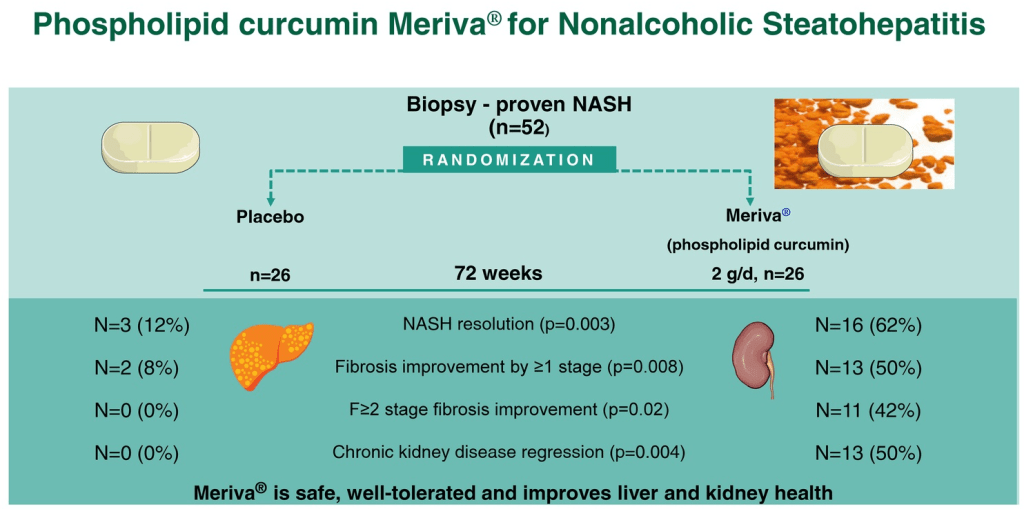
G Musso et al. Hepatology 2025; 81: 560-575. Effect of phospholipid curcumin Meriva on liver histology and kidney disease in nonalcoholic steatohepatitis: A randomized, double-blind, placebo-controlled trial
“Let food be thy medicine” is a well-known phrase usually attributed to Hippocrates (though it is unclear if he said this). Regardless, this study indicates that added curcumin in the diet could be beneficial for steatotic liver disease.
Methods: In this double-blind trial, 52 patients with biopsy-proven NASH (71% with stage ≥F2 fibrosis, 58% with stage A2-G2/A2-G3a chronic kidney disease) were randomized 1:1 to receive Meriva 2 g/d (1 g BID) or placebo for 72 weeks. Meriva is a formulation of curcumin extract with phospholipids that has improved oral bioavailability of curcumin metabolites.
Key findings:
- Sixteen (62%) patients on Meriva (curcumin) versus 3 (12%) patients on placebo had NASH resolution (RR = 5.33)
- hirteen (50%) patients on Meriva versus 2 (8%) patients on placebo had ≥1 stage fibrosis improvement (RR = 6.50)
- Eleven (42%) patients on Meriva versus 0 (0%) on placebo had regression of significant liver fibrosis (RR = 18.01)
- Thirteen (50%) patients on Meriva versus 0 (0%) on placebo had chronic kidney disease regression (RR = 10.71)
- Compared with placebo, Meriva improved eGFR (difference in adjusted eGFR change: +3.59 [2.96–4.11] mL/min/1.73 m2/y, p = 0.009), fasting glucose(−17 mg/dL; 95% CI = −22, −12), HbA1c (−0.62%; 95% CI = −0.87%, −0.37%), LDL-C (−39 mg/dL; 95% CI = −45, −33), triglycerides (−36 mg/dL, 95% CI = −46, −26), HDL-C (+10 mg/dL; 95% CI = +8, +11), and inflammatory markers
- The observed benefits were associated with downregulation of hepatic NF-kB which is a proinflammatory transcription factor and a known curcumin target
My take: A larger multicenter study is needed to confirm these promising results. This study shows that dietary changes and lifestyle modification remain important tools in treating MASH (aka NASH).
Related editorial (open access!): S Zelber-Sagi, JM Schattenberg. Hepatology 2025; 81: 399-401. Is curcumin the new kid on the block for the treatment of MASH?
Related blog posts:
- Pharmacological Management of Pediatric Steatotic Liver Disease
- Non-Invasive Studies Often Fail to Detect Advanced Liver Fibrosis in Steatotic Liver Disease
- You No Longer Have Fatty Liver Disease-You Have Steatotic Liver Disease!
- AASLD Practice Changes for Metabolic Liver Disease in 2024
- Semaglutide in Adolescent Obesity
- Survodutide, Dual Glucagon Receptor/GLP-1 Receptor Agonist, for MASH (Phase II Trial)
- Tirzepatide for Metabolic Dysfunction–Associated Steatohepatitis (MASH) & Uptick in GLP1 Use
- Pharmacotherapy for Obesity
- Fibrosis and Steatotic Liver Disease -Who Needs to be Followed by Hepatology?
- Prevalence of Steatotic Liver Disease in U.S. And Risk of Complications
- Three-fer on Steatotic Liver Disease
- Bad Fatty Liver Disease Can Get Worse Quickly
- Semaglutide Keeps Weight Off at Four Year Mark
- How Many Kids Would Be Good Candidates for Bariatric Surgery?
- Fatty Liver Disease AASLD Practice Guidance 2023
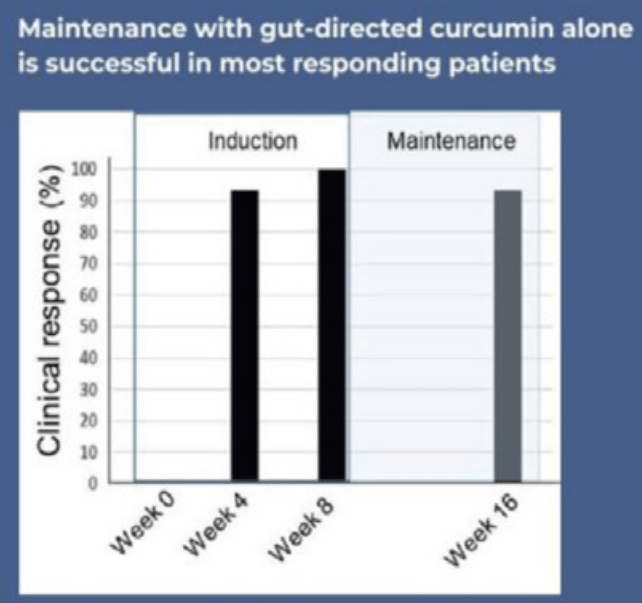
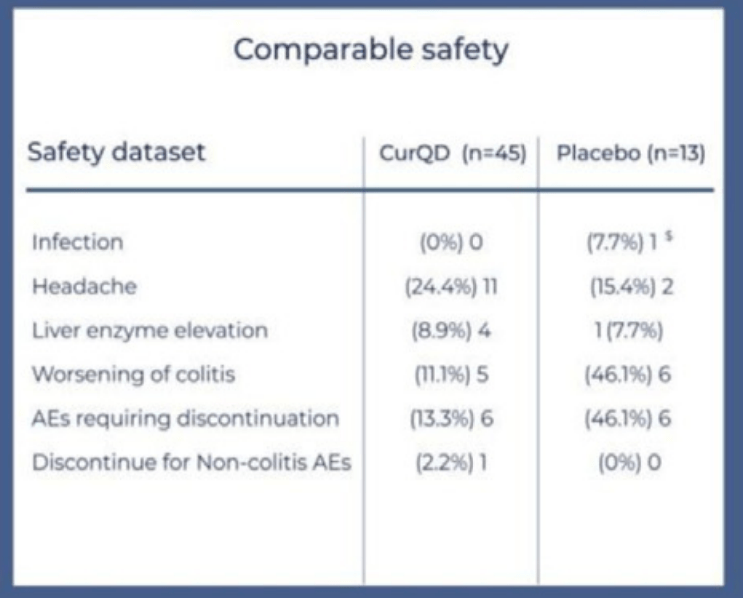
- Spice It Up! Curcumin for Ulcerative Colitis (2024)
- Spice It Up? Curcumin for Ulcerative Colitis (2015)
Disclaimer: This blog, gutsandgrowth, assumes no responsibility for any use or operation of any method, product, instruction, concept or idea contained in the material herein or for any injury or damage to persons or property (whether products liability, negligence or otherwise) resulting from such use or operation. These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. Because of rapid advances in the medical sciences, the gutsandgrowth blog cautions that independent verification should be made of diagnosis and drug dosages. The reader is solely responsible for the conduct of any suggested test or procedure. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition.