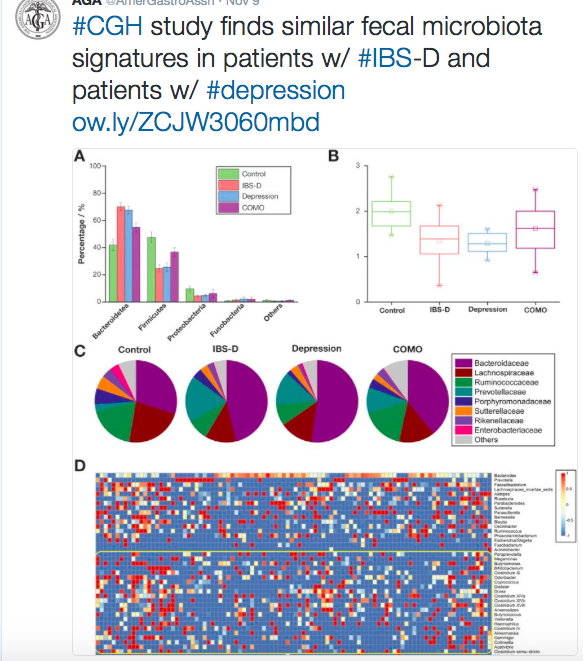
A recent study (Y Liu et al. Clin Gastroenterol Hepatol 2016; 14: 1602-11) showed that fecal microbiota signatures were similar between patients with diarrhea-predominant irritable bowel syndrome (IBS-D) and in patients with depression.
The authors analyzed stool samples from 100 Chinese subjects. In addition to analyzed stool microbiota, the authors evaluated visceral hypersensitivity with a barostat and assessed for mucosal disease with immunohistochemical analyses of sigmoid biopsies.
In both IBS-D patients and patients with depression, the stool diversity was much less than controls and had similar abundance of many alterations, including higher proportions of Bacteroides and Prevotella (see below).
My take: It is interesting to speculate on whether changes in our microbiome could trigger/be related to the pathogenesis of not only IBS-D but other non-GI disorders like depression.
In the screenshot below, the term “COMO” refers to the 25 subjects who had both IBS and depression.