One of the most influential medical articles that I’ve read this year: JR Thiagarajah et al. Gastroenterology 2018; 154: 2045-59. (Senior authors/corresponding authors: Yaron Avitzur and Martin Martin). This article provides an excellent review of the terminology and provides algorithms to help in the evaluation of chronic diarrhea in infants. These algorithms incorporate the role of exome sequencing.
The first part of this review focuses on terminology:
- For those with persistent and severe diarrhea that is not due to an acquired short bowel syndrome (eg. from necrotizing enterocolitis, gastroschisis, or volvulus), the authors use the term congenital diarrhea and enteropathies (CODEs). They suggest using CODEs in place of intractable or protracted diarrhea of infancy.
- Instead of osmotic diarrhea, the authors prefer diet-induced diarrhea since all diarrhea involves osmotic forces. Typically, with this type of diarrhea, stool osmotic gap is >100 mOsm.
- Secretory diarrhea “is also imprecise…We prefer to use the term electrolyte-transport-related diarrhea” (eg. congenital sodium or congenital chloride diarrhea)
Key points:
- Most acquired diarrhea is related to infectious agents and to allergic disorders. Though, persistent diarrhea after an infection could be an early sign of a primary immunodeficiency.
- Stool osmotic gap: = 290 – 2 x (Stool Na + Stool K). Osmotic gap >100 mOsm is high, <50 mOsm is low.
- Stool osmolality in almost all cases is isomolar to serum (~290). If there is suspicion of improper collection or tampering, then this can provide objective evidence of this.
- Reducing substances >0.5% indicates malabsorption of monosaccharides. Low pH (<5.3) is indicative of carbohydrate malabsorption (due to abundance of short-chain fatty acids that are products of fermentation)
- Elastase is “unchanged by intestinal proteases and if low can imply pancreatic insufficiency.” Falsely-low values can occur due to dilution in high-volume diarrhea.
- Alpha-one-antitrypsin is largely resistant to intestinal proteases and elevation indicates excess enteric protein loss (eg. protein-losing enteropathy)
Diagnostic evaluation:
- See figure 1 in review. Initial evaluation after exclusion of acquired diarrheas (eg infection/allergic): History, Blood tests (CBC, CMP, CRP, ESR, IgG, lipid panel), Stool tests (electrolytes, reducing substances, elastase, fecal fat, A1AT, pH, calprotectin/lactoferrin).
- Determining stool output may require a “urine catheter for a few days” for accuracy and help elucidate the effect of fasting on stool output.
- Figure 2 divides evaluation based on type of diarrhea: watery, fatty, and bloody.
- Fatty diarrhea may be due to pancreatic insufficiency, abetalipoproteinemia and chylomicron retention disease. The latter two disorders typically are indicated by fat-laden enterocytes in histologic sections
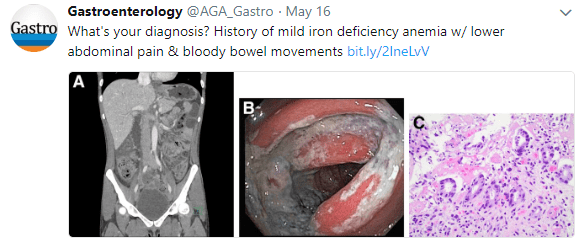
- Bloody diarrhea “should precipitate investigation for very-early-onset inflammatory bowel disease, autoimmune enteropathy, or primary immunodeficiency”
- Watery diarrhea –see tomorrow’s post. Before undergoing extensive evaluation, the authors recommend obtaining an UGI/SBFT to exclude congenital short bowel syndrome.
My take: after initial exclusion of common causes for diarrhea in infancy, early endoscopy is needed along with early use of genetic testing.
Related blog posts:
- Patterns and Puzzles with Very Early Onset Inflammatory Bowel Disease
- “Genetic Testing and the Future of Pediatric Gastroenterology”
- Exome Sequencing in VEO-IBD: More Data
- It’s often elemental
- 10 Years of Intractable Diarrhea
- Diarrhea, GC-C and guanylin
- If I ever see an infant with Congenital Sodium Diarrhea | gutsandgrowth
- Another Rare Cause of Neonatal Diarrhea | gutsandgrowth
Disclaimer: These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition.