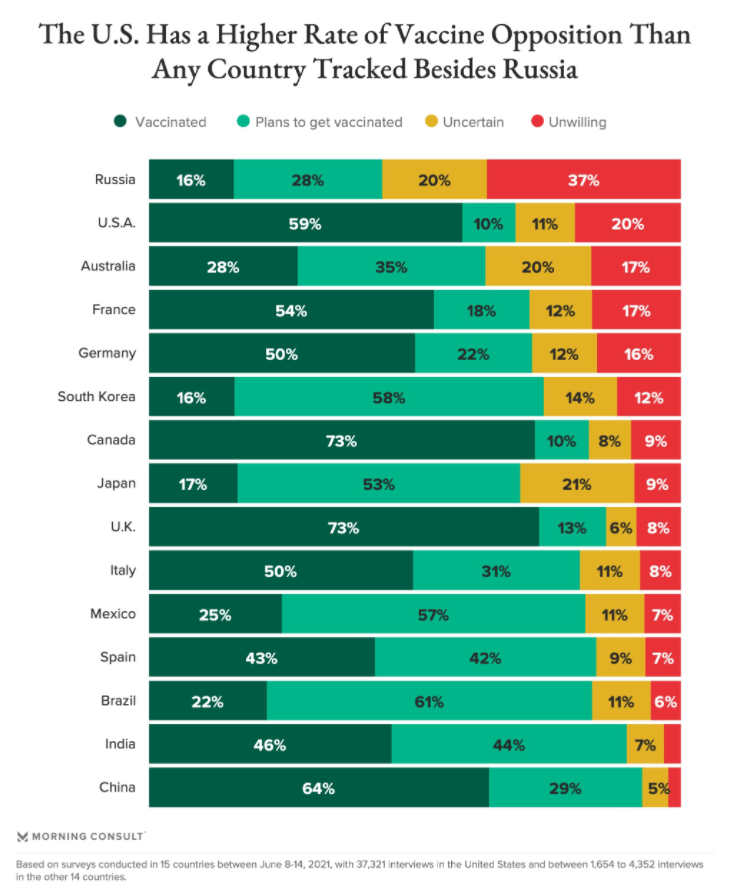
From AJC, Hashem Dezhbakhsh: An incentive to encourage vaccination
This is a good read. An excerpt:
Vaccine hesitancy, which can prolong the pandemic, is a textbook example of a negative consumption externality, where an individual’s choice can harm or impose costs on others. Indoor smoking, drunk driving, or littering are other examples…
One policy option is to use the insurance mechanism, with risk assessment and risk pricing as its enforcing arms….
For example, a risky driver has a higher auto insurance premium than a safe driver, a smoker has a higher health insurance premium than a non-smoker,…Similarly, health insurance premiums, deductibles, and co-pays can be set higher for those who are unvaccinated...
Using risk pricing to set insurance premiums and co-pays for these individuals makes good sense and is fair policy. It incentivizes individuals to vaccinate, while also providing a fairer insurance pricing system by charging those with self-selected higher risk a higher price, instead of shifting their medical costs to others through uniform insurance pricing.