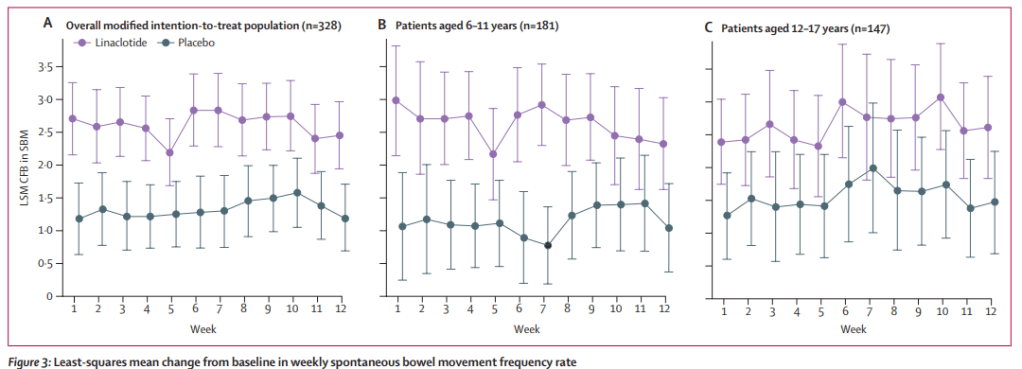
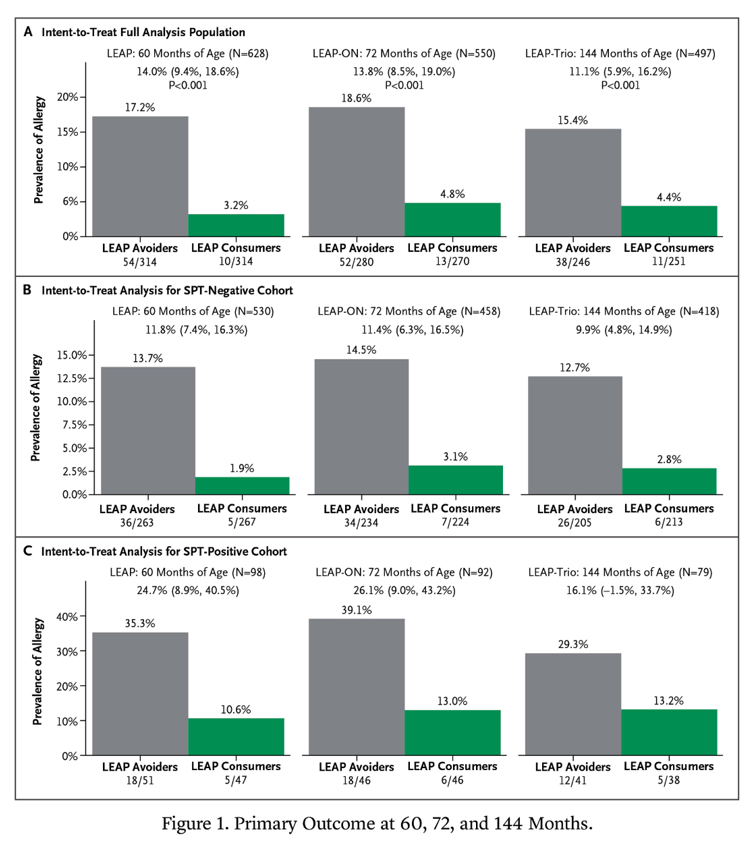
BE Lacy et al. Gastroenterology & Hepatology 2024; 20: 264-272. Open Access! Leaky Gut Syndrome: Myths and Management
Background: “Leaky gut syndrome is a recent diagnosis now popularized in the lay literature. It has been associated with a myriad of disorders (eg, Alzheimer disease, autism, dementia, diabetes, fibromyalgia),5-8…Despite lay literature claims of gut permeability’s pathologic nature, it is important to understand that all individuals are subject to a baseline level of intestinal permeability, as normal intestinal physiology involves selectively permeable tight junctions that respond to a variety of biological factors…Minimal to no reliable evidence exists to suggest that leaky gut syndrome maintains a causative role in the pathogenesis of conditions that are most commonly associated with it in lay discussion, including fibromyalgia, chronic fatigue syndrome, allergies, headache, and brain fog.11,19 “
Key Points:
- Myth: Leaky Gut Syndrome Is Common and Causes Extraintestinal Symptoms
- Myth: Leaky Gut Syndrome Develops Owing to Stress and Eating Gluten – “a variety of factors may influence intestinal permeability, including illness, antibiotic and drug use, alcohol consumption, and physical activity.1,21-24“
- Myth: Leaky Gut Syndrome Is Just a Break in the Gut Lining
- Myth: Leaky Gut Syndrome Can Be Confidently Diagnosed by Symptoms Alone -“reported symptoms typically include bloating, abdominal pain, fatigue, headache, and food sensitivities, among dozens of other symptoms.1,9 Such symptoms are nonspecific in nature”
- Myth: Leaky Gut Syndrome Can Be Readily Diagnosed by Blood Work and Standard Endoscopy -“Although available, the clinical utility of using orally ingested saccharide probes and in vitro techniques is limited partly owing to unknown normal values for comparison, lack of standardized protocols, and limited attempts at validation.47…As noted previously, confocal laser endomicroscopy may provide valuable information on intestinal permeability, although it may not be as sensitive as once thought for the evaluation of food sensitivities.45 For now, no validated tool exists to accurately diagnose leaky gut syndrome.39…The utility of measuring zonulin in over-the-counter kits is thus suspect. Other plasma biomarkers measuring bacterial translocation, such as lipopolysaccharide-binding protein, may correlate more reliably with intestinal permeability.52 Currently, no blood test to diagnose leaky gut syndrome exists, and further investigation is needed to identify valid, reliable, and clinically useful serum biomarkers of impaired intestinal barrier function.”
- Myth: Leaky Gut Syndrome Can Be Diagnosed by Stool Studies -“stool testing for leaky gut syndrome has been marketed to consumers…such tests are unregulated, and minimal evidence exists to support their use in the clinical setting… Even if testing were to reliably measure intestinal permeability, results would be of unclear significance, as no standard of care currently exists for treating and managing leaky gut syndrome. “
- Myth: Leaky Gut Syndrome Can Be Cured by Diet and Probiotics -“a direct link between diet and treatment of leaky gut syndrome has not been established.”
- Myth: Nutritional Supplements Can Cure Leaky Gut Syndrome -“although several nutritional supplements have been suggested to improve intestinal permeability, only glutamine has been shown to improve leaky gut syndrome in the context of IBD and IBS. More data are needed before any nutritional supplements, including glutamine, can be recommended in clinical practice”
- Myth: Medications Cannot Change Intestinal Permeability -“Several medications can alter intestinal permeability.” Examples include lubiprostone (for IBS), and prednisone and infliximab (for IBD).
- Myth: Once Leaky Gut Syndrome Develops, It Will Never Go Away -“no study has been performed to properly evaluate changes in symptoms and underlying pathophysiology over time.”
Overall: A leaky gut “cannot be accurately diagnosed by symptoms, blood work, or stool studies. Although the term leaky gut syndrome implies changes in intestinal permeability, it is the rare patient who undergoes objective testing to identify changes in intestinal permeability…changes in intestinal permeability are not always deleterious, and the relationship with symptoms is unclear.”
My take: It is not unusual for me to take a deep breath and sigh when I see that I am about to see a patient with a chief complaint of a “leaky gut.” Typically, this visit will mean a lengthy discussion indicating that previous testing was not worthwhile and there are no specific treatments. Many times this discussion is not well-received.
Related blog post: Is Intestinal Function in Children with Autism Different?