to healthy controls.
Related blog post: COVID Booster Advice for IBD from Dr. David Rubin (@IBDMD)
NB Halasa et al. NEJM 2022; 387: 109-119. Open access: Maternal Vaccination and Risk of Hospitalization for Covid-19 among Infants
Using a case-control design, the authors found that complete (2 dose) vaccination during pregnancy —Key findings:
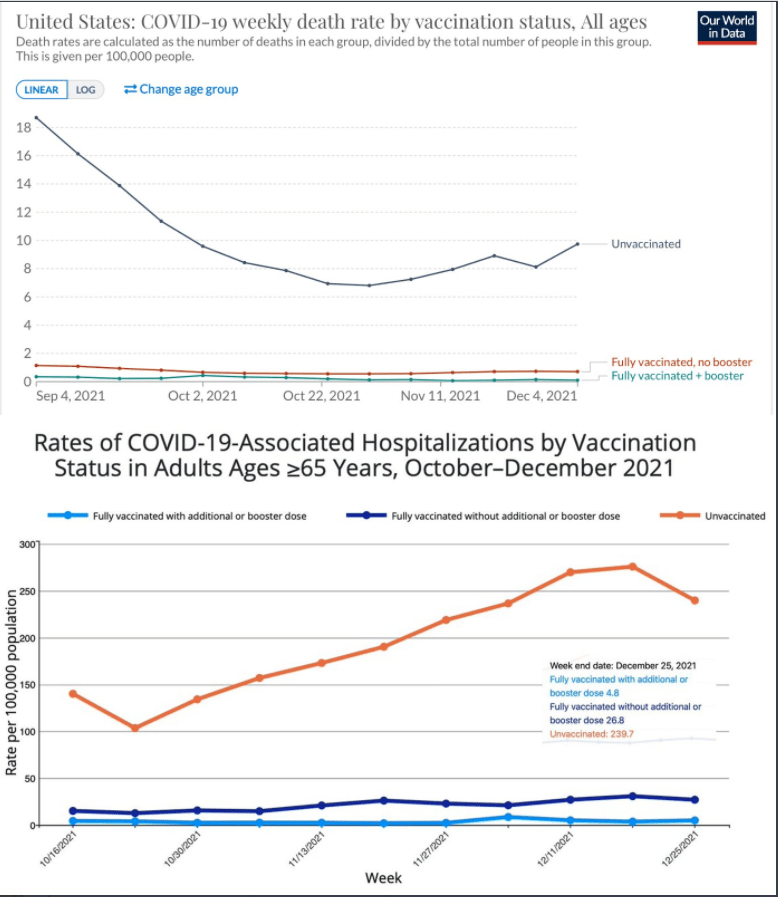
- The effectiveness of maternal vaccination against hospitalization for Covid-19 among infants < 6 months was 52% overall, 80% during the delta period, and 38% during the omicron period.
My take: Vaccination protects mother and infant. “Maternal vaccination with two doses of mRNA vaccine was associated with a reduced risk of hospitalization for Covid-19, including for critical illness, among infants younger than 6 months of age.”