LE Irastorza et al. JPGN 2022; 74: 267-271. Eosinophil-Derived Neurotoxin Predicts Response to Proton-Pump Inhibitor Treatment in Pediatric Eosinophilic Esophagitis
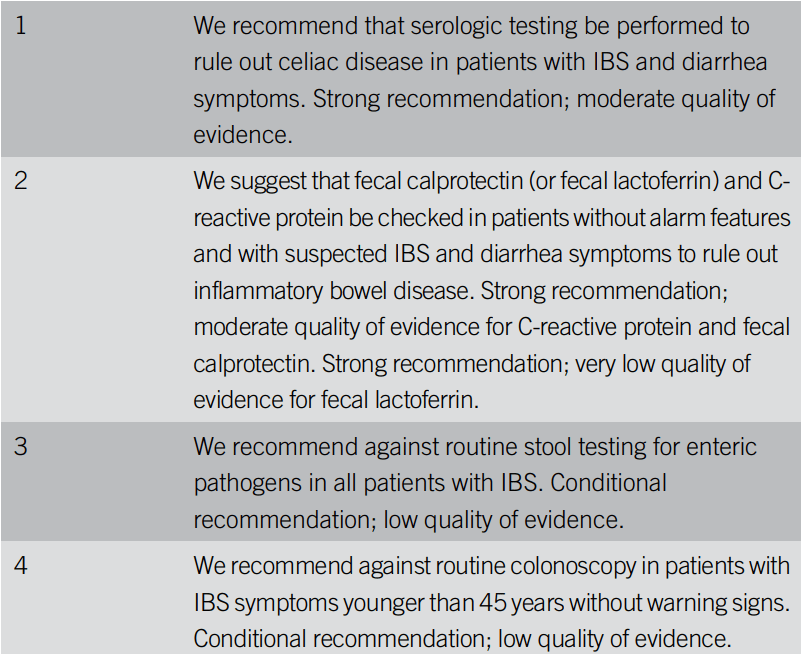
In this prospective study, the authors compared Eosinophil-Derived Neurotoxin (EDN) levels in pediatric patients with eosinophilic esophagitis (EoE) who responded PPIs (n=15) to those who did not respond to PPIs (n=21). The publication states that EDN levels of 10 mcg/mL or greater are diagnostic for EoE (sensitivity 97%, specificity 89%) but EDN levels have not previously been studied as a marker for PPI responsiveness.
Key finding: EDN concentration was significantly higher in the PPI-nonresponsive group than in the PPI-responsive group (219.1 ± 229 mcg/mL vs 75.7 ± 60 mcg/mL, respectively, P = 0.036).
However, Figures 1 (see below) and 2 show that EDN levels while generally higher in those who did not respond to PPIs are not likely to help much at all in predicting who will respond to PPIs, mainly due to a lot of overlap in the levels. While very elevated levels (above ~300 mcg/mL) all occurred in PPI non-responders, this only accounted for 5 patients out of 36 in the entire cohort.
My take: This article’s title is quite misleading. EDN levels are generally higher in PPI-nonresponders but they do not predict response.
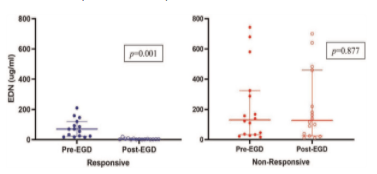
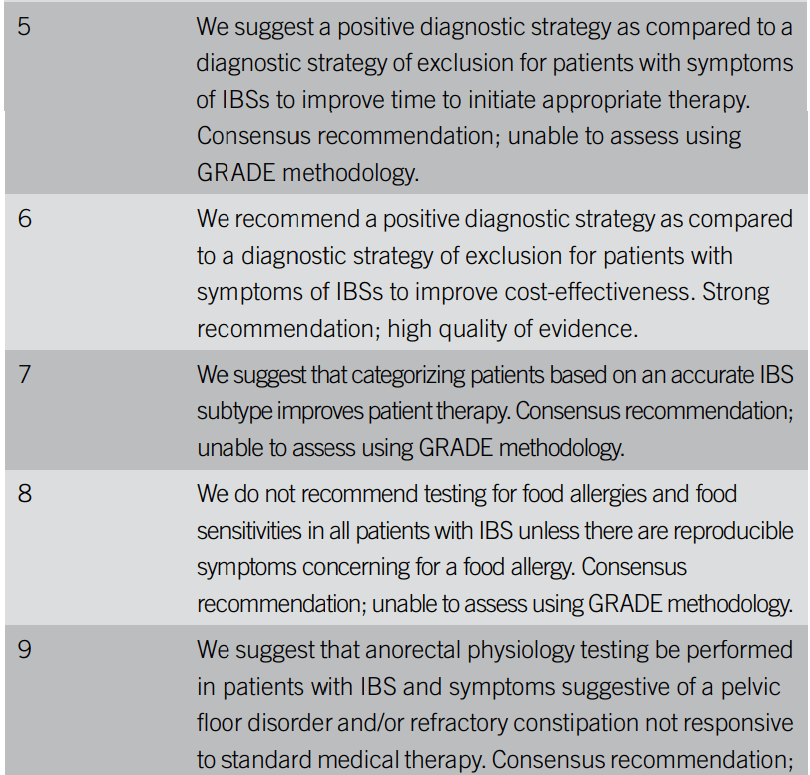
Figure 1
AA Wenzel et al. JPGN 2022; 74: e31-e34. Continued Basal Zone Expansion After Resolution of Eosinophilia in a Child With Eosinophilic Esophagitis on Benralizumab
This case report examined the effect of benralizumab, a monoclonal antibody against the interleukin-5 receptor (IL5Rα) on eosinophils in 20 year old with asthma and EoE. Histology was notable for resolution of esophageal eosinophilia but demonstrated marked basal zone hyperplasia (BZH) in association with high numbers of CD3+ T cells and tryptase+ mast cells. Subsequently, she improved with the institution of dupilumab with resolution of BZH and mast cell inflammation with significant reduction in T cells.
My take: Even with resolution of eosinophilia, mast cells and T cells appear to be capable of coordinating mucosal inflammation and symptoms of EoE (at least in some patients). This study mirrors my limited experience, in which patients receiving benralizumab had a grossly abnormal-appearing esophagus but resolution of the eosinophils.
Related blog posts: