A recent review article, “The Imperative for Climate Action to Protect Health,” (A Haines, K Ebi. NEJM 2019; 380: 263-73, and commentary 209-11) explains why many brilliant minds are so concerned about our climate.
What is happening to our climate:
- “Climate change is already adversely affecting human health…if no additional actions are taken, then over the coming decades, substantial increases in morbidity and mortality are expected.”
- “August 2018 was the 406th straight month during which global mean temperatures were above the long-term mean.”
- “Carbon dioxide (the primary greenhouse gas) have risen from approximately 280 ppm in preindustrial times to approximately 410 ppm today. Carbon dioxide remains in the atmosphere for centuries, with about 20% persisting for more than 1000 years.”
- “The global mean temperature is currently increasing at a rate of 0.2 degrees C per decade owing to past and continuing emissions.”
Health Consequenes:
- Major climate events including heat waves, floods, rising sea levels, droughts and storms with their immediate and long-term effects of health: heat-related illnesses, fatalities, injuries, and mental health effects
- Worsened air quality: asthma and COPD exaccerbations, worsened cardiovascular outcomes
- Water-borne illnesses due to effects on water quality: cholera, campylobacter infection, algae blooms, cryptosporidium, leptospirosis are some examples
- Disruption of food supply and safety –heat can interfere with soil moisture and crop yield: malnutrition
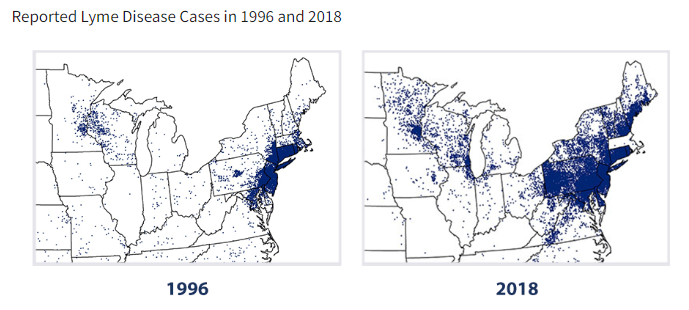
- Proliferation of vector-related illnesses: zika virus, dengue, lyme disease, malaria to name a few
- Social: flooding and heat are likely to lead to social upheaval, mass migration, and violent conflicts
Even if all of the goals of the Paris Agreement were honored by all of the signatories, “it would not be sufficient to limit warming to 2 degree C above preindustrial levels…[it] would be expected to result in a temperature increase of approximately 3.2 degree C by the year 2100, relative to the preindustrial period.”
The authors cite estimates that mitigating adverse climate effects could prevent more than 175,000 premature deaths and 22,000 fewer deaths annually by 2030.
The associated commentary link the recent destructive California wildfires to climate change. They note that “tackling this challenge may feel overwhelming.” Working on this can include both individual lifestyle actions and institutional efforts.
Individual actions:
- Walking/cycling more
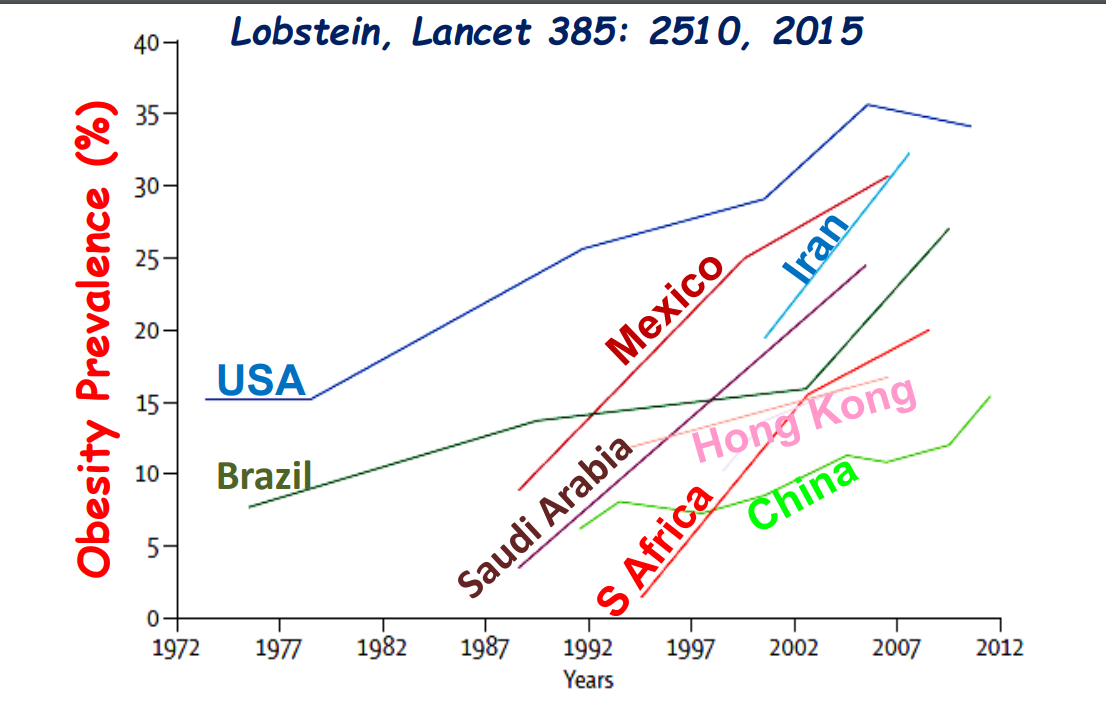
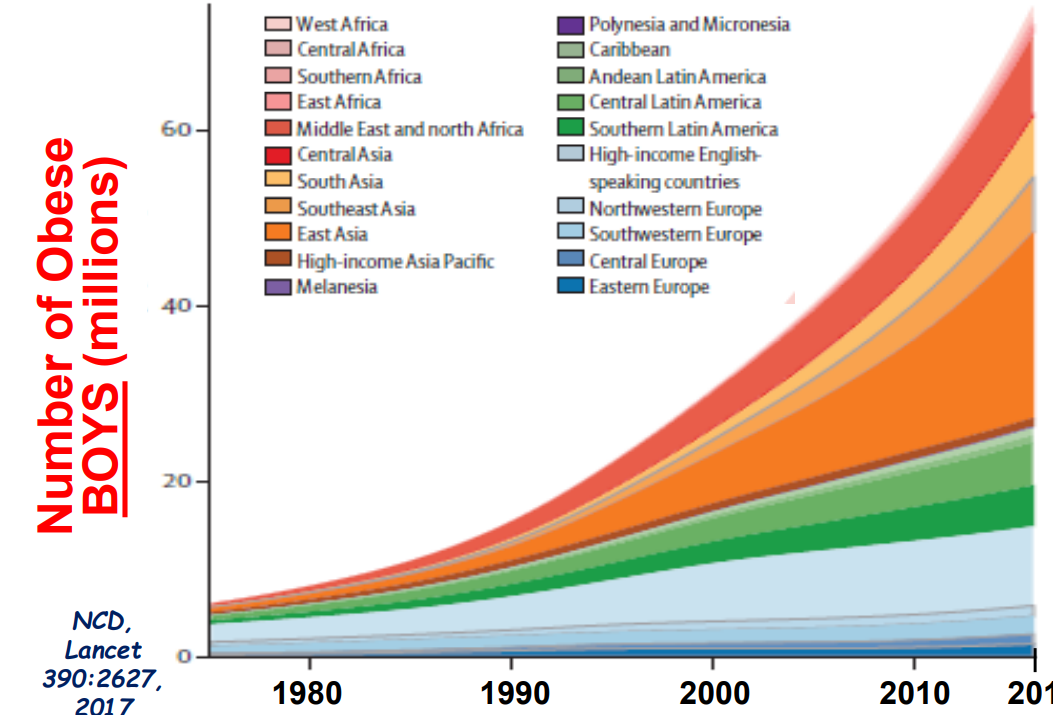
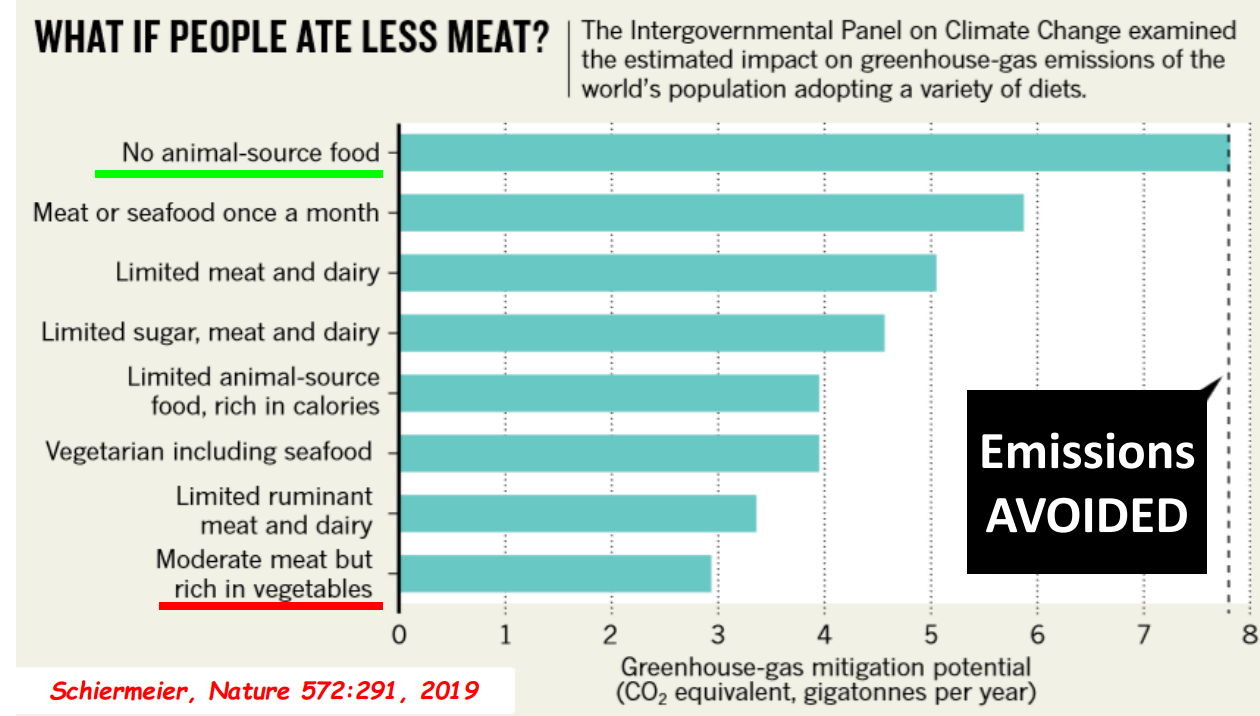
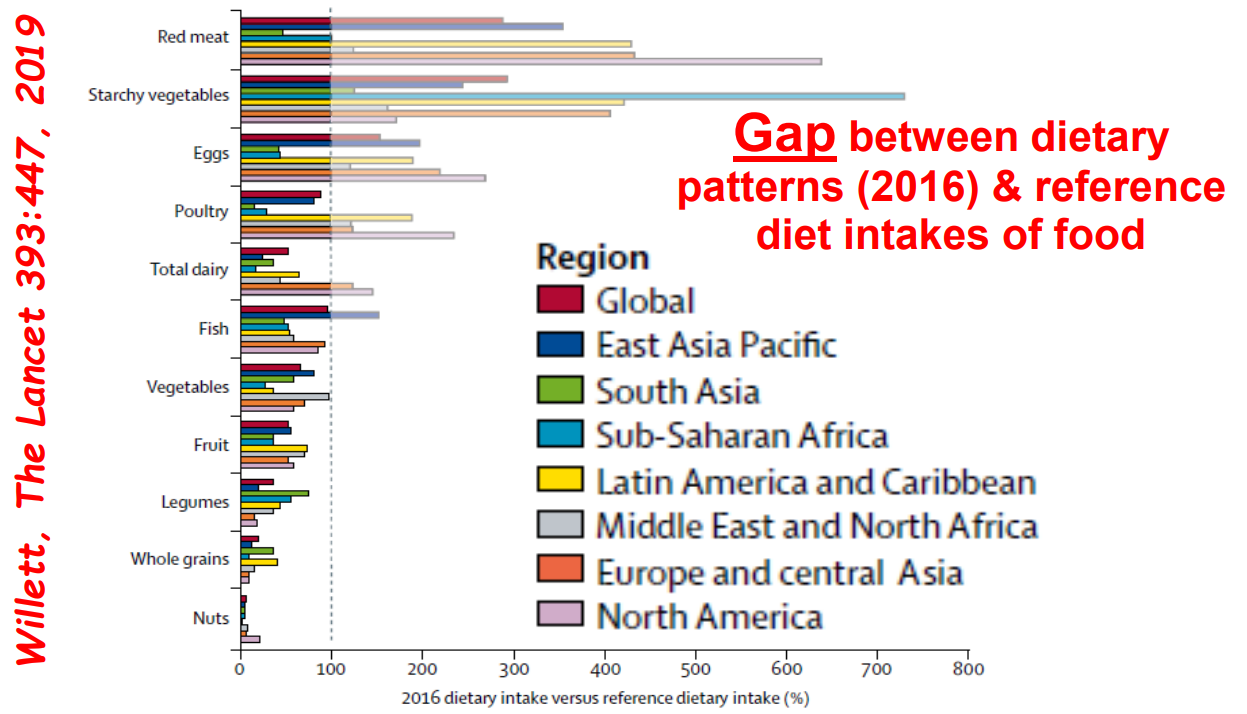
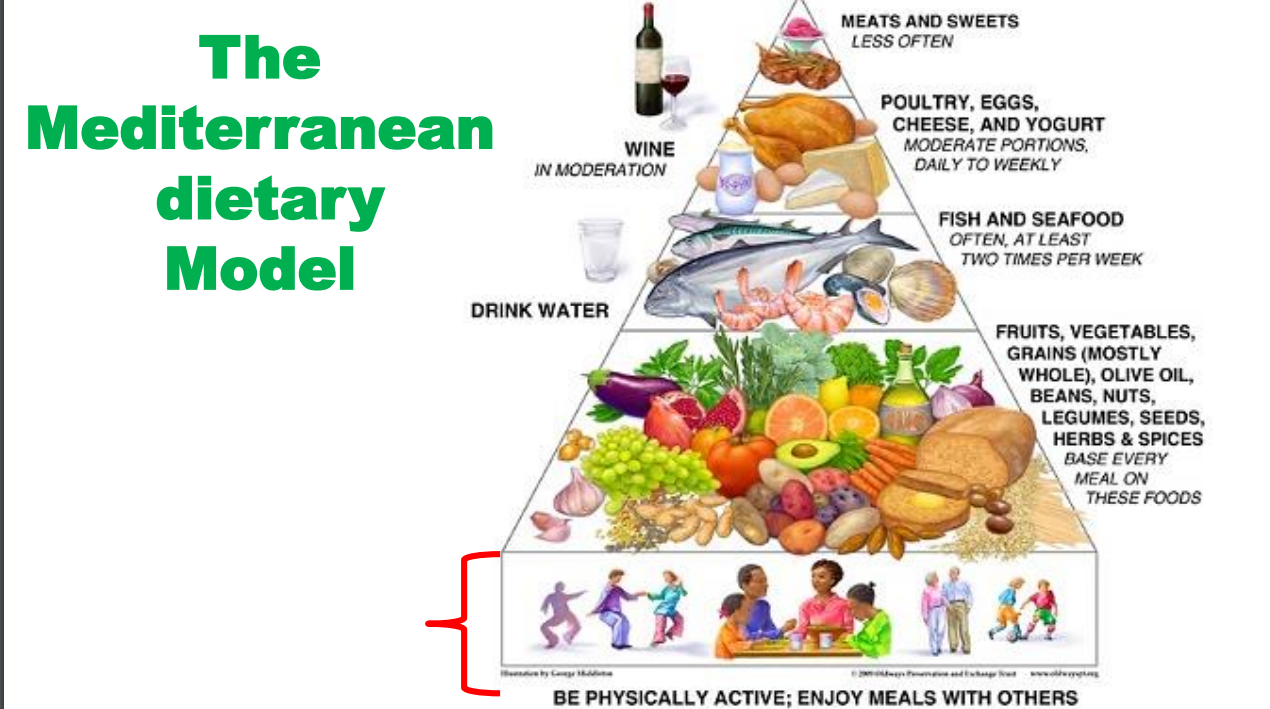
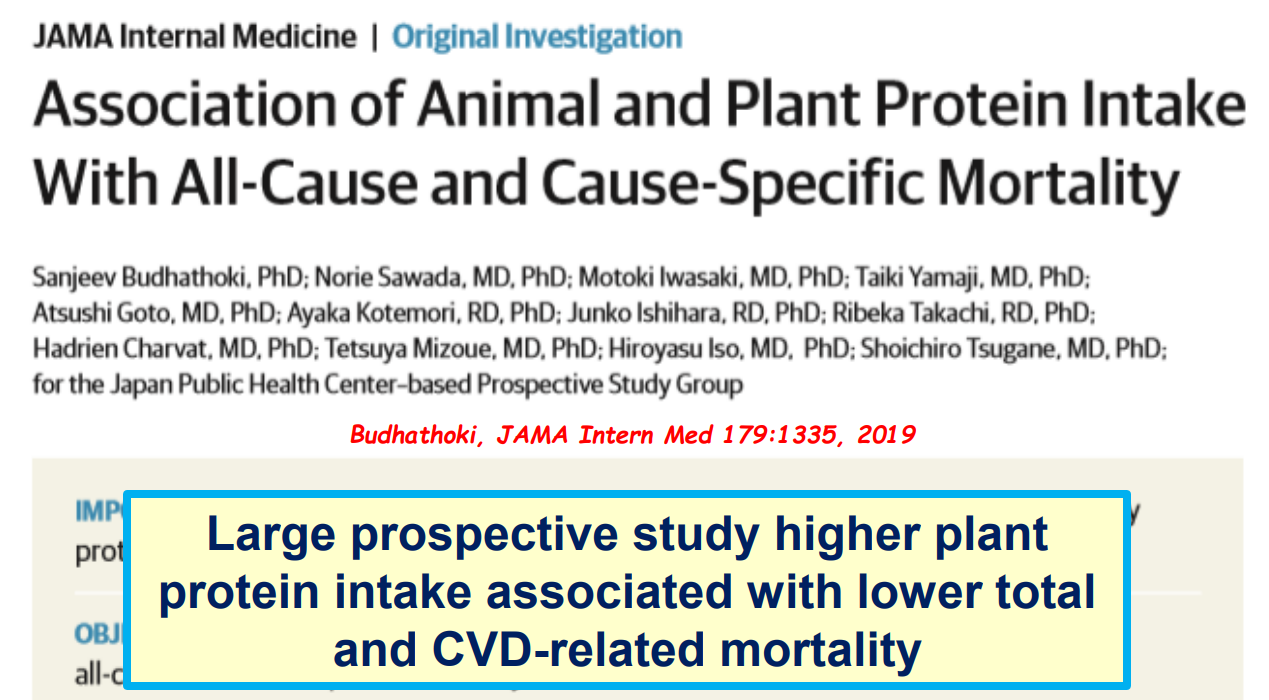
- Eating less meat
- Reducing food waste
- Conserving energy
Institutional actions:
- Health care system accounts for 1/10th of greenhouse gas emissions and health systems need to work on cutting their emissions
- Health care institutions can invest/divest in industries who are helping and harming efforts to limit fossil fuel consumption
Resources:
From review article by Haines and Ebi: “Health professionals have leading roles to play in addressing climate change. They can support health systems in developing effective adaptation to reduce the health risks of climate change, promote healthy behaviors and policies with low environmental impact.”
My take: Interestingly, the issue of delay in addressing problems is discussed in an unrelated commentary (NEJM 2019; 380: 118-9) related to denial. For the author, she was attempting to deny the possibility that her father had ALS. At the end, she quotes Elisabeth Kubler-Ross: “Denial helps us to pace our feelings of grief. There is a grace in denial. It is nature’s way of letting in only as much as we can handle.” Clearly, much of the world remains in denial of the necessitiy to address climate change.
Related blog post:

Badwater Basin, Death Valley -salt-covered dried up basin