This month’s Gastroenterology issue is devoted solely to the use/expected uses as well as risks of artificial intelligence (AI) for gastroenterology and hepatology.
DL Shung, M Iacucci. Gastroenterol 2025; 169: 391-392. Artificial Intelligence in Gastroenterology and Hepatology: Potential and Perils
An excerpt:
“AI is reshaping the landscape of gastroenterology and hepatology with the promise of better, faster, more objective, and standardized care of delivery. However, behind the algorithms lies a more insidious risk: the erosion of trust in human providers…Information risk …include both error commission (ie, when the models generate false statements, introduce nonsensical concepts, or fabricate sources) and error omission (ie, summaries that omit critical information)…
When AI becomes the center of care, patients may perceive their doctors as intermediaries…diminishing the therapeutic effect of the patient-physician relationship…This arrangement can dilute clinical training, increase physician burnout, and lead to medicolegal implications…Other risks include perpetuating bias from nonrepresentative training data and amplifying uncertainty of AI due to lack of real-world validation…
We hope that AI systems will allow us to spend more, not less, time with patients and empower us to provide personalized care by leveraging high-quality multimodal data.”
Most of the articles are behind a paywall in this issue. There are five that are open access articles:
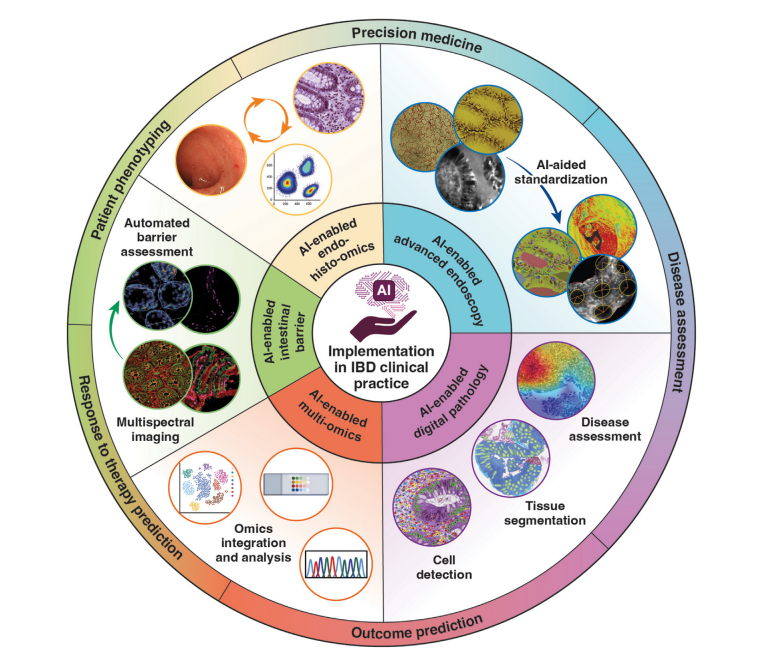
- M Iacucci et al. Gastroenterology 2025;169:416–431. Artificial Intelligence–Driven Personalized Medicine: Transforming Clinical Practice in Inflammatory Bowel Disease
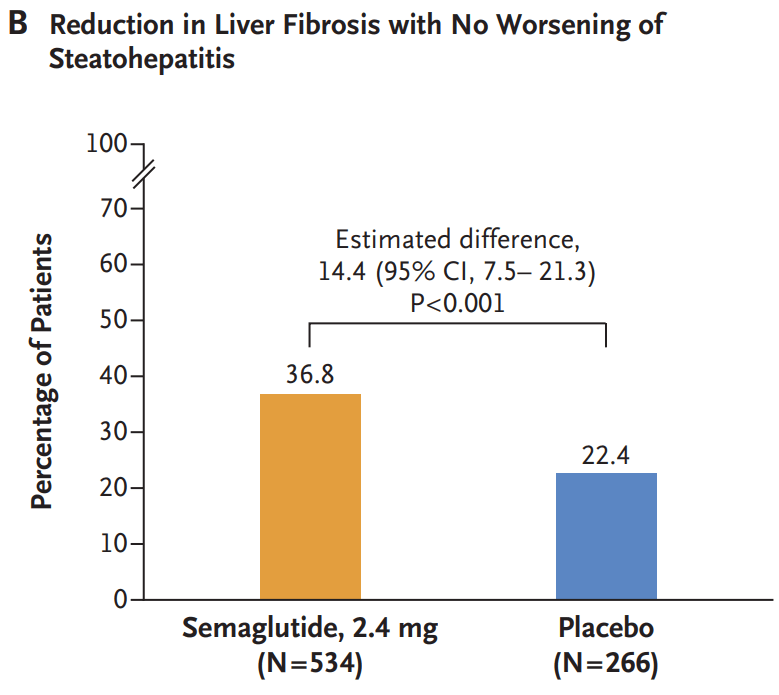
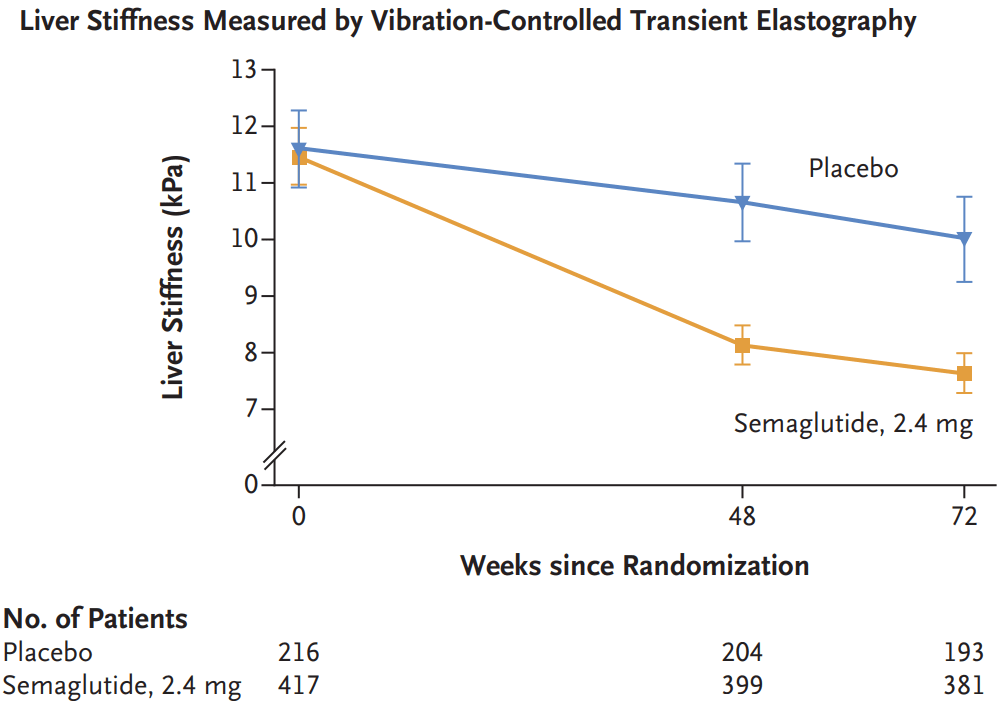
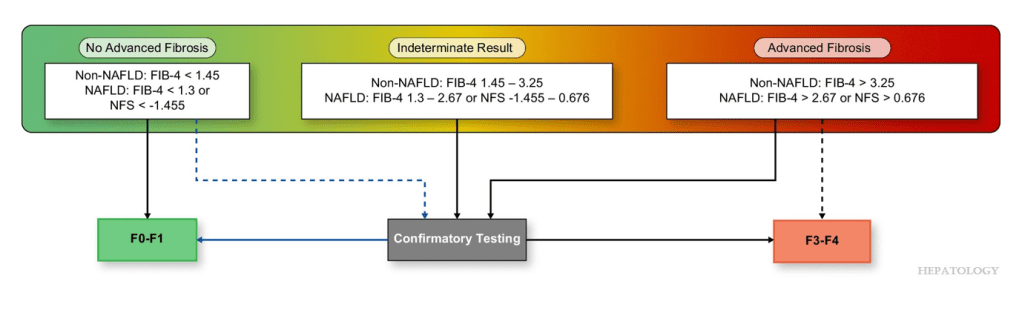
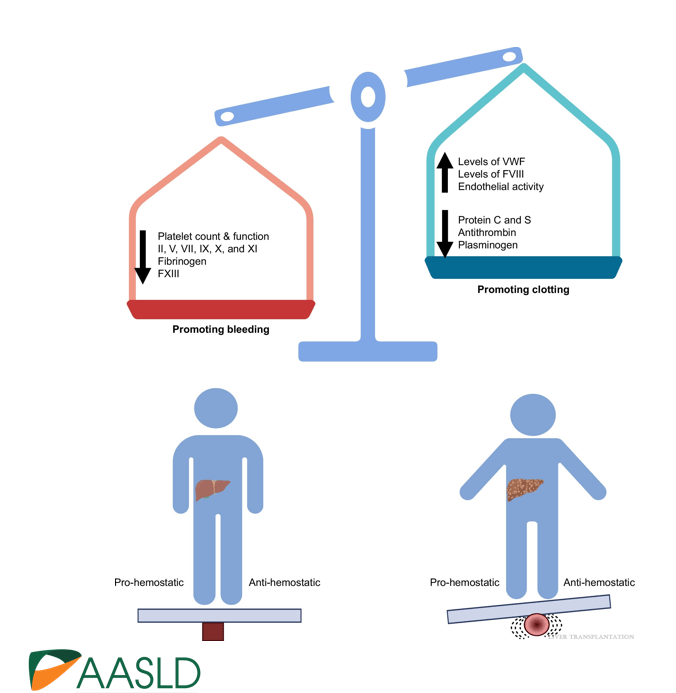
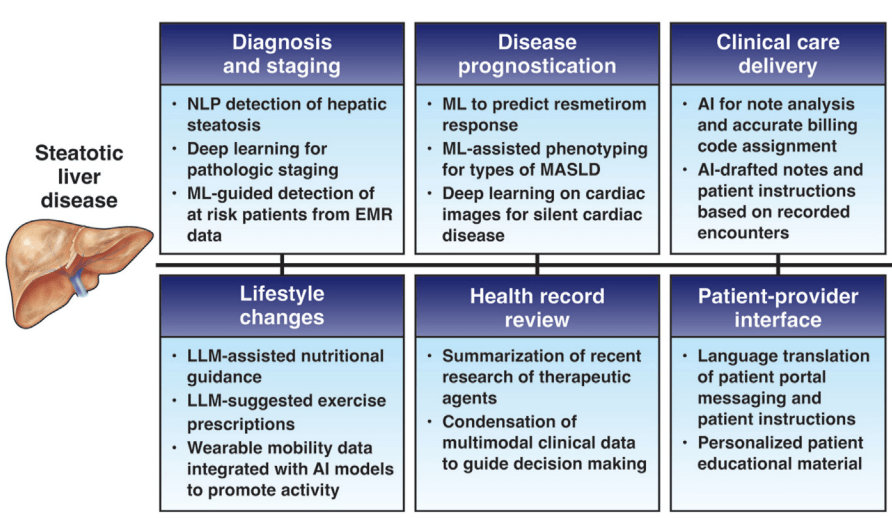
- A Spann et al. Gastroenterology 2025;169:456–470. The Role of Artificial Intelligence in Chronic Liver Diseases and Liver Transplantation

- T Rozera et al. Gastroenterology 2025;169:487–501. Machine Learning and Artificial Intelligence in the Multi-Omics Approach to Gut Microbiota
- A El-Sayed et al. Gastroenterology 2025;169:518–530. Clinical Implementation of Artificial Intelligence in Gastroenterology: Current Landscape, Regulatory Challenges, and Ethical Issues
- MF Byrne et al. Gastroenterology 2025;169:531–544. Synergies Among Clinicians, Academia, and Industry in the Age of Artificial Intelligence
My take: These articles provide a good deal of information about the applications and risks of AI. In my view, physicians will be needed more than ever to help interpret/manage the huge amount of information available.
Related blog posts:
- The Future of Medicine: AI’s Role vs Human Judgment
- Artificial Intelligence in the Endoscopy Suite
- Rising Scientific Fraud: Threats to Research Integrity Plus One
- ChatGPT4 Outperforms GI Docs for Postcolonoscopy Surveillance Advice
- Will Future Pathology Reports Include Likely Therapeutic Recommendations?
- Medical Diagnostic Errors
- Answering Patient Questions: AI Does Better Than Doctors
- Dr. Sana Syed: AI Advancements in Pediatric Gastroenterology