CL Mack et al. JPGN 2019; 68: 495-501. This multicenter prospective open-label phase I/III trial of IVIG in biliary atresia patients status-post Kasai indicated that the infusions were tolerated. However, though this study was not powered to detect efficacy, survival with native liver was LOWER among patients who had received IVIG (n=29): 58.6% compared to the comparison placebo group 70.5% (n=64). Thus, despite the theoretical advantages of IVIG which targets aspects of the immune system and improvement in a murine model, in practice IVIG does not appear promising for biliary atresia.
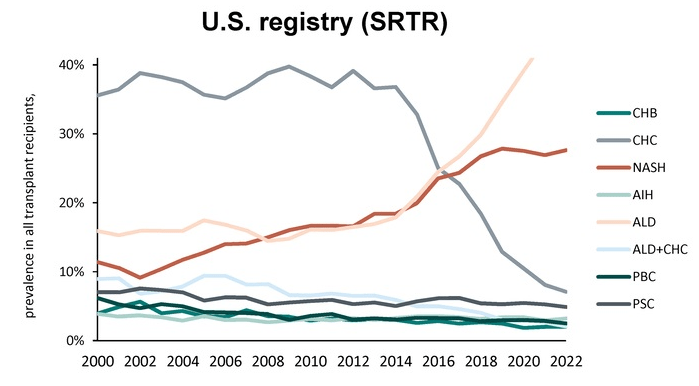
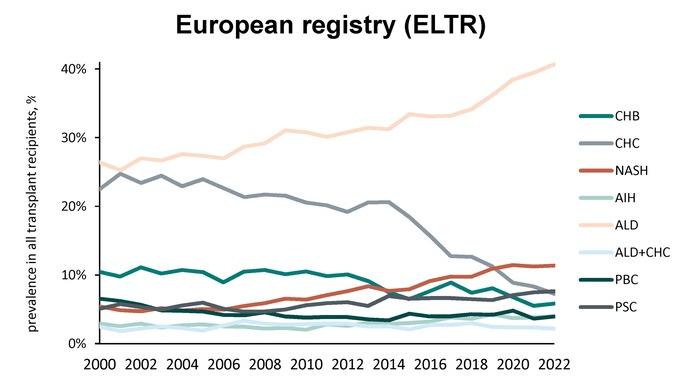
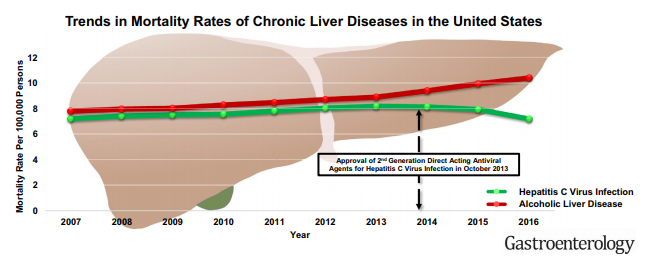
D Kim et al. Hepatology 2019; 69: 1064-74. This study shows that despite improvements in hepatitis C mortality rates associated with newer treatments, there is an overall increase in mortality rates from cirrhosis and hepatocellular carcinoma. This increase is driven by increasing prevalence and severity of both alcoholic liver disease and nonalchoholic fatty liver disease. The overall cirrhosis-related mortality increased from 19.77/100,000 persons in 2007 to 23.67 in 2016 with an annual increase of 2.3%. Similarly, the overall HCC-related mortality increased from 3.48/100,000 persons in 2007 to 4.41 in 2016 at annual increase of 2%. The editorial on page 931 (TG Cotter and MR Charlton) notes that each year there are more than 40,000 deaaths associated with chronic liver disease.
H Park et al. Hepatology 2019; 69: 1032-45. This study, using Truven Health MarketScan Cata, examined the outcomes of more than 26,000 patients with newly-diagnosed hepatitis C virus (HCV) infection. Among the 30% who received oral direct-acting antiviral (DAA) therapy, there were improved outcomes in those with and without cirrhosis. In those with cirrhosis (n=2157), DAA was associated with a 72% and 62% lower incidences of HCC and DCC [decompensated cirrhosis] respectively. In noncirrhotic HCV patients (n=23,948), DAA was associated with a 57% and 58% lower incidence of HCC and DCC respectively. In addition to improved health outcomes, DAA treatment resulted in decrease health care costs, especially for patients with cirrhosis.
Z Kuloglu et al. JPGN 2019; 68: 371-6. In this multicenter Turkish study, the authors identified 810 children (median age 5.6 years) with unexplained transaminase elevation (62%),unexplained organomegaly (45%), obesity-unrelated liver steatosis (26%) and cryptogenic fibrosis or cirrhosis (6%). LAL-D [lysosomal acid lipase deficiency] activity was deficient in 2 siblings (0.2%); both had LDL ~155. Overall, even in at risk groups, LAL-D is rare.
Related posts:

Joshua Tree National Park