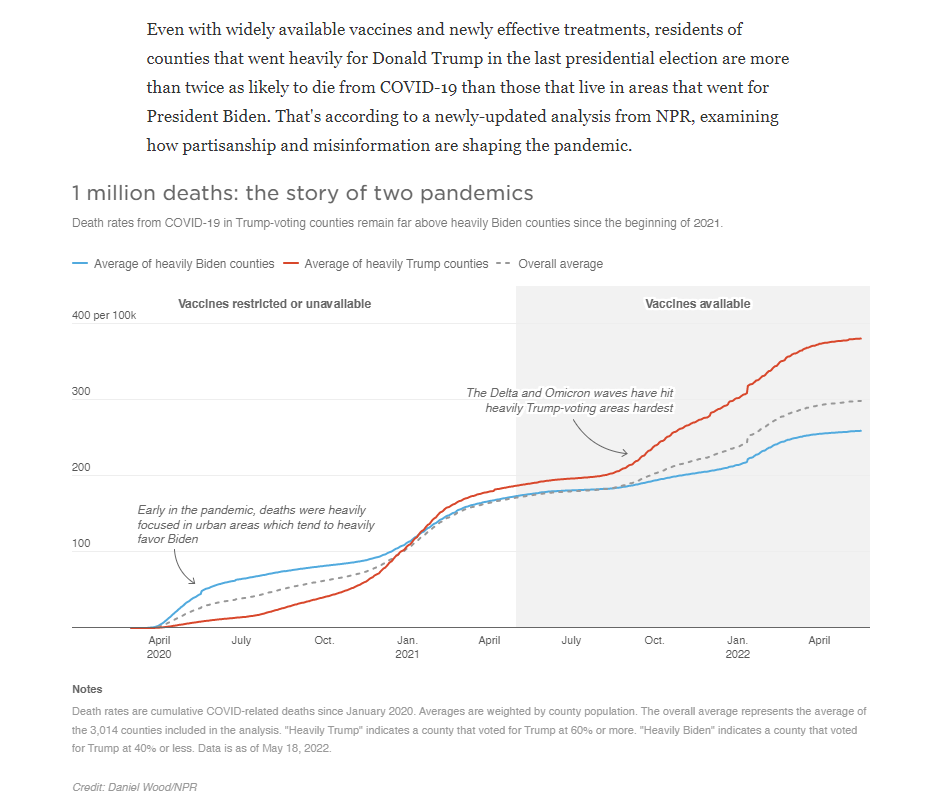
NY Times article: U.S. Coronavirus Cases Are Rising Sharply, but Deaths Are Still Down
This article explains why deaths from COVID-19 have not increased despite increasing number of infections. Three main reasons: increased testing -detects many with less severe symptoms, younger population are being infected, and new treatment approaches may be helping. However, “the dip in coronavirus mortality will not necessarily last. As more people socialize, those with milder infections might end up ferrying the pathogen to vulnerable individuals…Recent upswings in coronavirus case numbers leave experts apprehensive of what’s to come. Death, when it occurs, tends to trail infection by about two to four weeks.”
The Budesonide Oral Suspension (BOS) resulted in 62% of BOS patients meeting the threshold of < 15 eos/hpf compared to 1% of placebo patients. From lead author, Ikuo Hirano: “the results of the BOS trial showed that BOS successfully treated both the symptoms and signs of EoE. The positive results will hopefully lead to an approved, safe and effective therapy for EoE.”
Abstract from ACG Meeting October 2019:
Abstract: Efficacy of Budesonide Oral Suspension for Eosinophilic Esophagitis in Adolescents and Adults: Results From a Phase 3, Randomized, Placebo-Controlled Trial
Introduction: Eosinophilic esophagitis (EoE) is a chronic immune-mediated disease for which there is an unmet clinical need for new therapies. The safety and efficacy of budesonide oral suspension (BOS) for the treatment of EoE has been demonstrated in a previous phase 2 study. The current phase 3 study evaluated the efficacy and safety of BOS in a large cohort of patients with EoE.
Methods: This randomized, double-blind, placebo-controlled trial (SHP621-301; NCT02605837) investigated the safety and efficacy of BOS in patients (11–55 years) with EoE and dysphagia. Patients were randomized 2:1 to 2.0 mg BOS or placebo twice daily (b.i.d.) for 12 weeks (Figure 1). Co-primary endpoints were histologic (peak eosinophil count ≤6 eosinophils/high-powered field [eos/hpf]) and dysphagia symptom (≥30% decrease in symptoms as measured by the Dysphagia Symptom Questionnaire [DSQ]) responses after 12 weeks of therapy. Secondary endpoints included change in DSQ score and change in EoE Endoscopic Reference Score (EREFS) from baseline to final treatment period. Safety was also assessed.
Results: A total of 322 patients were randomized (BOS, n=215; placebo, n=107), of whom 318 patients received at least one dose of double-blind therapy (BOS, n=213; placebo, n=105) (Table). The primary outcomes were achieved, with significantly more histologic and symptom responders in the BOS-treated than the placebo-treated group (53.1% vs 1.0%, p< 0.001; 52.6% vs 39.1%, p=0.024, respectively; Figure 2). Improvements in mean DSQ score from baseline to week 12 were significantly greater in the BOS group (n=197) than the placebo group (n=89) (−13.0 vs −9.1; p=0.015). Similarly, improvements in mean EREFS scores were significantly greater with BOS (n=202) than placebo (n=93) (−4.0 vs −2.2; p< 0.001). In total, 61.0% of patients reported a treatment-emergent adverse event (TEAE) (BOS, 61.0%; placebo, 61.0%). Only 2.5% of patients experienced a TEAE leading to dose discontinuation (BOS, 1.4%; placebo, 4.8%). Few patients had severe or serious TEAEs on BOS or placebo. No life-threatening TEAEs were reported.
Discussion: This phase 3 trial demonstrated the efficacy of BOS as induction therapy for EoE. BOS resulted in significant improvements in histologic, symptomatic and endoscopic endpoints compared with placebo. The majority of TEAEs were mild to moderate and comparable between placebo and BOS. A double-blind, placebo-controlled maintenance study (SHP621-302) is ongoing.
Related blog posts:

Island Ford, Sandy Springs