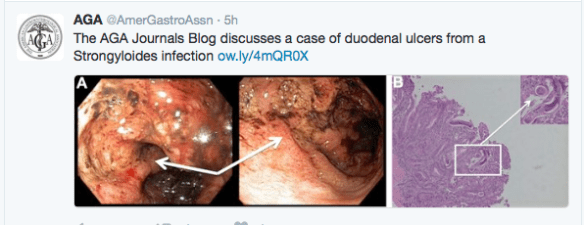
- 6-Mercaptopurine (6-MP) often can be used when patients are intolerant of azathioprine. S Hubener et al. Clin Gastroenterol Hepatol 2016; 14: 445-53. This retrospective study showed that 15 of 20 patients with autoimmune hepatitis and prior azathioprine intolerance responded to 6-MP. This is somewhat unexpected as azathioprine is metabolized into 6-MP. However, rather than 6-thiouracil, the “imidazol component of azathioprine, which is cleaved off…might trigger adverse reactions.” Another artical on thiopurines (Aliment Pharmacol Ther 2016; 43: 863-883) (thanks to Ben God for this reference) provides a thorough review of the pharmacogenetics and pharmocokinetics of these medications. While this review reinforces the recommendation to check TPMT before treatment, it notes that only a small proportion of thiopurine toxicity is related to deficient TPMT activity.
- There is no formal validated or consensus definitions of mild, moderate, or severe IBD. L Peyrin-Biroulet et al. Clin Gastroenterol Hepatol 2016; 14: 348-54. While the Lemann index measures the cumulative structural bowel disease, the authors propose criteria which involves three areas of severity: impact of the disease on the patient (eg. clinical symptoms), inflammatory burden (eg. biomarkers, mucosal disease, disease extent), and disease course (eg. structural disease, intestinal resection, perianal disease, extraintestinal manifestations)
- Fundic gland polyps (often associated with proton pump inhibitor therapy) are not premalignant lesions. There is an “inverse correlation between the FGPs and gastric neoplasia.” S Varghese et al. Gastroenterol Hepatol; 2016; 12: 153-4.
- Parents of newborns do not know how to use car seats. BD Hoffman et al (J Pediatr 2016; 171: 48-54) showed that 95% of car seats were misused (291 families). Serious misuse was present in 91%.
Related blog posts: Lemann index: Short Takes on IBD Articles | gutsandgrowth