Tag Archives: Coronavirus
“Quietly” Testing Famotidine for COVID-19
Yesterday, I received two emails (first from Steven Liu) about an article in Science and today I’ve already seen this article is referenced in a CNN report:
New York Clinical Trial Quietly Tests Heartburn Remedy Against Coronavirus
Key points:
- In China, a review of ~6000 patients suggested lower mortality in those taking famotidine (not statistically significant)
- Famotidine may interfere with viral replication protease in the coronavirus based on computer modeling
- A randomized trial with IV famotidine (large quantities are not available) is underway in New York using 9 times the dose used for heartburn.
- The article notes that increased heart problems are common in those with reduced renal function
- “We still don’t know if it will work or not”
My take: Famotidine may be a hot commodity –at least until studies are completed. Based on experience with hydroxychloroquine, some of our patients may need to look for alternative acid blockers.
Related blog posts:
- NY Times: How Will We Know When to Reopen the Country? & Timely Tweets
- Hydroxychloroquine NOT Likely Effective
- COVID-19 Projections -IHME Data IHME Link: IHME Website for COVID-19 This post details the projected needs (ventilators, ICU beds) and projected mortality. Currently, peak of this pandemic in U.S. is anticipated to be April 16th.
- How to Do a Colonoscopic Polypectomy and U.S. COVID-19 Tracker NPR: Map: Tracking The Spread Of The Coronavirus In The U.S This tracker details the pandemic in every state.
- How to Protect Healthcare Workers from COVID-19 -Lessons from Hong Kong and Singapore Atul Gawande has a very pertinent article in the New Yorker: Keeping the Coronavirus from Infecting Health-Care Workers
- What is the Current Standard of Care for PPE and Endoscopy Cases? Link to manuscript: COVID-19 in Endoscopy: Time to do more?
- Bill Gates: What We Need to Do Now for COVID-19, False-negative testing & Article Describing 3 Stages of Infection From NY Times: If You Have Coronavirus Symptoms, Assume You Have the Illness, Even if You Test Negative Bill Gates: Here’s how to make up for lost time on covid-19 & article describing 3 stages of infection: COVD-19 Illness in Native and Immunosuppressed States: A Clinical-Therapeutic Staging Proposal
- Allocating Scarce Resources During COVID-19 Pandemic Links CDC Link: Testing for COVID-19 Full Link NEJM 2020 (Ezekial J Emmanuel et al): Fair Allocation of Scarce Medical Resources in the Time of Covid-19. This post also displays some data on sensitivity/specificity of testing
- Iron Injectables Links Financial Times: Coronavirus tracked: the latest figures as the pandemic spreads | Free to read & from Johns Hopkins: COVID19 Caseload & Outcomes Worldwide
- COVID-19: Veneto vs. Lombardy and Georgia’s Part of this Pandemic Link: Harvard Business Review: Lessons from Italy’s Response to Coronavirus & Georgia DPH: COVID-19 Daily Status Report
- “Crushing It” Two More Pediatric Hepatitis C studies Full link from NY Times: How Long Will Coronavirus Live on Surfaces or in the Air Around You? and blog post shows how to properly place PPE
- Ethical Dilemmas and Digestive Symptoms –Common with COVID-19 Full link: NEJM: Facing Covid-19 in Italy — Ethics, Logistics, and Therapeutics on the Epidemic’s Front Line & digestive symptoms ACG: Full Link: ACG Media Statement
- More Advice on Coronavirus for Pediatric GIs: NASPGHAN and CCFA CCFA Guidance for Pediatric Caregivers and Patients —Updates on COVID-19 and IBD
- Autoimmune Hepatitis Outcomes, Grand Rounds on Splenomegaly, Hydroxychloroquine for SARS-CoV-2 & Zantac Warning
- Liver Shorts and COVID-19 Screenshots This post includes Fauci donuts, AJG reference on COVID-19 digestive symptoms, and technology to sterilized used PPE
- New: NEJM link to video demonstrating need for PPE during intubation -see picture at bottom of post. Fluorescent Spray During Intubation and at the bottom -there is an image showing how hydroxychloroquine and azithromycin could increase risk for life-threatening arrhythmias
More Advice on Coronavirus for Pediatric GIs: NASPGHAN and CCFA
- Full link to CCFA Recommendations (from 3/11/20): Guidance for Pediatric Caregivers and Patients —Updates on COVID-19 and IBD
- Link to Johns Hopkins daily tracker: COVID19 Caseload & Outcomes Worldwide
- Link to New NASPGHAN/ICN COVID19/IBD worldwide registry: Can report cases at the following: SECURE-IBD Registry
- The Centers for Disease Control provides updates on the virus and safety information for the public and healthcare professionals. Here is a CDC Fact Sheet.
- The State Department provides a list of travel advisories for those who are planning to fly outside of the United States.
For Georgia:
- The State of Georgia has a new COVID-19 hotline. It can be reached by calling (844) 442-2681.
- The Georgia Department of health has put together a Daily Status Report which you can find here.
NASPGHAN statement regarding Coronavirus (SARS-CoV-2) Associated Infectious Disease (COVID -19) and Pediatric GI Patient Care and Providers.
Dear Members,
In view of the COVID -19 pandemic, care of our pediatric GI patients and at the same time our pediatric GI providers (i.e. physicians and other members of the healthcare team) is an utmost priority at NASPGHAN. NASPGHAN is working on several initiatives concurrently, and we are writing at this time to make you aware.
1. The Endoscopy Committee and the Clinical Practice Committee are working on a statement regarding elective procedures for pediatric GI patients with respect to this highly contagious pathogen, COVID to both preserve Personal Protective Equipment (PPE) as well as limit potential exposure.
2. A task force of leaders from NASPGHAN, ESPGHAN, LASPGHAN, and Asia (Hangzhou, China) will be writing a commentary to be published in the JPGN, our journal, with what COVID-19 means to the pediatric gastroenterologist.
3. Mike Kappleman of UNC, ICN, NASPGHAN and in particular the IBD Committee, are launching a prospective, real-time monitoring study of COVID-19 in IBD patients. The study is IRB and HIPAA approved and will link its data with that collected by the European Porto group’s study of coronavirus in IBD patients in Europe and Asia, thereby allowing an operational real-time active surveillance network for children and adolescents with IBD (our patients).
4. Jason Silverman, Jennifer Lee, and Peter Lu are putting together a special episode of the Bowel Sounds Podcast™ including relevant up-to-date guidelines and information about COVID-19 as it relates to our members and our patients.
5. The Endoscopy Committee and Clinical Practice Committee are working on information and options for telemedicine and virtual health, given the more recent announcement by CMS and the White House/President Trump in terms of changes in reimbursement given the coronavirus pandemic.
6. Within the next 24 hours, the NASPGHAN Website, as well as GIKids.org will house resources and links to the Centers for Disease Control and Prevention (CDC), the American Academy of Pediatrics (AAP), Crohn’s and Colitis Foundation (CCF), the Canadian Association of Gastroenterology (CAG) and the Joint GI Societies Statement (adult-based), including ASGE, ACG, AGA on Endoscopic procedures in the face of COVID-19.
7. Finally, please feel free to send us suggestions that would help our pediatric GI community work towards creative solutions during this time.
Sincerely,
Karen F. Murray MD
President, NASPGHAN
James Heubi MD
Past President, NASPGHAN
Benjamin Gold MD
President Elect, NASPGHAN
Jeannie S. Huang MD
Secretary Treasurer, NASPGHAN
Rina Sanghavi MD
Silent Anal Fistulas –Sounds Bad, Is It?
A recent prospective study (PH Kim et al. Clin Gastroenterol Hepatol 2020; 18: 415-23) with 440 consecutive adults (mean age 29.6 years) with Crohn’s disease (CD) identified asymptomatic anal fistulas with MRE (including anal MRI) studies. 36 patients were newly diagnosed and the remainder had established CD.
Key findings:
- In all of these patients, none of whom had clinical fistulas, an MRE identified “perianal tracts” in 53 (12%).
- 37 of 290 (12.8%) of patients without a perianal fistula history and 16 of 150 (10.7%) with a history of healed perianal fistula had perianal tracts identified on MRE
- No patients had any lesions that required treatment after examination by a surgeon
- MRE detection of asymptomatic tracts was independently associated with later need for perianal treatment: 17.8% cumulative incidence at 37 months (aHR 3.06)
My take: Abnormal perianal tracts on MRE in asymptomatic patients indicate an increased risk of developing clinically-significant perianal disease –though most do not.
More on COVID19:
- No children with IBD have been reported thus far from ESPGHAN which includes a 100 sites (mainly Europe) (as of March 10th); to report cases: ESPGHAN COVID19 Case Report Page
- There is some discussion that biologic therapy for IBD may have some protective effects
Could Immunotherapy (EPIT) Work For Eosinophilic Esophagitis? & Coronavirus Up-to-Date Tally
A recent double-blind pilot study (n=20) (JM Spegel et al. Clin Gastroenterol Hepatol 2020; 18: 328-36) explored the use of epicutaneous immunotherapy (EPIT) in children with milk-induced eosinophilic esophagitis (EoE). 15 children received active treatment with a “Viaskin” milk allergen extract patch and 5 children received a placebo.
The premise of EPIT for EoE has been based on animal models (mouse & piglet) which have shown that epicutaneous desensitization to peanuts has been successful in preventing development of EoE.
The design of the study involved EPIT during a 9 month milk-free period followed by a milk-containing diet for 2 months. Biopsies were taken and then there was an additional 11 month open-label phase in which all patients received EPIT.
Key findings:
- No significant differences in mean eos/hpf in the two groups: 50 vs 48 in EPIT compared to placebo respectively.
- There were 9 of 19 (47%) had a significant drop in eosinophil count with less than 15 eos/hpf at the end of the open-label phase.
- Overall, adverse events were similar in both groups, though the EPIT group had more frequent GI adverse events than the placebo group (67% vs. 40%)
My take: The primary and secondary endpoints were not reached in this study. However, based on the open-label phase response, further studies are warranted.
Related blog posts:
- New Therapy for Eosinophilic Esophagitis
- Grading Treatment Response in EoE
- Promising Biologic for Eosinophilic Esophagitis
- Transnasal Endoscopy (Unsedated) for EoE
- How Genetics Influence Response Rate to PPIs in EoE
- Association and Causation: Early Life Risk Factors for Eosinophilic Esophagitis
- Negligible Effect of Eosinophilic Esophagitis Treatment on Longitudinal Growth
- Increased Risk of EoE with TEF/EA
- What is EoE?
- EoE Update 2018 (Dr. Seth Marcus)
- Updated Consensus Guidelines for Eosinophilic Esophagitis
- Time to Diagnosis in Eosinophilic Esophagitis
- Adrenal Insufficiency due to Fluticasone in EoE
- Higher Doses of Topical Steroids for Eosinophilic … – gutsandgrowth
Also, from Johns Hopkins: COVID19 Caseload & Outcomes Worldwide
AAP Behind the Scenes 2020 (Part 1): Pandemic Monitoring
Currently I am vice chair for the section of nutrition at the Georgia Chapter of the American Academy of Pediatrics; Dr. Tanya Hofmekler is now chair of the section. I recently attended a Board Meeting which received reports from a number of committees. One of the presentations from Dr. Evan Anderson (infectious disease specialist), provided an update on the coronavirus, the flu, and other emerging infections.
Key Points:
- Coronavirus appears to be more contagious than the flu but less contagious than many other infections like measles
- CDC has website which is update for the coronavirus which is updated frequently: 2019 Novel Coronavirus (2019-nCoV) Situation Summary
- This is a bad year for the flu (see “red line” on last two slides). The number of hospitalizations/mortality in young children (0-4) is increased compared to previous years, though the number of cases has been higher in previous years
- There is now an FDA-approved Ebola vaccine
- A single case of measles can cost $50,000 for public health to respond; direct medical costs could be much higher
Related blog post:
The Best Information We Have To Date on the Emerging Coronavirus
The NEJM has made the information it has on the emerging coronavirus open access. Here are the links:
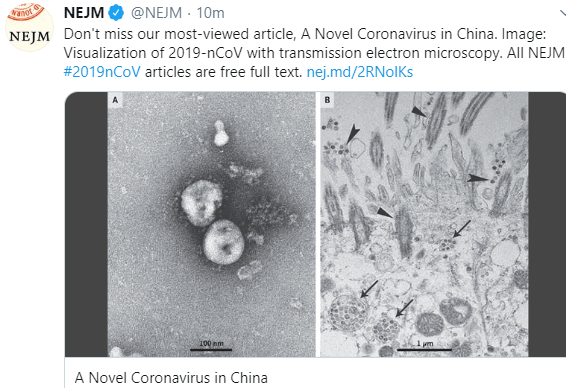
- NEJM: A Novel Coronavirus from Patients with Pneumonia in China, 2019
- NEJM: Perspective: A Novel Coronavirus Emerging in China — Key Questions for Impact Assessment
- NEJM: Editorial: Another Decade, Another Coronavirus
- Also, in depth coverage from the NY Times: What is the Coronavirus? Symptoms, Treatment, and Risks
An excerpt from the editorial:
For the third time in as many decades, a zoonotic coronavirus has crossed species to infect human populations. This virus, provisionally called 2019-nCoV, was first identified in Wuhan, China, in persons exposed to a seafood or wet market. The rapid response of the Chinese public health, clinical, and scientific communities facilitated recognition of the clinical disease and initial understanding of the epidemiology of the infection. First reports indicated that human-to-human transmission was limited or nonexistent, but we now know that such transmission occurs, although to what extent remains unknown. Like outbreaks caused by two other pathogenic human respiratory coronaviruses (severe acute respiratory syndrome coronavirus [SARS-CoV] and Middle East respiratory syndrome coronavirus [MERS-CoV]), 2019-nCoV causes respiratory disease that is often severe.1 As of January 24, 2020, there were more than 800 reported cases, with a mortality rate of 3%…
Both SARS-CoV and MERS-CoV infect intrapulmonary epithelial cells more than cells of the upper airways.4,6 Consequently, transmission occurs primarily from patients with recognized illness and not from patients with mild, nonspecific signs. It appears that 2019-nCoV uses the same cellular receptor as SARS-CoV (human angiotensin-converting enzyme 2 [hACE2]),3 so transmission is expected only after signs of lower respiratory tract disease develop…
It is likely that 2019-nCoV will behave more like SARS-CoV and further adapt to the human host, with enhanced binding to hACE2.