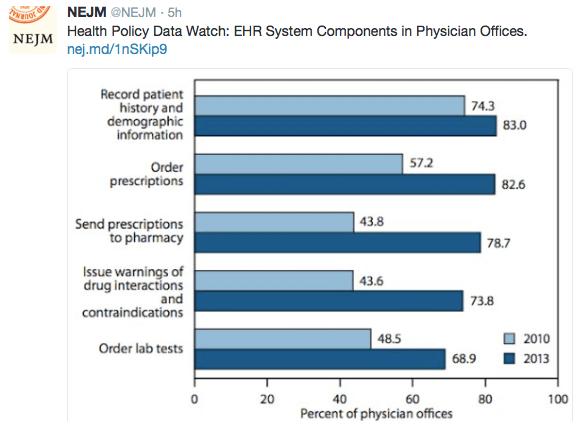
A recent editorial (EW Campion et al. NEJM 2016; 375: 993-4) made a few worthwhile points and shows how NEJM has been successful and innovative over 20 years of using the web and social media.
- This has allowed more widespread access to its content, even by resource-poor countries.
- The use of the web has facilitated quick distribution of multiple resources for outbreaks like Ebola and Zika.
- Currently, every article back to 1812 is available online (over 173,000 with more than 570,000 pages)
- NEJM has 340,000 twitter followers and 1.3 million followers on facebook
- Despite the importance of NEJM, as well as other healthcare media, important caution is needed.
“We do need to be wary of challenges and dangers that the new media have created. On the Internet, speed and simplicity often displace depth and quality, especially on complex subjects. Our privacy is increasingly vulnerable. Misinformation, misrepresentation, and piracy are common. There are health scams and even sham medical conferences and fake medical journals.”
My take: Careful use of internet resources has been incredibly helpful. But, beware of the inherent hazards that have accompanied these advances.
Related blog posts:
- Why I blog | gutsandgrowth
- Why Social Media is Important for Doctors | gutsandgrowth
- Incorporating Social Media into Medicine | gutsandgrowth
- Personal Look at 20 Years of Doctoring (Part 2) | gutsandgrowth