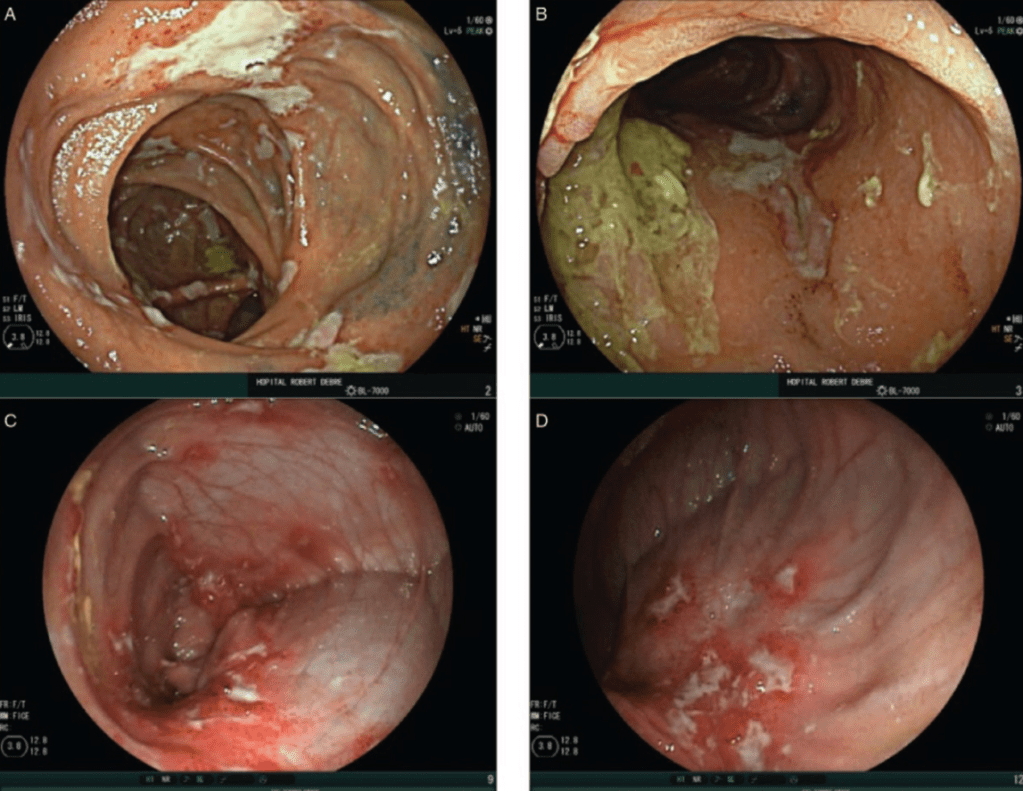
L Peyrin-Biroulet et al. Gastroenterol 2021; Open Access DOI:https://doi.org/10.1053/j.gastro.2021.06.015. Histologic Outcomes With Vedolizumab Versus Adalimumab in Ulcerative Colitis: Results From An Efficacy and Safety Study of Vedolizumab Intravenous Compared to Adalimumab Subcutaneous in Participants With Ulcerative Colitis (VARSITY)
In total, 769 patients received vedolizumab (n = 383) or adalimumab (n = 386). Geboes Index and Robarts Histopathology Index (RHI) scores were used to assess prespecified histologic exploratory end points of histologic remission (Geboes <2 or RHI ≤2) and minimal histologic disease activity (Geboes ≤3.1 or RHI ≤4) at weeks 14 and 52.
Key findings:
Vedolizumab induced greater histologic remission than adalimumab:
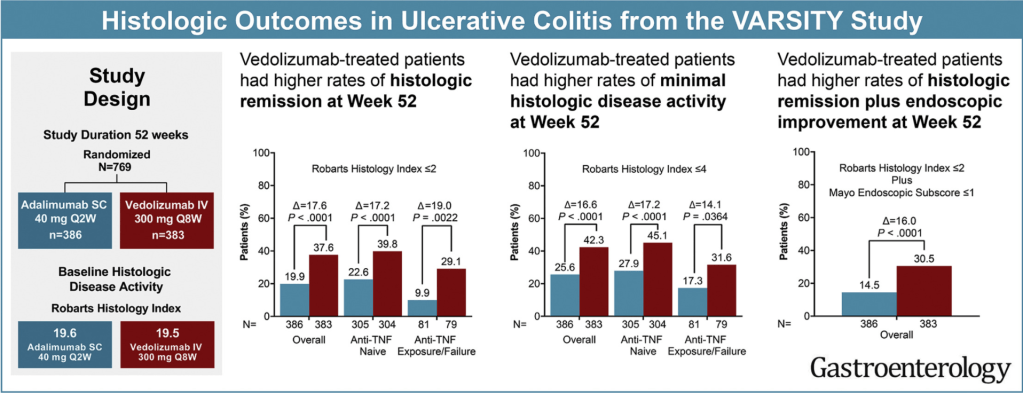
- week 14: Geboes: 16.7% vs 7.3%, RHI: 25.6% vs 16.1%
- week 52: Geboes: 29.2% vs 8.3%, RHI: 37.6% vs 19.9%
- Histologic outcomes were generally better in anti–TNF-naïve vs -failure patients
My take: This study shows that histologic outcomes with vedolizumab, similar to clinical outcomes, were better than with adalimumab. Some of this difference could be due to the trail design which did not allow optimization of adalimumab dosing.
Related posts:
- Vedolizumab versus Adalimumab for Ulcerative Colitis (part 2)
- Vedolizumab More Effective Than Adalimumab for Ulcerative Colitis
- Real-World Vedolizumab: Better Than Expected | gutsandgrowth
- Comparative Efficacy: Vedolizumab vs Anti-TNF Agents | gutsandgrowth
- Vedolizumab vs. Adalimumab for Infliximab Failure in Ulcerative Colitis: Which is better?