From Nate Silver:



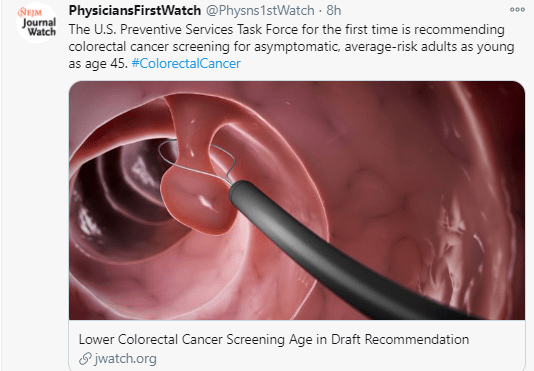
Aubrey Gordon provides personal insight into the issue of weight stigma in her opinion piece: NY Times Leave Overweight Kids Alone
Here a few excepts:
The war on childhood obesity reached its zenith with the 2010 introduction of the national “Let’s Move!” campaign, “dedicated to solving the problem of obesity within a generation.” It was a campaign against “childhood obesity” — not specific health conditions or the behaviors that may contribute to those health conditions. It wasn’t a campaign against foods with little nutritional value, or against the unchecked poverty that called for such low-cost, shelf-stable foods. It was a campaign against a body type — specifically, children’s body types.
In 2012, Georgia began its Strong4Life campaign aimed at reducing children’s weight and lowering the state’s national ranking: second in childhood obesity. Run by the pediatric hospital Children’s Healthcare of Atlanta, it was inspired in part by a previous anti-meth campaign. Now, instead of targeting addiction in adults, the billboards targeted fatness in children…The billboards purported to warn parents of the danger of childhood fatness, but to many they appeared to be public ridicule of fat kids…
Despite ample federal and state funding, multiple national public health campaigns and a slew of television shows, the war on obesity does not appear to be lowering Americans’ B.M.I.s. According to the Centers for Disease Control and Prevention, since 1999 there has been a 39 percent increase in adult obesity and a 33.1 percent increase in obesity among children.
Weight stigma kick-starts what for many will become lifelong cycles of shame..Yet, despite its demonstrated ineffectiveness, the so-called war on childhood obesity rages on. This holiday season, for the sake of children who are told You’re not beautiful. You’re indulging too much. Your body is wrong. You must have done it, I hope some parents will declare a cease-fire.
Related blog posts:

Related blog posts:
DK Mullady et al. Gastroenterol 2020; 159: 1120-1128. AGA Clinical Practice Update on Endoscopic Therapies for Non-Variceal Upper Gastrointestinal Bleeding: Expert Review
Listed below are the 10 ‘Best Practice Advice’ recommendations. I think the acknowledgement that “hemostatic powder should be preferentially used as a rescue therapy and not for primary hemostasis, except in cases of malignant bleeding or massive bleeding with inability to perform thermal therapy or hemoclip placement” (#7) is very useful.
Related blog posts:
M Slaoui, M Hepburn. NEJM 2020; 383: 1701-1703. Full text: Developing Safe and Effective Covid Vaccines — Operation Warp Speed’s Strategy and Approach
As an aside, I have always thought that the name, “Operation Warp Speed,” sounded like a line from the movie Spaceballs.
This article provides insight into the strategy for “Operation Warp Speed” (OWS). An excerpt:
OWS’s strategy relies on a few key principles. First, we sought to build a diverse project portfolio that includes two vaccine candidates based on each of the four platform technologies…In addition, advancing eight vaccines in parallel will increase the chances of delivering 300 million doses in the first half of 2021…
Of the eight vaccines in OWS’s portfolio, six have been announced and partnerships executed with the companies: Moderna and Pfizer/BioNTech (both mRNA), AstraZeneca and Janssen (both replication-defective live-vector), and Novavax and Sanofi/GSK (both recombinant-subunit-adjuvanted protein). These candidates cover three of the four platform technologies and are currently in clinical trials. The remaining two candidates will enter trials soon...
No scientific enterprise could guarantee success by January 2021, but the strategic decisions and choices we’ve made, the support the government has provided, and the accomplishments to date make us optimistic that we will succeed in this unprecedented endeavor.
Related article:
NY Times (11/9/20): Pfizer’s Early Data Shows Vaccine Is More Than 90% Effective

Healio Gastroenterology: Kiwi fruit effective, well tolerated in treating chronic constipation
From a randomized (Virtual) ACG 2020 study from Samuel W. Chey and colleagues (University of Michigan), n=79 adults:


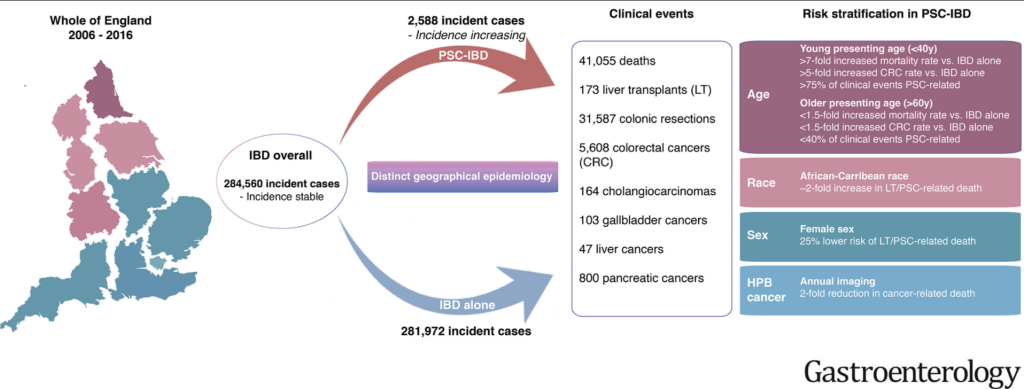
PJ Trivedi et al. Gastroenterol 2020; 159: 915-928. Effects of Primary Sclerosing Cholangitis on Risks of Cancer and Death in People With Inflammatory Bowel Disease, Based on Sex, Race, and Age
Methods: The authors linked prospectively collected data from national health care registries maintained for all adults in England on hospital attendances, imaging and endoscopic evaluations, surgical procedures, cancer, and deaths.
Key findings:
My take: This study shows the impact the added diagnosis of PSC has for patients with IBD. One of the limitations in assessing outcomes is determining whether someone with IBD has PSC as there are a lot of patients with IBD who have asymptomatic changes in their biliary tree.
Related blog posts:
HB Murray et al. Clin Gastroenterol Hepatol 2020; 18: 2471-2478. Frequency of Eating Disorder Pathology Among Patients With Chronic Constipation and Contribution of Gastrointestinal-Specific Anxiety
Key findings:
The authors note that screening for eating disorders “is of particular importance before prescribing dietary interventions.”
My take: While this was a study with adults, it is likely that chronic constipation may be a presenting feature of an eating disorder in teenagers as well.

JM Scheiman et al. Annals of Internal Medicine. 2020; https://doi.org/10.7326/M20-2928. Surprise Billing for Colonoscopy: The Scope of the Problem
Background: “Federal law eliminates consumer cost sharing for multiple methods of colorectal cancer screening, including colonoscopy when done by an in-network provider. However, some patients having screening incur considerable out-of-pocket costs because out-of-network bills are not included in federal mandates. “Surprise billing” articles are widespread in the research literature and lay press . To date, the frequency of unexpected patient costs for screening colonoscopy have yet to be rigorously quantified.”
This study with ~983,000 procedures, which was conducted between 2012-2017, shows that it is common to get additional charges from a screening colonoscopy (which is supposed to be covered). Despite using an in-network physician, these charges can be due to “out-of-network” costs from anesthesia or pathology. This can also occur when anesthesia bills the colonoscopy as a diagnostic procedure rather than as a screening procedure.


Related blog posts:

Abstract: Association Between Parent Comfort With English and Adverse Events Among Hospitalized Children
Key finding: Children of parents expressing LCE (limited comfort with English) had 2.1 higher odds of adverse events than children of parents who expressed comfort with English, after controlling for other factors.
Related blog post: No Habla Appendicitis