TL Hedrick et al. Clin Gastroenterol Hepatol 2023; 21: 2473-2477. Open Access! AGA Clinical Practice Update on Management of Ostomies: Commentary
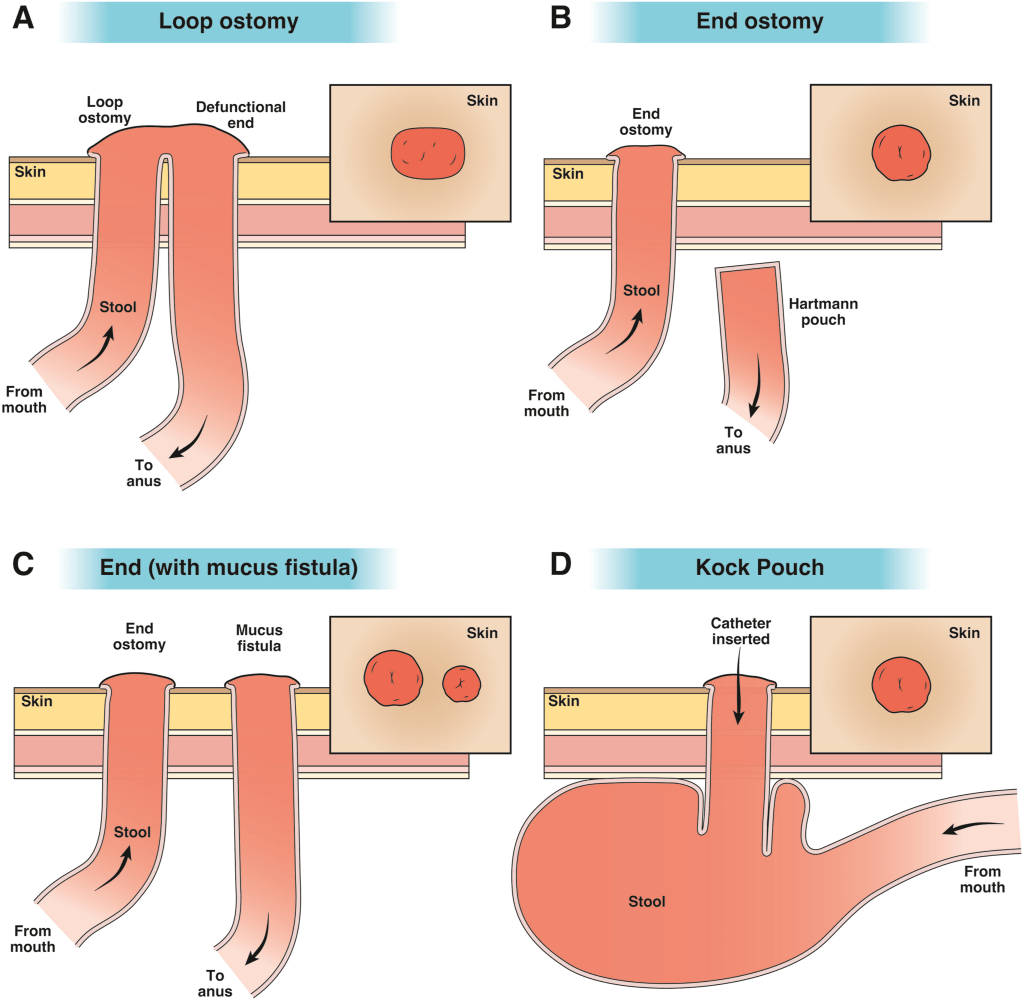
This article is a helpful review on ostomy care. The article reviews approaches to common problems including early high ostomy output, ostomy leakage, stoma retraction, mucocutaneous separation, dermatological problems, chronic high ostomy output, parastomal hernia, and stoma prolapse. A few of their comments:
- “An estimated 750,000 Americans live with an ostomy and 130,000 new ostomy surgeries occur in the United States annually.1“
- “Reversal [of ostomy] before 6 weeks of the index surgery is associated with an increased risk of complications”
- For leakage of ostomy: “Management steps involve thickening the stool with antidiarrheals to facilitate a more solid effluent and pouching techniques to bolster the height of the stoma off the peristomal skin (eg, convex appliance, ostomy belt, paste, or barrier rings). Each of these items is available through the patient’s medical equipment supplier. Additional pearls include heating the appliance with a hair dryer before application, lying flat for several minutes after application, ensuring the peristomal skin is dry before application, and use of a fine dusting of stomal powder followed by skin sealant on the peristomal skin before application.”
- Stoma prolapse: “The rate of stomal prolapse is 5% to 10%.12 Acute prolapse can lead to incarceration and ischemia, which presents as pain, obstipation, and purple/black discoloration of the stoma…In the absence of ischemia, the prolapse may be reduced by laying the patient in a relaxed position and gently squeezing the ostomy back into the abdomen. If the stoma cannot be reduced with pressure alone, a cup of sugar applied directly to the stoma and left in place for 20 minutes can reduce stomal swelling and facilitate reduction of the prolapse. Surgery can be avoided if the prolapse is mild, easily reducible, and does not interfere with pouching.”
- Medications for High Ostomy Output include bulking agents (fiber, guar gum, marshmellows), antimotility agents (eg. loperamide, diphenoxylate/atropine), and antisecretory agents (PPIs, Octreotide). Treatment of specific underlying disease may help, such as anti-inflammatory agents for IBD and GLP-2 analogues for short bowel.
Related blog posts:
Disclaimer: This blog, gutsandgrowth, assumes no responsibility for any use or operation of any method, product, instruction, concept or idea contained in the material herein or for any injury or damage to persons or property (whether products liability, negligence or otherwise) resulting from such use or operation. These blog posts are for educational purposes only. Specific dosing of medications (along with potential adverse effects) should be confirmed by prescribing physician. Because of rapid advances in the medical sciences, the gutsandgrowth blog cautions that independent verification should be made of diagnosis and drug dosages. The reader is solely responsible for the conduct of any suggested test or procedure. This content is not a substitute for medical advice, diagnosis or treatment provided by a qualified healthcare provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a condition.