Author Archives: gutsandgrowth
AASLD: Advice for Patients with Liver Diseases and Liver Transplants During COVID-19
AASLD: OK Fix et al. Hepatology 2020; 72: 287-304. Full Article Link: Clinical Best Practice Advice for Hepatology and Liver Transplant Providers During the COVID‐19 Pandemic: AASLD Expert Panel Consensus Statement
This is a lengthy article with extensive recommendations –here are a few:
- Consider etiologies unrelated to COVID‐19, including other viruses such as hepatitis A, B and C, when assessing patients with COVID‐19 and elevated liver biochemistries.
- Consider other causes of elevated liver biochemistries, including myositis (particularly when AST>ALT), cardiac injury, ischemia, and cytokine release syndrome.
- Generally, this article supports continuation of ongoing treatments in those with liver disease who are without active infection. “Do not reduce immunosuppression or stop mycophenolate for asymptomatic posttransplant patients without known COVID‐19”
- “As we learn more about how the COVID‐19 pandemic impacts the care of patients with liver disease, we will update the online document available at https://www.aasld.org/about-aasld/covid-19-and-liver.”
Nutrition ‘Mythbuster’ Webinar
A recent Children’s Healthcare Webinar by Hillary Bashaw reviewed several nutrition topics. I took some notes and some screenshots. Some errors of omission and transcription may have occurred.
Key points from talk:
- Cow’s milk overall is a healthy beverage for children, though there are several plant-based alternatives that can be effective substitutes. Soy milk and pea-protein milk are often the best alternatives.
- Fiber from foods is the best way to get fiber. Gummy fiber products are not recommended.
- Eating breakfast likely helps with school performance; however, this does not mean it is the ‘most important’ meal of the day.
Related article: RJ Merritt et al. JPGN 2020; 71: 276–81. Full text link: NASPGHAN Position Paper: Plant-based Milks
- One of the slides from this talk modifies the Table 1 (adds skim milk) from this article.
- “Milk‘s contribution to the protein intake of young children is especially important. For almond or rice milk, an 8 oz serving provides only about 2% or 8%, respectively, of the protein equivalent found in a serving of CM.”
- “As presently constituted, almond, rice, coconut, hemp, flax seed, and cashew “milks” are inappropriate replacements for CM in toddlers and young children for whom milk remains an important part of the diet.”
Milk–related blog posts:
- It’s Complicated: The Relationship Between Milk and Health
- Is Drinking Milk Healthy?
- The Genius of Breastmilk | gutsandgrowth
- Overdiagnosis of Cow’s Milk Protein Allergy in Infants and Formula Industry Influence
- Pediatric Osteoporosis and Bone Health -Lecture Slides with commentary
Fiber:
Fiber–related blog posts:
- Why Fiber Matters?
- It’s Alimentary! Part 1
- Why Fiber (Fruits and Veggies) Is Good For You
- Eat your veggies…if you do not want to get sick
Breakfast:
Breakfast-related blog posts:
Trichobezoar: Don’t Do What They Did
A recent review and case report (AF Nita et al JPGN 2020; 71: 163-70) describe an anguishing outcome after an endoscopy. This publication is a useful, cautionary tale. In my view, the associated editorial (“MacGyver and Rapunzel in the Pediatric Endoscopy Suite” by JR Lightdale, pg 147-8) tiptoes on the issue of safety concerns of the endoscopic approach described in the review.
Case report: The authors describe a 9 year old with trichobezoar/Rapunzel syndrome who underwent a 3 hour endoscopic procedure with APC to remove the trichobezoar which was found to be composed of both human hair and doll’s hair (the latter may have contributed to complications). In addition, the child had undiagnosed celiac disease. Subsequent to the procedure, the child required a laparotomy; she had 18 small intestinal perforations and a gastric perforation. The child went on to need an extensive small bowel resection (107 cm) and a 3 month hospitalization.
The authors state that a previous review had indicated only a 5% success rate for trichobezoar endoscopic removal (RR Gorter et al. Pediatr Surg Int 2010; 26: 457-63). However, they claim increased success more recently by identifying 16 of 52 (30.7%) removal rate from recent case reports. Interestingly, one of the successful endoscopic removals cited by the authors had a respiratory arrest during the procedure (Esmali et al).
Bad advice from this article:
- #1 The authors repeatedly suggest now that there is a >30% endoscopic success rate for endoscopic removal and thus they suggest that “it remains reasonable to attempt endoscopic retrieval” as long as a gastric trichobezoar occupies less than two-thirds of the stomach and has limited to no extension into the small bowel.
- #2 The authors believe that “the skill mix of the endoscopist” is an important issue.
My take on their ‘learning points’:
- This 30% success rate should not be taken seriously due to publication bias (many unsuccessful cases are not reported) and due to treatment bias. Many clinicians would never attempt to remove a very large trichobezoar. Thus, the 30% success rate likely includes bezoars that may be more amenable to removal and by centers with more advanced endoscopists.
- The second claim about endoscopist skill is also bad advice. First of all, some of the authors of this study have extensive endoscopic experience and yet this did not preclude a bad outcome for this child. Secondly, in my experience, ~85% of individuals (including GI doctors) consider themselves above average; thus, it may be difficult to know if the ‘skill mix’ of the endoscopist is suitable. Large trichobezoars are rare and no individuals will have enough experience to be considered experts.
- My advice: Don’t try to be MacGyver in the endoscopy suite. Most trichobezoar cases are more suitable for surgical removal. The most important skill of a good endoscopist is good judgement and the ability to identify cases in which an endoscopy is ill-advised.
MIT Technology Review: How to Talk to Conspiracy Theorists
From Bryan Vartabedian’s 33email –this link: MIT Technology Review: How to Talk to Conspiracy Theorists
An excerpt:
- Always, always speak respectfully. Every single person I spoke to said that without respect, compassion, and empathy, no one will open their mind or heart to you. No one will listen.
- Go private…
- Test the waters first. That way you save yourself time and energy. “You can ask what it would take to change their mind, and if they say they will never change their mind, then you should take them at their word and not bother engaging,”
- Agree…[with some parts] Conspiracy theories often feature elements that everyone can agree on
- Try the “truth sandwich. Use the fact-fallacy-fact approach…
- Or use the Socratic method. In other words, use questions to help others probe their own argument and see if it stands up. ..The best way to change someone’s view is to make them feel like they’ve uncovered it themselves,” he says. That means engaging in back-and-forth questions and answers until you hit a dead end, gently pointing out inconsistencies.
- Be very careful with loved ones.
- Realize that some people don’t want to change, no matter the facts.
- If it gets bad, stop. … “If I am not enjoying the discussion and getting angry, then I simply stop.”
- Every little bit helps. One conversation will probably not change a person’s mind, and that’s okay
Related blog posts:
- @AllergyKidsDoc: Deep Down the Rabbit Hole ob Bias
- “The Truth About Allergies and Food Sensitivity Tests”
- War on Science and Genetically-Modified Foods
- Alan Alda (aka Hawkeye Pierce) on Communicating Science …
- NPR: “Should You Trust That New Medical Study?” | gutsandgrowth
- Why I have always liked Arthur Caplan… | gutsandgrowth
- How to Understand Scientific Studies | gutsandgrowth
- Short Take on Understanding Bias | gutsandgrowth
Comparative Efficacy: Vedolizumab vs Anti-TNF Agents
M Bohm et al. AP&T: 2020; July 2020 https://doi.org/10.1111/apt.15921 Full text: Comparative safety and effectiveness of vedolizumab to tumour necrosis factor antagonist therapy for Crohn’s disease
Thanks to Ben Gold for this reference.
Methods: Retrospective observational cohort (May 2014–December 2017) propensity score‐weighted comparison of vedolizumab vs TNF‐antagonist therapy (infliximab, adalimumab, certolizumab) in CD. This study included 1266 patients (n = 659 vedolizumab).
Key findings:
- Rates of non‐infectious serious adverse events (odds ratio [OR] 0.072, 95% confidence interval [CI] 0.012‐0.242) were significantly lower with vedolizumab vs TNF‐antagonist therapy.
- These events included severe arthralgias in 3 vedolizumab-treated patients. For anti-TNF recipients, events included hypersensitivity or infusion reactions (n = 6), drug‐induced psoriasis (n = 6), drug‐induced lupus (n = 5), severe liver function test abnormalities (n = 3), skin rash (n = 2), lung cancer (n = 1) and jaw or hip necrosis (n = 2).
- Rates of serious infections (OR 1.183, 95% CI 0.786‐1.795), were NOT significantly lower with vedolizumab vs TNF‐antagonist therapy.
- “The risk of serious infections with biologic therapy is largely driven by disease activity and concomitant use of immunosuppressive agents…. the higher concomitant use of steroids among the vedolizumab‐treated patients in our cohort may therefore help to explain the lack of observed difference in risk for serious infections between agents.”
- No significant difference was observed between vedolizumab and TNF‐antagonist therapy for clinical remission (hazard ratio [HR] 0.932, 95% CI 0.707‐1.228), steroid‐free clinical remission (HR 1.250, 95% CI 0.677‐2.310) or endoscopic remission (HR 0.827, 95% CI 0.595‐1.151).
- “Our observational cohort study was not designed to be a noninferiority study, and the safety and effectiveness comparisons were exploratory in nature.”
- The efficacy of vedolizumab in this study is more impressive given that 91% of the patients had prior anti-TNF therapy.
- “Exploratory subgroup analyses suggested that vedolizumab might be superior to subcutaneous TNF‐antagonist therapy for the achievement of clinical remission and steroid‐free clinical remission in TNF‐antagonist–naïve patients.”
- TNF‐antagonist therapy was associated with higher treatment persistence compared with vedolizumab.
My take: This article shows that clinical experience with vedolizumab is quite good and compares favorably with anti-TNF agents. Randomized head-to-head studies are needed, though, to truly determine efficacy in similar populations.
Related blog posts:
- Expert Guidance on Current IBD Mgt (2020)
- Real-World Vedolizumab: Better Than Expected
- Predicting Response to Vedolizumab and Ustekinumab for Inflammatory Bowel Disease
- Ustekinumab Over Vedolizumab for Crohn’s Disease as a 2nd Line Agent for Crohn’s disease
- IBD Highlights from Recent Meetings with Commentary by Dr. Sandborn Explains Why Vedolizumab Should Be Considered a First Line Agent (2019)
- VICTORY Consortium Data for Vedolizumab 2018
- Vedolizumab More Effective Than Adalimumab for Ulcerative Colitis (Part 2)
- Vedolizumab More Effective Than Adalimumab for Ulcerative Colitis
- Vedolizumab vs Adalimumab for Infliximab Failure in Ulcerative Colitis –Which is Better?
- Getting the Most Out of Vedolizumab
- Enthusiasm for Vedolizumab
- Expert Guidance on Inflammatory Bowel Disease (Part 3)
- Expert Guidance on Inflammatory Bowel Disease (Part 2)
COVID-19: At-Risk Populations, Moral Distress, and Related News
Before today’s post –more on voting this year:
Democracy Docket Four Ways to Safely Cast Your Ballot without USPS
- This article also has very helpful links to all of the states’ resources, regulations, and contacts
Several recent commentaries have shown scenarios impacted by this pandemic. Thanks to Ben Gold for sharing these references.
CA Wong et al. Pediatrics, : Mitigating the Impacts of the COVID-19 Pandemic Response on At-Risk Children
Here, we (1) highlight the health risks of the pandemic response measures to vulnerable pediatric subpopulations and (2) propose risk mitigation strategies that can be enacted by policy makers, health care providers and systems, and communities.
- Children With Behavioral Health Needs
- Children in Foster Care or at Risk for Maltreatment
- Children With Medical Complexity
R Cholera et al. Pediatrics. Full link: Sheltering in Place in a Xenophobic Climate: COVID-19 and Children in Immigrant Families
One in 4 children (>18 million) in the United States lives in an immigrant family, in which the child or ≥1 parent was born outside the United States.1 Among children in immigrant families (CIF), >7 million live in “mixed-status” families, meaning ≥1 parent is not a US citizen.2… The COVID-19 pandemic amplifies existing inequities and introduces new ones as immigrant families navigate school closures, lack of health insurance and paid leave, and decisions to seek medical care or public services amid ongoing immigration enforcement. Additionally, immigrant families are more likely to live in multigenerational households,4 heightening the risk of COVID-19 for multiple family members…For CIF in US communities coping with persistent fears of immigration enforcement and family separation, economic devastation during a pandemic may threaten the stability of place. In this article, we apply a health equity framework5 to evaluate the impact of COVID-19 on CIF and highlight opportunities for advocacy and action for pediatricians, hospitals and health care systems, and policymakers to mitigate the unique risks faced by CIF
AM Evans et al. Pediatrics: Pediatric Palliative Care in a Pandemic: Role Obligations, Moral Distress, and the Care You Can Give
Moral distress refers to the experience of being unable to take the action that one believes to be morally right or required.1… the inability to provide care because of resource constraints, involvement in care that one deems to be against a patient’s interests, and disputes about care planning with families and within teams…
We cannot have an obligation to save a life that cannot be saved: we can only be obliged to do what we can… It is only your role to act well within your scope of responsibility and to be the best clinician that you can be under the circumstances. Recognizing the limits of one’s powers can relieve a burden of guilt that is unconnected with one’s own choices and actions.
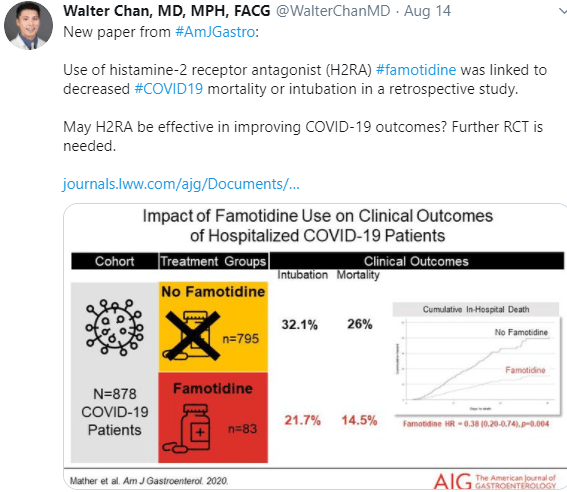
Famotidine may be helpful based on a retrospective study:
This long piece from Slate details the myriad public health mistakes in the U.S. approach to COVID-19: The Trump Pandemic
Screenshots and Tweets; MCAT Exposures, Uninsured in Texas, Health Inequalities, a Joke, Other News
Good Reads:
- Wired: Bill Gates on Covid: Most US Tests Are ‘Completely Garbage’
- MMWR: Hospitalization Rates and Characteristics of Children Aged <18 Years Hospitalized with Laboratory-Confirmed COVID-19 — COVID-NET, 14 States, March 1–July 25, 2020 “Analysis of pediatric COVID-19 hospitalization data from 14 states found that although the cumulative rate of COVID-19–associated hospitalization among children (8.0 per 100,000 population) is low compared with that in adults (164.5), one in three hospitalized children was admitted to an intensive care unit…Among 222 (38.5%) of 576 children with information on underlying medical conditions, 94 (42.3%) had one or more underlying conditions . The most prevalent conditions included obesity (37.8%), chronic lung disease (18.0%), and prematurity (gestational age <37 weeks at birth, collected only for children aged <2 years) (15.4%)end highlight.” Key finding: Using a multisite, geographically diverse network, this report found that children with SARS-CoV-2 infection can have severe illness requiring hospitalization and intensive care.
COVID-19 Physician’s Personal Experience
Link: MY COVID-19 Excerpts:
The Downside of Home Infusion of Biologics
N Giese-Kim et al. Am J Gastroenterol: July 22, 2020 – Volume Publish Ahead of Print – Issue – doi: 10.14309/ajg.0000000000000750. Link to abstract: Home Infliximab Infusions Are Associated With Suboptimal Outcomes Without Cost Savings in Inflammatory Bowel Diseases
In this study, there were 27,396 patients with IBD (1,839 pediatric patients). Overall, 5.7% of patients used home infliximab infusions.
Results:
- Those with home infusions:
- more likely to be nonadherent compared with both office-based (22.2% vs 19.8%; P = .044) and hospital-based infusions (22.2% vs 21.2%; P < .001).
- more likely to discontinue infliximab compared with office-based (44.7% vs 33.7%; P < .001) or hospital-based (44.7% vs 33.4%; P < .001) infusions.
- On Kaplan-Meier analysis, the probabilities of remaining on infliximab by day 200 of therapy were 64.4%, 74.2%, and 79.3% for home-, hospital-, and office-based infusions, respectively (P < .001)
- Home infusions did not decrease overall annual care costs compared with office infusions ($49,149 vs $43,466, P < .001)
My take: In my experience, office-based infusions can be provided safely and in a cost-effective manner. From the authors: “home infliximab infusions for patients with IBD were associated with suboptimal outcomes including higher rates of nonadherence and discontinuation of infliximab. Home infusions did not result in significant cost savings compared with office infusions.”
Related blog posts:
- How Do Home Infusions Stack Up?
- Pediatric Home and Office Biologic Infusions -What is Needed
- Infliximab infusions without premedication
- My first take: It is hard to save money at a Rolls Royce Dealership
- Orphan Drugs –Very Profitable (Humira is labelled an orphan drug!)
- NY Times: Humira’s Best-Selling Drug Formula: Start at a High Price. Go Higher.
Drug Therapy for Celiac Disease: Case Report
Briefly noted: L Waters et al. Annals Int Med 2020; doi:10.7326/L20-0497. Celiac Disease Remission With Tofacitinib
The authors describe a male with a well-documented case of celiac disease and alopecia areata. He was placed on tofacitinib off-label for his alopecia areata and it was discovered that his celiac disease had developed “complete histologic and serologic remission…while he was still on a gluten-containing diet.” Prior to medication, he had confirmation of both severe histologic changes and high tTG IgA titers.
The authors note that tofacitinib inhibits CD8+ T-cell mediated enteropathy in a transgenic mouse model.
My take (borrowed from authors): Tofacitinib has many potential adverse effects but may considered for further study, especially in refractory celiac disease.
_______________________________________